
(© natali_mis - stock.adobe.com)
WASHINGTON — A newly developed bionic pancreas could eliminate the necessity for painful injections in diabetes patients. This revolutionary device employs a unique algorithm that controls implanted insulin pumps, which can be personalized according to each patient’s specific needs. Computer simulations indicate that the system’s insulin delivery is swift and closely replicates the body’s natural function.
“Not only is intraperitoneal infusion of insulin much more physiological because you are reproducing the natural physiology, but it simplifies the control problem because you don’t have delays,” explains study author Claudio Cobelli in a media release. “So, this means you can have a very simple, robust controller to handle the everyday situations.”
This artificial organ could greatly transform diabetes treatment. Presently, Type 1 diabetes impacts 46.3 million people globally, with a three-percent annual increase in the number of affected individuals. Managing this condition requires precise insulin calculations, with many patients needing multiple doses per day to control their blood sugar levels and guard against related diseases.
Standard insulin delivery methods involve multiple daily injections with small needles, an approach that can be inconvenient and painful, thereby reducing the quality of life. Normally, the pancreas naturally produces insulin which then travels to the liver to aid in glucose processing. However, individuals with Type 1 diabetes do not produce sufficient insulin, making dosage supplementation necessary for all patients.
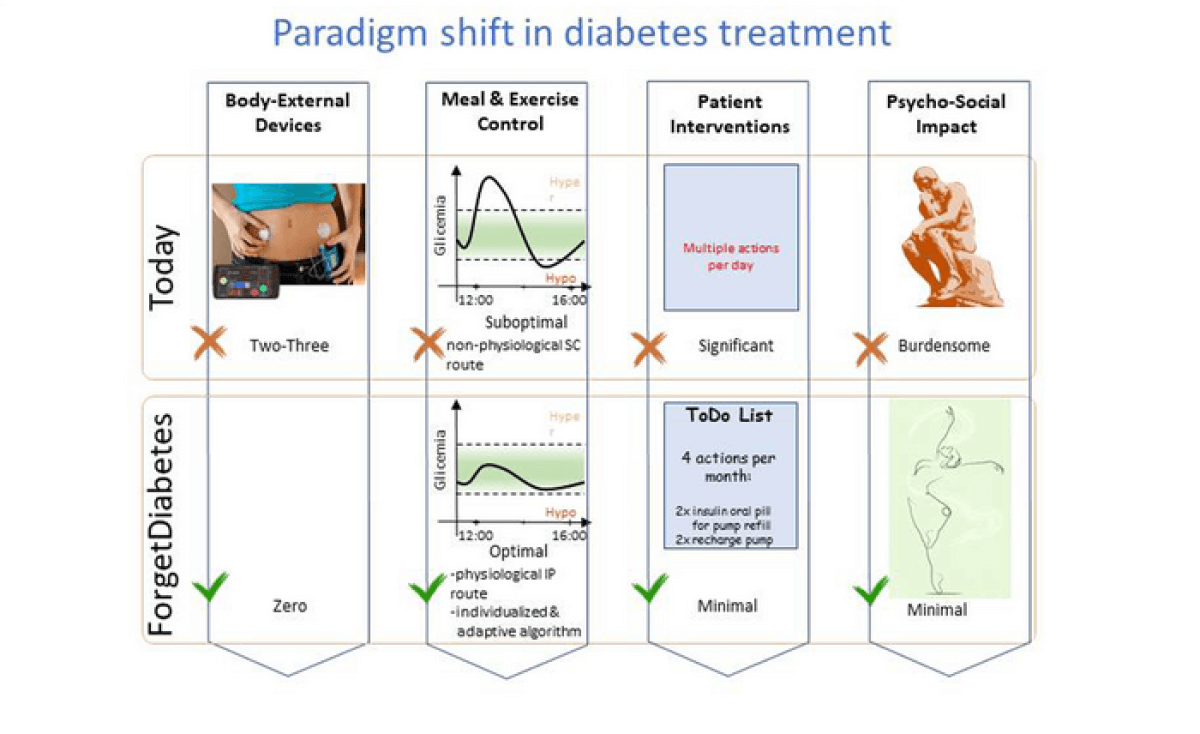
Currently, automated insulin delivery systems necessitate that patients manually input their carbohydrate consumption, notifying the system of their meals before they eat. Furthermore, these systems are slow to sense and deliver insulin, increasing the chance of inaccuracies due to delays and potential errors in manual meal calculations. This leads to a high incidence of hyperinsulinemia—a condition that damages large blood vessels.
In response to these challenges, an international team developed a model that accounts for individual patient variations and validated a pump control algorithm that eliminates the need for meal announcements.
“This is a big plus. It helps with tuning the devices and allows personalization,” Cobelli says. “Different people have different needs, so you need to personalize the algorithms.”
By merging data from prior research with current experimental results, the researchers validated the pump control algorithm, adjusting for mealtime variance at breakfast, lunch, and dinner. Their work, published in APL Bioengineering, is part of a European project named “FORGET DIABETES.” This initiative aims to expedite the development of automated insulin delivery technologies for clinical trials.
Today, diabetes is one of the top 10 leading causes of death worldwide.
You might also be interested in:
- Losing 15 percent of your bodyweight may be the best treatment for diabetes
- Artificial pancreas successfully helps Type 2 diabetes patients manage blood sugar levels
- Replacement pancreas created by stem cells could help patients with Type 1 diabetes
South West News Service writer Mark Waghorn contributed to this report.







