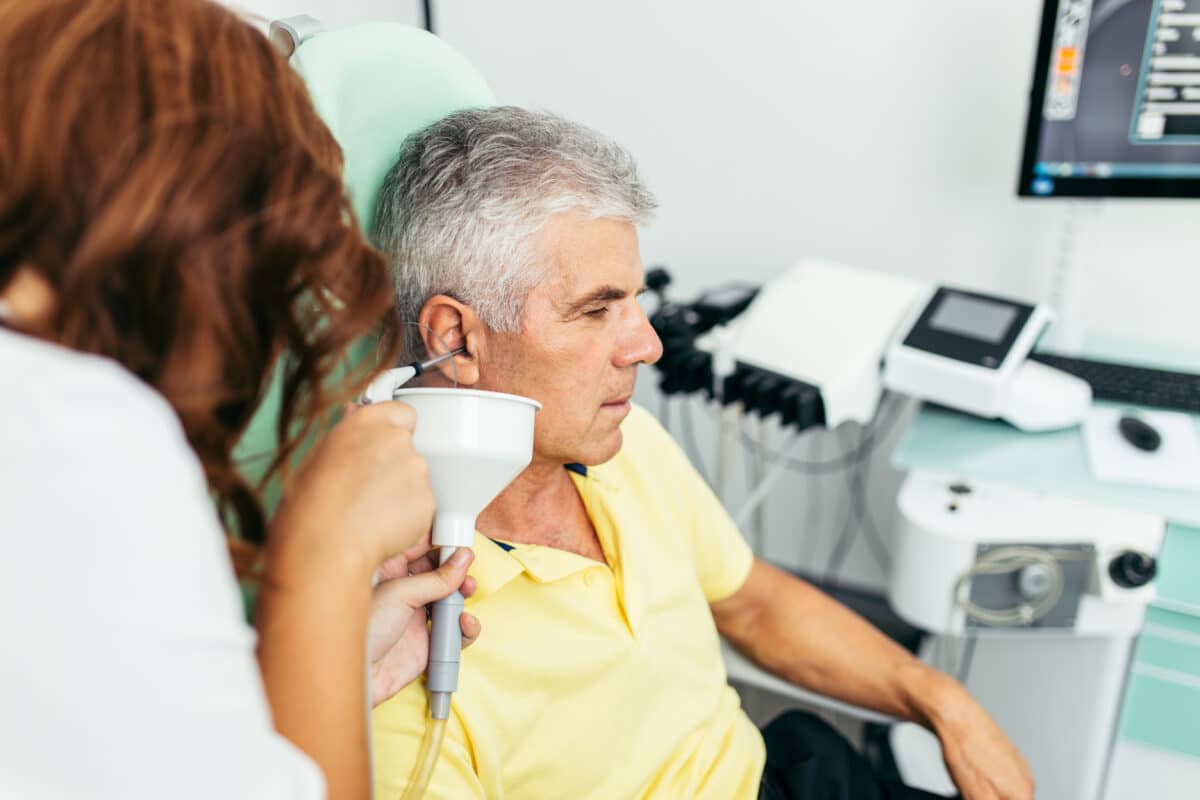
Doctor performing ear irrigation and earwax removal on patient. (Photo by DuxX on Shutterstock)
In a nutshell
- Chinese researchers developed an AI system that can detect Parkinson’s disease by analyzing earwax with 94.4% accuracy
- The technology identifies four specific chemical compounds in ear canal secretions that differ between Parkinson’s patients and healthy individuals
- This breakthrough could enable faster, cheaper screening for Parkinson’s disease in primary care settings
ZHEJIANG, China — Parkinson’s disease affects millions worldwide, yet current diagnostic methods often catch the condition too late for optimal treatment. By the time most patients receive their diagnosis, they’ve already lost substantial numbers of dopamine-producing brain cells. Chinese researchers may have found a solution in an unexpected place: earwax.
Their new study, published in Analytical Chemistry, shows that artificial intelligence can detect Parkinson’s disease by analyzing volatile organic compounds (VOCs) in ear canal secretions with over 94% accuracy, potentially revolutionizing how we screen for this devastating neurological condition.
The research builds upon a remarkable observation from 2016, when Joy Milne, a Scottish woman, said she could detect Parkinson’s disease by smell years before her husband was diagnosed. Though met with skepticism at the time, her claims spurred scientists to investigate whether human scent, or more specifically, the chemical compounds behind it, could reveal hidden diseases.
Current Parkinson’s diagnoses typically rely on a neurologist’s evaluation of physical symptoms, which means the disease is often identified only after significant neurological damage has occurred. The study’s authors note that “early diagnosis and intervention are crucial for PD treatment,” but existing methods frequently miss that early window.
How Scientists Transformed Earwax Into a Diagnostic Sample
In the study, researchers from Zhejiang University collected earwax samples from 209 participants: 108 individuals diagnosed with Parkinson’s and 101 without. They analyzed the samples using two types of chemical detection methods: gas chromatography: mass spectrometry (GC-MS) and gas chromatography–surface acoustic wave (GC-SAW) sensors.
