(Image by crystal light on Shutterstock)
In a nutshell
- Steroid injections were associated with faster arthritis progression compared to no treatment or hyaluronic acid injections
- Hyaluronic acid injections showed signs of slowing disease progression while still providing pain relief
- Both treatments reduced pain, but only steroid shots were linked to concerning structural changes on MRI scans
SAN FRANCISCO — Getting a cortisone shot for knee arthritis might provide quick pain relief, but new research reveals a troubling association: those steroid injections may be linked to faster joint damage over time. A surprising study found that patients who received corticosteroid injections showed more signs of arthritis progression compared to those who got no treatment at all, or even a different type of injection.
The findings raise important questions about a common medical practice. More than 10% of knee arthritis patients receive these steroid shots, yet the study suggests they may be trading short-term comfort for potential long-term harm. By contrast, patients who received hyaluronic acid injections — a gel-like lubricant for joints — not only avoided signs of worsening arthritis, but actually showed reduced disease progression on MRI scans.
How Researchers Conducted the Investigation
The study, published in Radiology, analyzed data from 210 people participating in the Osteoarthritis Initiative, a large-scale project tracking Americans with knee problems from 2004 to 2015. The average participant was 64 years old, and around 60% were women—characteristics typical of the knee arthritis population.
What set this study apart was its use of detailed MRI scans to assess joint health. Researchers evaluated images from two years before the injection, at the time of injection, and again two years afterward using the Whole-Organ MRI Score (WORMS). This scoring system provides a comprehensive assessment of cartilage, bone marrow, meniscus, ligaments, and joint effusion.
Participants were grouped into three categories: 44 received corticosteroid injections, 26 received hyaluronic acid, and 140 were matched controls who had no injections. The control group was carefully selected using propensity-score matching to ensure they were comparable in age, sex, body mass index, arthritis severity, pain levels, and physical activity.

Clear Differences Emerged Between Treatments
Those who received steroid injections showed significantly more arthritis progression than both the control group and the hyaluronic acid group. The researchers found clear statistical evidence that steroid shots were linked to faster joint deterioration. The damage was especially evident in cartilage—the smooth tissue that cushions the knee joint.
By contrast, hyaluronic acid injections appeared to slow down arthritis progression. Patients in this group actually showed less joint damage after their injection compared to before they received it, suggesting these treatments may help protect the joint structure.
Both types of injections helped with pain relief. Steroid shots provided more dramatic pain reduction — cutting pain scores roughly in half — while hyaluronic acid injections offered more modest but still meaningful pain relief. However, only steroid shots came with the concerning side effect of potentially faster joint deterioration.
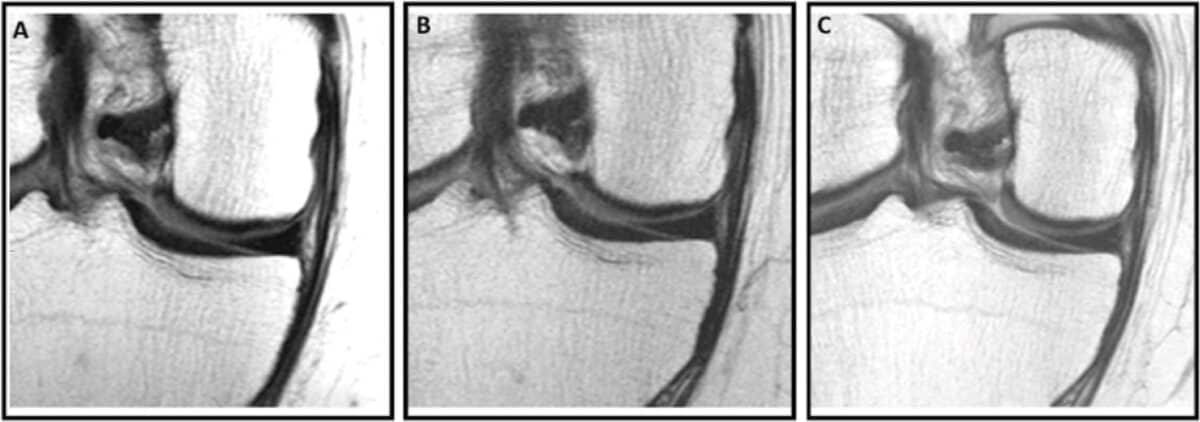
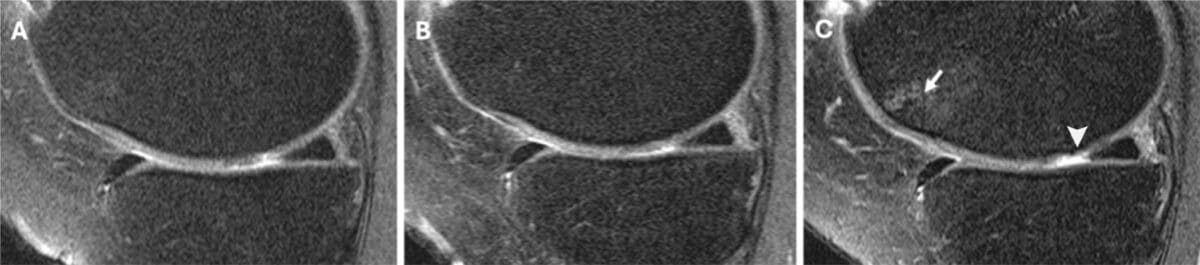
MRI images helped visualize the contrast. In a 58-year-old woman who received a steroid injection, follow-up scans showed new full-thickness cartilage lesions and bone marrow damage. In a 57-year-old man who received hyaluronic acid, the same cartilage remained intact and unchanged over four years.
