A standard body fat test may not reveal the true scope of your overall health. (© Dmytro Panchenko - stock.adobe.com)
In A Nutshell
- A 15-year study of 4,252 U.S. adults found body fat percentage is a significantly better predictor of early death than Body Mass Index (BMI).
- BMI showed no statistically significant link to all-cause mortality after adjusting for age, race, and income.
- People with high body fat had a 78% greater risk of death and were 3.6 times more likely to die from heart disease.
- BMI and body fat percentage only agreed 60% of the time when assessing who was “healthy,” raising concerns about misclassification.
GAINESVILLE, Fla. — That dreaded moment at the doctor’s office when you step on the scale? The calculation that follows may not be as telling as many assume. A new study tracking 4,252 U.S. adults over a 15-year period found that body fat percentage was a significantly better predictor of mortality than Body Mass Index (BMI), the widely used standard.
While BMI, an indirect measure of body composition based on height and weight, is still common in clinical settings, the study found that it was not significantly associated with death risk after adjusting for key demographic factors.

BMI vs. Body Fat: A Side-By-Side Comparison
Researchers from the University of Florida analyzed data from the National Health and Nutrition Examination Survey (NHANES) collected between 1999 and 2004. They linked this data to the National Death Index through December 31, 2019, but crucially, they capped individual follow-up at 15 years to ensure consistency in mortality tracking.
Participants were between 20 and 49 years old, and though the study analyzed 4,252 unweighted individuals, its design represents a broader population of approximately 131 million Americans. Instead of relying on BMI alone the researchers also used bioelectrical impedance analysis (BIA), a technology that estimates body fat percentage by measuring how electrical currents move through the body.
The results, published in the Annals of Family Medicine, were stark. Individuals classified as having unhealthy body fat levels had a 78% higher risk of dying during the study period. By contrast, BMI showed no statistically significant association with all-cause mortality in adjusted models. BMI did initially show a significant link with heart disease deaths in unadjusted models, but that association disappeared after accounting for age, race, and poverty status.
Interestingly, BMI and body fat percentage only aligned in classifying participants as “healthy” or “unhealthy” about 60% of the time. In four out of ten cases, the two measures gave conflicting assessments of health risk.
Why Body Fat Percentage May Matter More
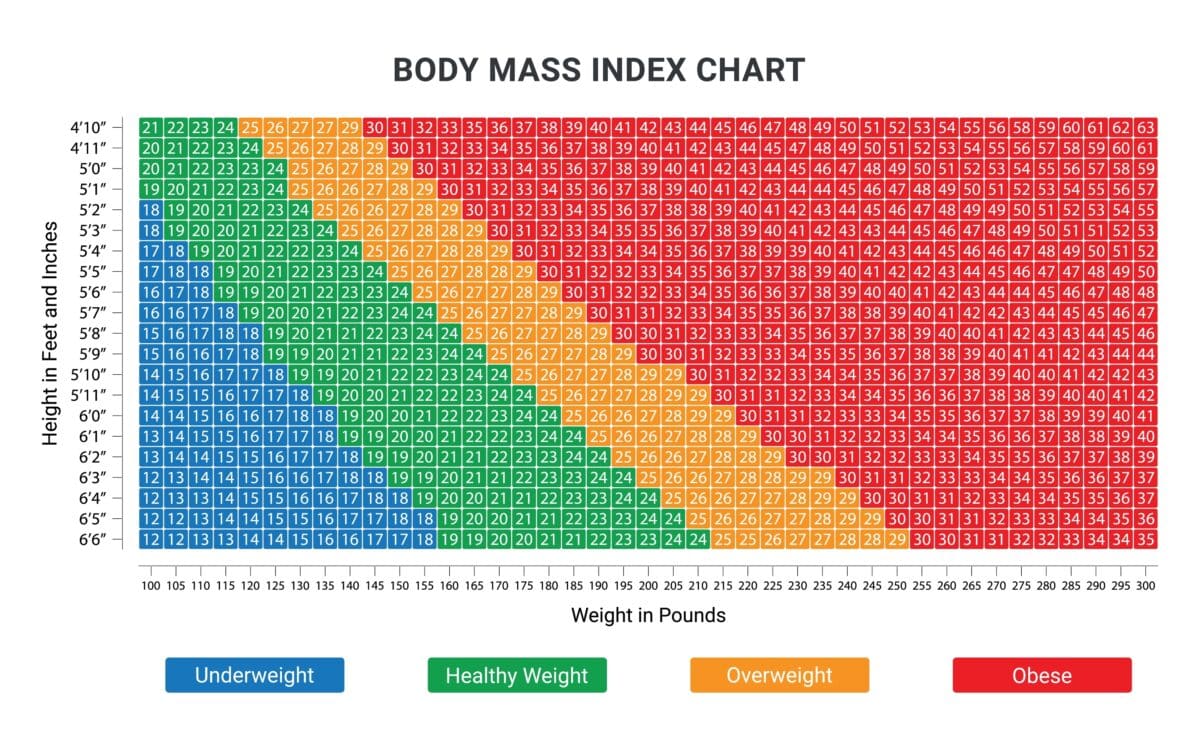
The mismatch makes intuitive sense. BMI can misclassify muscular individuals as obese and fail to identify those who carry dangerous fat deposits despite having a “normal” weight. For example, someone with a lean, muscular build may have a high BMI but low health risk, while someone with little muscle mass and high visceral fat may have a normal BMI but elevated risk.
