
Obesity And The Brain (© freshidea - stock.adobe.com)
CHICAGO — Decades before the first signs of memory loss appear, a hidden type of body fat might be signaling the early stages of Alzheimer’s disease.
Scientists have discovered a startling connection between visceral fat — the deep, hard-to-see fat that wraps around our internal organs — and the abnormal brain proteins associated with Alzheimer’s, potentially up to 20 years before symptoms emerge.
The study, led by researchers at Washington University School of Medicine and presented at the Radiological Society of North America’s annual meeting, examined 80 cognitively healthy adults with an average age of 49. Notably, nearly 58% of participants were classified as obese, with an average body mass index (BMI) of 32.31. For reference, a BMI between 18.5 and 24.9 is considered normal.
Using advanced imaging techniques, the research team mapped participants’ body composition and brain chemistry in unprecedented detail. They used brain PET scans to track the buildup of amyloid and tau proteins — the hallmark indicators of Alzheimer’s disease — and MRI scans to measure different types of body fat. The most striking finding is that visceral fat appears to be the critical culprit.
“Higher visceral fat was associated with higher PET levels of the two hallmark pathologic proteins of Alzheimer’s disease—amyloid and tau,” says lead study author Dr. Mahsa Dolatshahi in a media release.
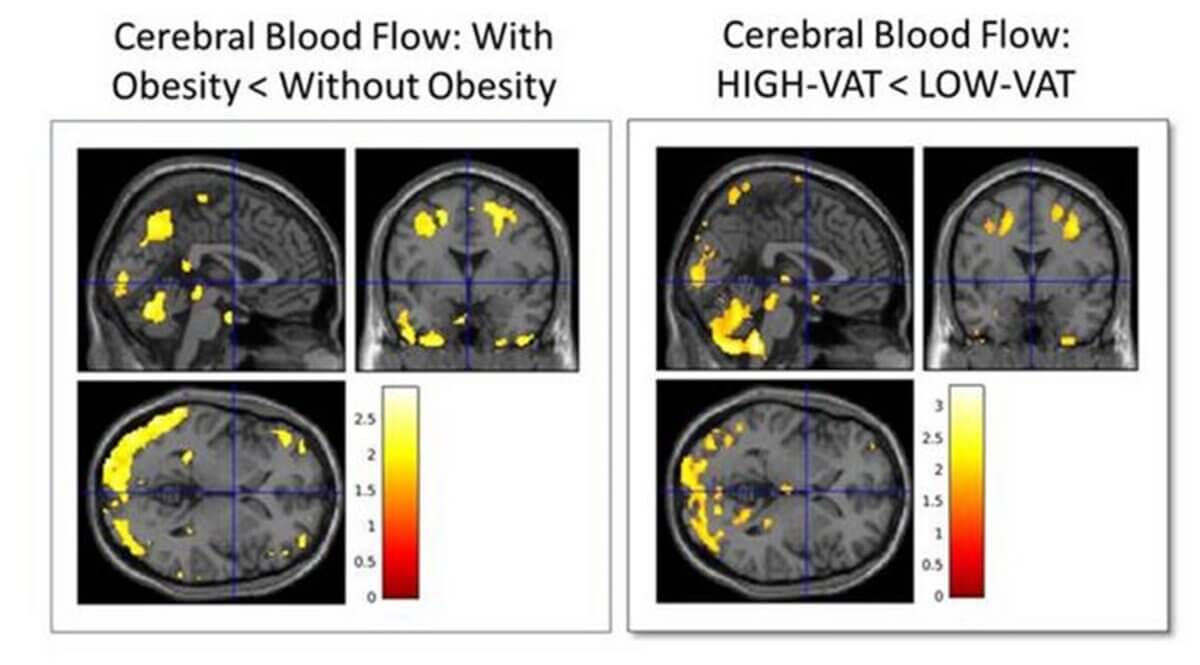
Radiological Society of North America (RSNA) and Mahsa Dolatshahi, M.D., M.P.H.)
Critically, visceral fat accounted for 77% of the effect of high BMI on protein accumulation. Other fat types showed no similar correlation. The study also revealed that higher insulin resistance and lower levels of “good” cholesterol (HDL) were linked to increased brain protein buildup.
For context, an estimated 6.9 million Americans currently live with Alzheimer’s, a number projected to double to 13 million by 2050 without significant medical breakthroughs.
“A key implication of our work is that managing Alzheimer’s risk in obesity will need to involve targeting the related metabolic and lipid issues that often arise with higher body fat,” explains senior study author Dr. Cyrus A. Raji.
The research offers a glimmer of hope: lifestyle modifications targeting visceral fat in midlife could potentially delay or prevent Alzheimer’s onset.
“Knowing that visceral obesity negatively affects the brain opens up the possibility that treatment with lifestyle modifications or appropriate weight-loss drugs could improve cerebral blood flow and potentially lower the burden of and reduce the risk for Alzheimer’s disease,” Dr. Raji notes.
With nearly three out of four Americans classified as overweight or obese, this study provides a powerful reminder that our body composition isn’t just about appearance — it could be a critical indicator of long-term brain health.







