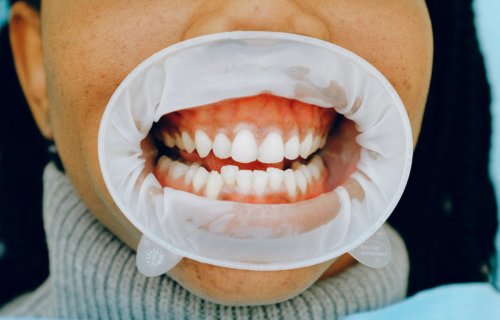
SEATTLE, Wash. — As far as dentists are concerned, bleeding gums are usually an early warning sign of gingivitis or other gum infections. However, a new study finds this unsettling dental condition may also reveal a problem with your diet. Researchers from the University of Washington say bleeding gums may be sign someone is lacking vitamin C in their diet.
The study finds bleeding of the gums, and even bleeding in the eye, has a link to low vitamin C levels in the bloodstream. Researchers discovered that increasing daily intake of vitamin C in people with low plasma levels helps reverse this bleeding problem.
They add both gum bleeding tendency and retinal hemorrhaging could be a sign of general trouble in a patient’s microvascular system. It may also point to microvascular bleeding in the brain, heart, and kidneys.
Bleeding gums is normally connected with gingivitis or periodontitis, both forms of serious gum disease. Dentists regularly tell patients to make sure they are brushing and flossing their teeth twice a day if they have these symptoms. The new report suggests adding sources of vitamin C, such as oranges and strawberries, may also be as important as improving dental hygiene.
“When you see your gums bleed, the first thing you should think about is not, I should brush more,” lead study author Philippe Hujoel says in a university release. “You should try to figure out why your gums are bleeding. And vitamin C deficiency is one possible reason.”
Do certain diets lead to less vitamin C?
The study stresses that reversing gum bleeding by increasing vitamin C does not necessarily prevent strokes or other serious health outcomes. However, the results do suggest that vitamin C recommendations designed to protect against scurvy – a deadly disease caused by extremely low vitamin C levels – are too low. Researchers add such low vitamin C levels can lead to bleeding, which should not be treated with dental floss.
As a result, Prof. Hujoel recommends people try to keep an eye on their vitamin C intake through non-processed foods such as kale, peppers, or kiwis. If you can not find palatable foods rich in vitamin C, consider a supplement of about 100 to 200 milligrams a day.
If someone is on a specialized diet, such as a paleo diet rich in lean meats, fish, fruits, vegetables, nuts, and seeds, it is important that they take a look at their vitamin C intake.
“Vitamin C-rich fruits such as kiwis or oranges are rich in sugar and thus typically eliminated from a low-carb diet,” the practicing dentist and professor of oral health sciences adds.
Scientists say people who exclusively eat lean meats and avoid vitamin-rich organ meats may be at a particularly high risk for vitamin C deficiency.
Bleeding gums and vitamin C have a long history
Researchers note the link between gum bleeding and vitamin C levels was first recognized more than 30 years ago. Two studies co-authored by former dean of the UW School of Dentistry Paul Robertson – published in 1986 and 1991 – identified gum bleeding as a biological marker for vitamin C levels. This connection somehow got lost in dental conversations concerning bleeding gums, the researchers say.
“There was a time in the past when gingival bleeding was more generally considered to be a potential marker for a lack of vitamin C,” Prof. Hujoel explains. “But over time, that’s been drowned out or marginalized by this over-attention to treating the symptom of bleeding with brushing or flossing, rather than treating the cause.”
The Washington team analyzed studies of 15 clinical trials in six countries. These reports involved 1,140 predominantly healthy participants and data from 8,210 U.S. residents surveyed in the Centers for Disease Control and Prevention’s Health and Nutrition Examination Survey.
“Retinal hemorrhaging and cerebral strokes are associated with increased gingival bleeding tendency, and that (vitamin C) supplementation reverses the retinal bleeding associated with low (vitamin C) plasma levels,” Prof. Hujoel’s review concludes.
“A default prescription of oral hygiene and other periodontal interventions to ‘treat’ microvascular pathologies, even if partially effective in reversing gingival bleeding as suggested in this meta-analysis, is risky because it does not address any potential morbidity and mortality associated with the systemic microvascular-related pathologies,” study authors write.
The study appears in the journal Nutrition Reviews.
SWNS writer Chris Dyer contributed to this report.