The study notes that individuals with normal BMI but high body fat percentage “may be unaware of their significantly increased risk of metabolic syndrome, Type 2 diabetes, and cardiovascular disease,” citing previous literature (not directly quoting any one author).
Modern BIA devices offer rapid and reproducible readings. The study used technology that was already 25 years old at the time of analysis, yet still found it more predictive of health outcomes than BMI. The authors point out that today’s BIA tools are “inexpensive, reliable, valid, and can be easily integrated into a clinic setting,” though the paper does not explicitly state they are “far less costly” than older tools.
Heart disease outcomes showed the clearest difference. Individuals with unhealthy body fat had 3.6 times higher risk of dying from heart disease, while BMI’s association with heart disease mortality vanished in adjusted analyses.
BMI’s Staying Power Despite New Evidence
Despite the growing body of research highlighting BMI’s limitations, the metric remains widely used by major health organizations including the CDC, NIH, WHO, ADA, and AHA. That’s largely because it’s quick and easy: height and weight are already collected at nearly every medical visit, while body fat measurement has traditionally required specialized equipment and additional time.
However, the authors caution that convenience may come at a cost. BMI can misclassify patients, sometimes triggering unnecessary interventions, and other times overlooking serious health risks.
What This Means for Your Health
The authors acknowledge several limitations. First, unlike BMI, body fat percentage thresholds are not yet standardized across institutions. Second, the study focused only on adults aged 20–49, meaning the findings may not apply to older populations. Third, the analysis focused exclusively on mortality rather than other health conditions like diabetes or cancer. Additionally, factors like smoking and physical activity were not included in the models. The authors explain this was deliberate: the goal was to assess body composition metrics as they are currently used in clinical settings, where such risk categories typically don’t adjust for smoking or exercise.
Still, the results reinforce what other research has been pointing to for years: body fat percentage offers a clearer view of long-term health risks than BMI alone. As lead author Frank Orlando and his co-authors suggest, it may be time to rethink how we assess body composition in both doctor’s offices and public health policy.
For many Americans, this could mean a shift in how health is judged; not just by what the scale says, but by what’s going on beneath the surface.
Disclaimer: This article is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your healthcare provider before making any changes to your health practices.
Paper Summary
Methodology
Researchers analyzed data from the National Health and Nutrition Examination Survey (NHANES) collected between 1999-2004, linking it to the National Death Index through December 2019. The study included 4,252 adults aged 20-49 years who were followed for 15-year mortality outcomes. Body mass index was calculated using standard height and weight measurements, while body fat percentage was measured using bioelectrical impedance analysis. Statistical analysis compared how well each measurement predicted death risk, controlling for factors like age, race, and poverty status.
Results
Body fat percentage showed strong statistical association with 15-year all-cause mortality (adjusted hazard ratio 1.78, P<0.001) and heart disease mortality (adjusted hazard ratio 3.62, P=0.003). BMI showed no statistically significant relationship with all-cause mortality and lost its association with heart disease mortality after adjusting for other factors. The two measurements only agreed 60% of the time when classifying people as healthy or unhealthy.
Limitations
The study was limited to adults aged 20-49, so findings may not apply to older populations. Body fat percentage thresholds used aren’t standardized like BMI categories. The research focused only on mortality outcomes rather than other health conditions. The study didn’t control for potentially important factors like smoking status or physical activity levels.
Funding and Disclosures
The authors reported no conflicts of interest. No specific funding information was provided.
Publication Information
Mainous III, A.G., Yin, L., Wu, V., Sharma, P., Jenkins, B.M., Saguil, A.A., Nelson, D.S., & Orlando, F.A. (2025). “Body Mass Index vs Body Fat Percentage as a Predictor of Mortality in Adults Aged 20-49 Years,” published in Annals of Family Medicine, 23(4), 337-343.








I am not sure about the accuracy of BIA. I have a scale that measures body fat percentage and lean mass and there is quite a variation day to day. Body fat percentage varies by around two percentage points which is about a 13% variation. It seems like a lot but maybe I am making too much of it. I guess the trick is to average the readings over a week’s time but that doesn’t help if it is a single reading in the doctor’s office. It still gives you an idea of a target range so in that respect it is helpful.
It’s always been pretty obvious to anyone who knows anything about fitness that BMI was a really stupid measure, assigning a better health rating for not good reason to someone who has a narrow frame (like a marathoner rather than like a sprinter or shot-putter), and for having a frail physique that lacks muscular strength.