(© Katsiaryna - stock.adobe.com)
CAMBRIDGE, United Kingdom — A drug sitting on pharmacy shelves could also help fight back against devastating brain diseases like Alzheimer’s. Researchers at the University of Cambridge have found that a medication typically used to treat glaucoma might offer a new weapon in the fight against neurodegenerative disorders.
Researchers have uncovered an unexpected ally in methazolamide, a drug primarily prescribed for eye conditions. In an innovative study published in Nature Chemical Biology, the team demonstrated how this medication could potentially clear harmful protein build-up associated with various forms of dementia.
The research focused on tau, a protein that, when it accumulates abnormally in the brain, can lead to devastating neurological conditions. These include Alzheimer’s, Pick’s disease, and progressive supranuclear palsy – conditions that currently have limited treatment options.
What makes this research particularly exciting is its creative approach to drug discovery. Instead of traditional laboratory cell cultures, the Cambridge team turned to an unlikely research subject: zebrafish. These small, transparent fish share surprising genetic similarities with humans, allowing scientists to model human diseases with remarkable precision.
“Zebrafish provide a much more effective and realistic way of screening drug compounds than using cell cultures,” explains Dr. Ana Lopez Ramirez, one of the study’s lead researchers, in a media release. “They also enable us to do so at scale, something that [is] not feasible or ethical in larger animals such as mice.”
The team screened an impressive 1,437 clinically-approved drug compounds, focusing on a class of medications called carbonic anhydrase inhibitors. Their breakthrough came when they discovered these drugs could help cells clear out tau protein build-up by essentially “taking out the trash” – triggering lysosomes (the cell’s waste disposal system) to move to the cell surface and expel the harmful protein accumulations.
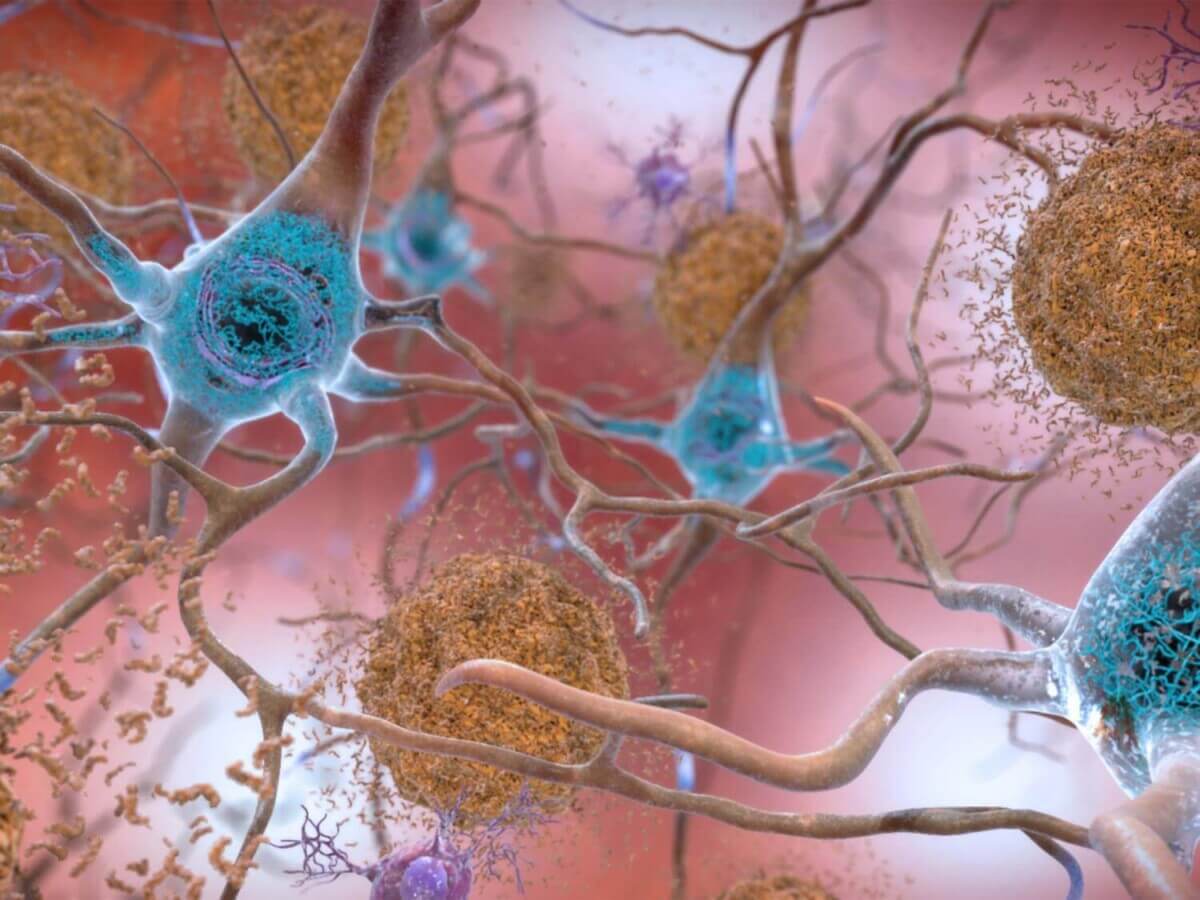
When tested on mice genetically engineered to carry a human tau mutation, the results were promising. Mice treated with methazolamide, which also goes by the brand name Neptazane, showed improved memory and cognitive performance, with significantly fewer tau protein aggregates in their brains compared to untreated mice.