The GC-MS method identified four specific VOCs that were significantly different in the ear secretions of those with Parkinson’s:
- Ethylbenzene
- 4-Ethyltoluene
- Pentanal
- 2-Pentadecyl-1,3-dioxolane
These compounds appear to reflect differences in metabolic or environmental factors associated with the disease. Each was statistically more prevalent (present at higher concentrations) in the Parkinson’s group than in the control group.
Earwax was chosen for a specific reason. Compared to skin secretions or saliva, ear canal secretions are less susceptible to contamination from environmental elements like lotions, perfumes, or airborne pollutants. The study notes that “ear canal secretions exist in a more stable environment, simplifying sample collection and significantly enhancing the accuracy of analysis.”
The breakthrough came when researchers paired this chemical data with a machine learning system called a convolutional neural network (CNN), which excels at identifying patterns in complex data. The CNN was trained to analyze the VOC profiles of earwax samples and classify them as either Parkinson’s-positive or not.
Bringing Artificial Intelligence into Medical Diagnosis
Rather than simply measuring chemical concentrations, the AI system converts chromatographic data into structured visual representations. The model was trained and validated on known samples, and then tested for its ability to classify new ones.
When evaluated using the GC-SAW data, the CNN model achieved an accuracy of 94.4%, with strong sensitivity and specificity, meaning it was highly effective at identifying both true positive and true negative cases.
This is particularly notable given that conventional Parkinson’s diagnoses often require extended periods of symptom observation and costly imaging procedures. The earwax-based method, in contrast, may offer a quicker and more accessible screening tool, pending further validation.

Why Timing Matters in Parkinson’s Detection
Parkinson’s disease is a progressive neurological disorder that affects millions of people globally. The authors of the study estimate that by 2030, approximately 9 million individuals will be diagnosed worldwide. The condition gradually damages brain cells involved in movement and coordination, leading to tremors, stiffness, and cognitive changes.
Existing treatments can alleviate symptoms and may slow disease progression, but their effectiveness depends heavily on early initiation. Because many individuals are diagnosed only after substantial neurological decline, new tools that enable earlier identification could significantly improve outcomes.
A non-invasive, cost-effective diagnostic approach like this one could be particularly useful in primary care settings and underserved regions, where specialist access is limited.
When Will The Earwax Test For Parkinson’s Be Available?
Despite the promising results, several challenges must be addressed before this method can be used in routine clinical care.
First, the study sample was drawn from a single hospital in China. Larger studies involving diverse populations across different geographic regions and demographic groups will be necessary to confirm the generalizability of the findings.
Second, the current model functions only as a binary classifier: it identifies whether someone likely has Parkinson’s disease or not. In clinical practice, doctors must often distinguish between Parkinson’s and other movement disorders that can present with similar symptoms, such as essential tremor or atypical parkinsonism.
The origin of the chemical differences themselves also remains to be determined. It is unclear whether the identified VOCs are produced directly by the disease process, are byproducts of medication, or reflect other lifestyle-related factors. The researchers acknowledge that additional studies will be needed to clarify these mechanisms.
Finally, while the model achieved high accuracy using retrospective data, it has not yet been tested in prospective clinical trials. Its performance in real-world diagnostic settings remains to be seen.
Nevertheless, the approach aligns with a growing area of research in which artificial intelligence is used to analyze biologically informative molecules in breath, sweat, saliva, or other bodily secretions. Such work could expand early detection not only for Parkinson’s but also for other chronic illnesses.
And while a commercial earwax test for Parkinson’s may still be years away, the evidence suggests that it is now a scientifically credible possibility.
Paper Summary
Methodology
The study involved 209 participants, including 108 individuals diagnosed with Parkinson’s disease and 101 without the condition. Ear canal secretion samples were collected from each participant and analyzed using two types of gas chromatography: GC-MS (to identify chemical compounds) and GC-SAW (for rapid signal detection). The researchers trained two types of AI models: a support vector machine using GC-MS data, and a convolutional neural network (CNN) using GC-SAW data.
Results
Four volatile organic compounds—ethylbenzene, 4-ethyltoluene, pentanal, and 2-pentadecyl-1,3-dioxolane—were found in significantly different concentrations in the Parkinson’s group. The CNN model trained on GC-SAW data achieved 94.4% accuracy, with an area under the ROC curve of 0.98, indicating strong sensitivity and specificity. This performance suggests that VOCs in earwax may serve as reliable diagnostic indicators.
Limitations
The study was limited to a single site and had a relatively small sample size. Age and demographic imbalances between the two groups may have influenced the results. The AI model does not currently distinguish between Parkinson’s and other similar neurological disorders. Furthermore, the biological pathways leading to the observed chemical differences were not examined in depth.
Funding and Disclosures
This research was supported by the National Natural Science Foundation of China, the Zhejiang Province “Pioneer” and “Leading Goose” R\&D programs, and the Fundamental Research Funds for the Central Universities. The authors reported no conflicts of interest.
Publication Information
Chen, X., Li, Y., Pan, C., Weng, S., Xie, X., Zhou, B., Dong, H., & Zhu, D. (2025). “An Artificial Intelligence Olfactory-Based Diagnostic Model for Parkinson’s Disease Using Volatile Organic Compounds from Ear Canal Secretions,” published in Analytical Chemistry. Received February 12, 2025; revised April 29, 2025; accepted May 19, 2025. DOI: https://doi.org/10.1021/acs.analchem.5c00908