What This Means for Your Healthcare Decisions
These findings don’t mean patients should avoid knee injections altogether. Managing arthritis pain is important for maintaining mobility and quality of life. But the results highlight the need for deeper conversations between patients and healthcare providers about treatment trade-offs.
Current guidelines from the American Academy of Orthopaedic Surgeons moderately recommend corticosteroids for short-term pain relief and advise against the routine use of hyaluronic acid. The new study doesn’t overturn those guidelines, but it suggests they may merit reevaluation if future research supports these results.
Importantly, this study cannot prove that steroid injections directly cause faster arthritis progression. It was observational in nature, meaning that unmeasured differences between patients could account for some of the outcomes. Still, the consistent patterns seen on MRI raise important questions that warrant further investigation in randomized controlled trials.
For the millions of Americans living with knee arthritis, this study offers both a note of caution and a reason for hope. Cortisone shots may still help with intense pain episodes, but patients should understand the potential risks to long-term joint health. Meanwhile, hyaluronic acid injections, often overlooked, may offer pain relief without the same structural downsides.
“This study could lead to more judicious use of corticosteroid injections, especially for patients with mild to moderate osteoarthritis who are not yet surgical candidates,” said lead author Dr. Upasana Upadhyay Bharadwaj, who was a research fellow in the Department of Radiology at University of California, San Francisco, at the time of the research, in a statement.
“Given their widespread use, these findings could influence clinical guidelines and patient care decisions, encouraging more cautious use and stronger consideration of alternatives like hyaluronic acid,” she added. “The public impact is significant, as osteoarthritis is a major global cause of disability, and millions receive such injections annually.”
Paper Summary
Methodology
Researchers conducted a secondary analysis of data from the Osteoarthritis Initiative, following 210 participants (mean age 64 years, 60% female) over multiple years. They used detailed 3-T MRI scans taken at three time points: two years before injection (T-2), at the time of injection (T0), and two years after injection (T+2). The study compared three groups—those who received corticosteroid injections (44 people), hyaluronic acid injections (26 people), and propensity-score matched controls who received no injections (140 people). Joint health was measured using the comprehensive Whole-Organ MRI Score (WORMS) system rather than simple X-rays. Only participants with a single injection during the study period were included.
Results
Corticosteroid injections were associated with greater WORMS progression compared to both controls (mean difference, 0.39; 95% CI: 0.05, 0.75; P = .02) and hyaluronic acid injections (0.42; 95% CI: 0.01, 0.84; P = .04) over the two-year follow-up period. Hyaluronic acid injections showed decreased progression compared to the pre-injection period (mean difference, −0.42; 95% CI: −1.34, −0.28; P = .003). Both injection types delivered pain relief, with corticosteroid injections reducing WOMAC pain scores by 5.20 points (P = .001) and hyaluronic acid by 2.15 points (P = .04). The differences were particularly notable in cartilage deterioration.
Limitations
As an observational study, it cannot establish direct causation between injections and arthritis progression. The researchers noted potential confounding factors and selection bias, as people who choose different treatments may differ in unmeasured ways. The study only included participants who reported receiving a single injection, which may limit generalizability to those receiving multiple treatments. Additionally, the study relied on participant reporting of injections, with potential gaps of 2 or more years between questions about injections when follow-up appointments were missed.
Funding and Disclosures
The study was supported by multiple National Institutes of Health grants (R01 AR064771, R01 AR078917, R01 AG070647). The data came from the Osteoarthritis Initiative, a public-private partnership funded by the National Institute of Arthritis and Musculoskeletal and Skin Diseases with additional private funding from pharmaceutical companies including Merck Research Laboratories, Novartis Pharmaceuticals, GlaxoSmithKline, and Pfizer. Most authors reported no relevant financial relationships, though some had consulting relationships with various companies.
Publication Information
The study was published in Radiology, Volume 315, Number 2, May 2025, by Bharadwaj et al. The research was a secondary analysis of data from the Osteoarthritis Initiative study conducted from February 2004 to January 2015, with the clinical trial identifier NCT00080171.








This article was sent to me by a friend, not a doctor, but someone with a medical background. I am impressed with the thoroughness and unbiased detail herein, and also the clarity of the material. I suffer from arthritis (undetermined type), and have had my right knee and right ankle replaced some fifteen years ago, with great success. I recently. began to experience pain in my left knee. My doctor said I was a candidate for replacement, but hesitated because of my age (84). He, gave me a cortisone injection and said to come back for further treatment. I was told not to worry about further damage, because I have no cartilage remaining. I related this to a friend and she sent your article to me. (The injection gave me relief for perhaps one day).