(© sdecoret - stock.adobe.com)
CORK, Ireland — Imagine a future where a computer can look inside your digestive system and tell your doctor exactly what’s going on, even before symptoms appear. This isn’t science fiction — it’s the cutting edge of medical technology, and it’s transforming how we understand and treat inflammatory bowel diseases (IBD) like Crohn’s disease and ulcerative colitis.
A forward-thinking review published in the journal eGastroenterology reveals how artificial intelligence (AI) is reshaping the landscape of IBD care. Led by researchers Yasuharu Maeda and colleagues, this study explores the exciting potential of AI to enhance the accuracy of diagnoses, predict disease outcomes, and personalize treatment plans for millions of IBD patients worldwide.
IBD affects an estimated 6.8 million people globally, causing chronic inflammation in the digestive tract that can lead to severe complications if left untreated. Traditionally, diagnosing and monitoring IBD has relied heavily on invasive procedures like colonoscopies and subjective interpretations by doctors. But what if a computer could do this job more accurately and consistently?
Enter AI-assisted endoscopy. This cutting-edge technology uses complex algorithms to analyze images and videos from inside the intestines, identifying signs of inflammation and disease activity that might be missed by the human eye. The review highlights several studies where AI systems have shown remarkable accuracy in assessing disease severity and predicting outcomes.
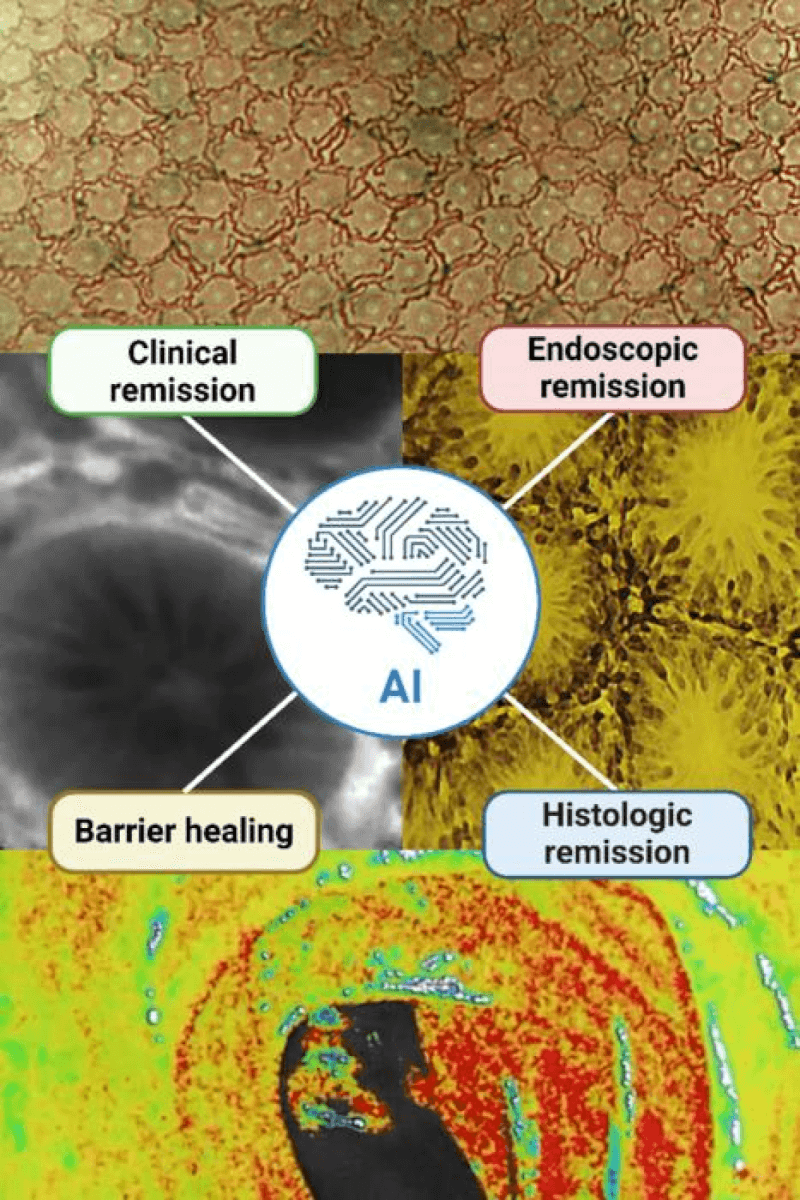
One standout example is a study by Takenaka and colleagues, where an AI model analyzed colonoscopy videos from 590 patients with ulcerative colitis. The AI achieved an astounding 98% sensitivity and 95% specificity in identifying histological remission — a key indicator of disease control. This level of accuracy surpasses what most human experts can achieve consistently.