“Methazolamide shows promise as a much-needed drug to help prevent the build-up of dangerous tau proteins in the brain,” says Professor David Rubinsztein, a lead researcher on the study.
Crucially, because methazolamide is already an approved medication, the path to potential clinical trials could be much faster than developing an entirely new drug. The research team isn’t stopping here. They plan to investigate methazolamide’s potential in treating other neurodegenerative diseases, including Huntington’s and Parkinson’s.
While it’s too early to celebrate a definitive cure, this research offers a glimmer of hope in the challenging landscape of brain diseases. By reimagining existing medications and using innovative research methods, scientists are opening new doors in the fight against devastating neurological conditions.
Paper Summary
Methodology
This study explored whether carbonic anhydrase (CA) inhibitors could reduce tau protein toxicity, a core feature in neurodegenerative diseases like Alzheimer’s. Researchers used a multi-phase approach, first screening over 1,400 drugs using a zebrafish model genetically engineered to express human tau protein. Zebrafish with this tau protein show neurodegenerative symptoms, making them ideal for testing drug effects.
Promising drugs were further validated in mouse models to ensure their effects on tau reduction were consistent and meaningful. The final phase used a specific CA inhibitor, methazolamide, in mice to confirm its effects and track tau protein reduction over time.
Key Results
The study revealed that CA inhibitors, especially methazolamide, significantly reduced tau protein levels and associated neurodegenerative symptoms in both zebrafish and mouse models. The zebrafish tests showed fewer tau aggregations and improved neuronal health with drug treatment.
In mice, methazolamide reduced tau-related toxicity, leading to better memory and cognitive performance. These findings suggest that CA inhibitors may help slow neurodegeneration, making them promising candidates for treating diseases characterized by tau protein buildup.
Study Limitations
The study relied on animal models, which, while useful, do not completely replicate human disease conditions. Zebrafish and mice, though showing tau toxicity, cannot capture the complexity of human tauopathies. Additionally, long-term effects and potential side effects of CA inhibitors need further investigation to understand their full implications in humans. Since different stages of neurodegeneration might respond differently to treatments, future studies should assess the drugs across various disease stages.
Discussion & Takeaways
The study underscores the potential of repurposing CA inhibitors as treatments for tau-related neurodegeneration. By accelerating tau clearance, these drugs might reduce the spread of toxic tau across neurons. This innovative approach could open new pathways for slowing down or even halting the progression of diseases like Alzheimer’s and other tauopathies.
However, translating these findings to human patients will require careful consideration of dosage, long-term effects, and specific disease mechanisms. The success of CA inhibitors in animal models points to a valuable direction in the search for effective neuroprotective drugs.
Funding & Disclosures
The research received funding from the UK Dementia Research Institute, Wellcome Trust, Alzheimer’s Research UK, and other institutions committed to studying neurodegeneration. The lead researcher, Dr. David C. Rubinsztein, disclosed consulting roles with several biotech companies, though no direct conflict of interest was reported in relation to this study.