AI’s potential goes beyond just looking at pictures. The review also explores how AI can integrate various data sources, including genetic information, blood tests, and even gut microbiome profiles, to create a more comprehensive understanding of each patient’s condition. This holistic approach could lead to more personalized treatment strategies, potentially improving outcomes and quality of life for IBD patients.
One of the most exciting applications of AI in IBD care is its ability to predict future disease flares. Imagine if your doctor could tell you months in advance that you’re at risk of a disease flare-up, allowing for preventative measures to be taken. Several studies highlighted in the review demonstrate AI’s prowess in this area, with some models accurately predicting the need for biological therapy or the risk of relapse within a year.
The implications of this technology are far-reaching. For patients, it could mean fewer invasive procedures, more targeted treatments, and better long-term health outcomes. For healthcare systems, AI could lead to more efficient resource allocation and potentially reduce the economic burden of IBD, which is estimated to cost billions of dollars annually in healthcare expenses and lost productivity.
However, the road to widespread adoption of AI in IBD care is not without challenges. The review acknowledges that most of these AI systems are still in the research phase and need further validation in real-world clinical settings. There are also important ethical considerations, such as ensuring patient privacy and addressing potential biases in AI algorithms.
Despite these hurdles, the overall tone of the review is one of cautious optimism. The authors envision a future where AI becomes an indispensable tool in the IBD clinician’s arsenal, working alongside human expertise to provide the best possible care for patients. While the journey ahead may have its challenges, the destination – a world where IBD is more manageable and less disruptive to patients’ lives – is well worth the effort.
Paper Summary
Methodology
This review article examined a wide range of studies that applied artificial intelligence to various aspects of inflammatory bowel disease care. The researchers systematically analyzed published literature on AI applications in endoscopy, histology, and predictive modeling for IBD. They focused on studies that used machine learning algorithms to analyze images from colonoscopies, tissue samples, and other diagnostic tests. The review process involved evaluating the methods, results, and potential clinical implications of each included study.
Key Results
The review found that AI systems consistently demonstrated high accuracy in assessing IBD disease activity, often matching or exceeding the performance of human experts. For example, multiple studies showed AI models achieving over 90% accuracy in identifying endoscopic remission in ulcerative colitis.
AI was also effective in predicting disease outcomes, with some models accurately forecasting the need for escalated therapy or the risk of relapse. Additionally, AI showed promise in integrating multiple data types to provide more comprehensive disease assessments.
Study Limitations
The authors note several limitations in the current state of AI research for IBD. Most studies were conducted in controlled research settings and may not fully reflect real-world clinical scenarios. There is a need for larger, multicenter studies to validate these AI models across diverse patient populations.
The review also highlights the challenge of standardizing AI algorithms across different healthcare systems and endoscopy equipment. Furthermore, many of these AI technologies are still in developmental stages and require regulatory approval before widespread clinical use.
Discussion & Takeaways
The review emphasizes the transformative potential of AI in IBD care, particularly in improving diagnostic accuracy, predicting outcomes, and personalizing treatment plans. The authors suggest that AI could lead to more objective and standardized assessments of disease activity, potentially reducing variability in clinical decision-making.
They also highlight the potential for AI to integrate various data sources, creating a more holistic view of each patient’s condition. However, the discussion also stresses the importance of carefully validating these AI tools and addressing ethical concerns before full clinical implementation. The authors conclude that while AI shows great promise, it should be seen as a tool to augment, not replace, clinical expertise in IBD management.
Funding & Disclosures
The review article does not mention any specific funding sources for this particular study. The authors declare no conflicts of interest related to this work. However, it’s important to note that many of the individual studies reviewed may have had their own funding sources and potential conflicts of interest, which were not detailed in this overarching review.







