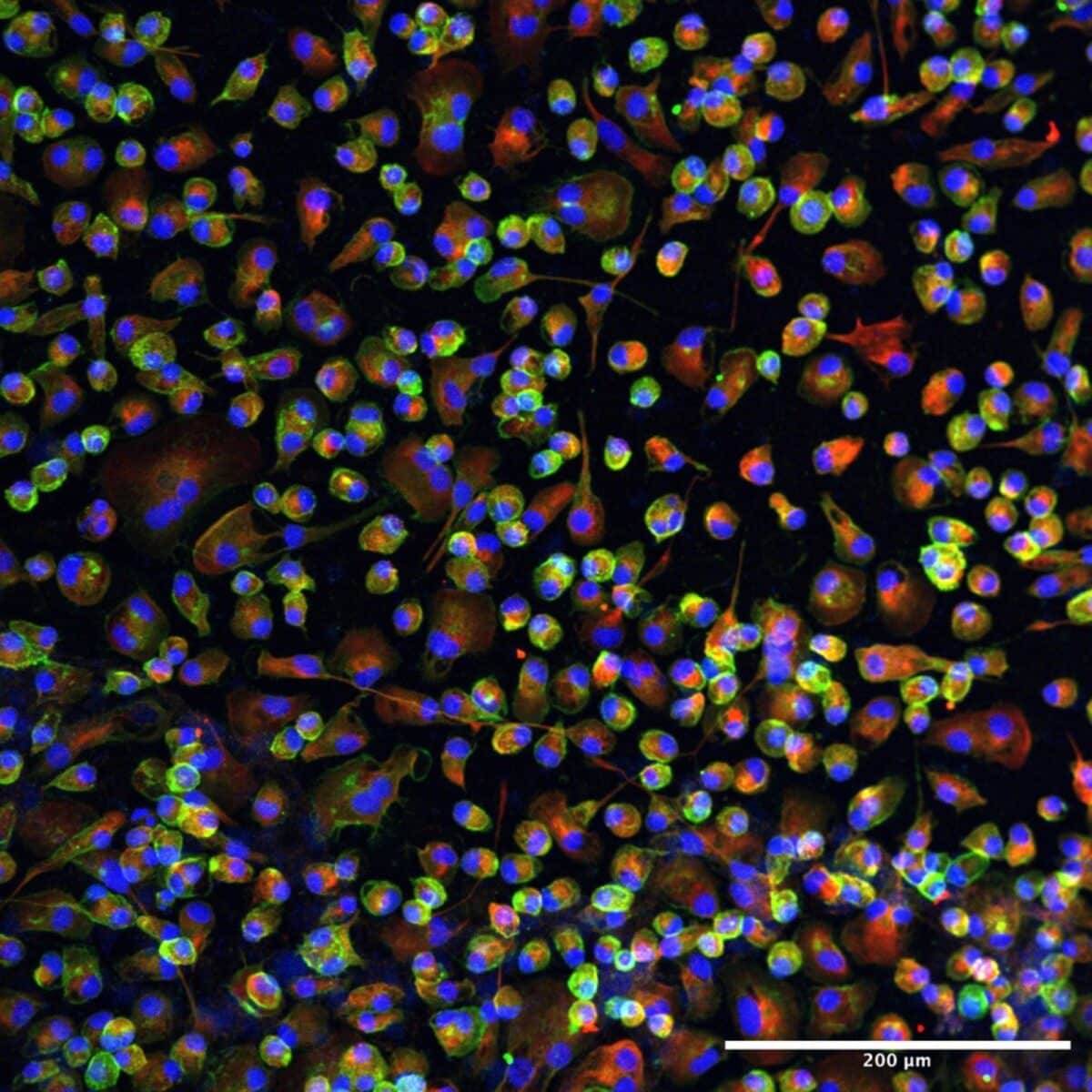
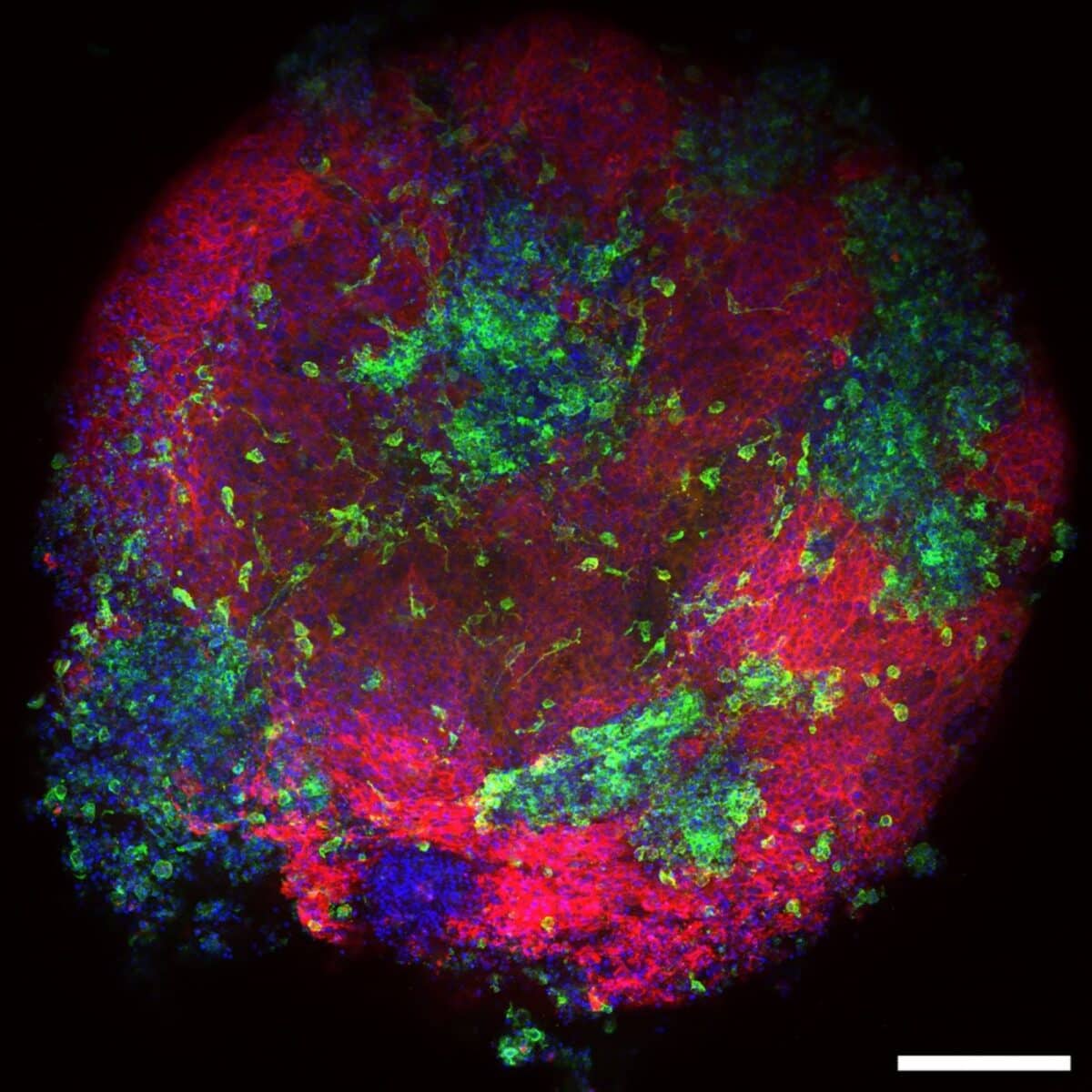
A human heart macrophage assembloid is shown using immunofluorescent microscopy imaging. The red color marks the heart muscle cells, the green color marks the macrophages and the blue color marks all cells. The scale bar in the bottom right corner of the image is 200 micrometers, or 0.2 mm, in length. Graphic courtesy of the Aguirre lab at Michigan State University.
These tiny hearts may help develop new AFib treatments without any human (or animal) patients
In a Nutshell
- Researchers added immune cells called macrophages to lab-grown mini-hearts, creating a more realistic model of human heart tissue that includes the immune system.
- When exposed to chronic inflammation, these mini-hearts developed irregular, rapid electrical activity characteristic of atrial fibrillation, the most common heart rhythm disorder.
- The immune cells wired directly into the heart’s electrical system and amplified the irregular beats, revealing how inflammation triggers arrhythmias.
- The platform successfully tested an anti-inflammatory drug and could help researchers develop new treatments without relying on animal models.
Scientists have built lab-grown miniature hearts that can develop irregular heartbeats after prolonged inflammatory exposure, giving researchers a promising and novel way to study the most common heart rhythm disorder and test treatments without using animals or human patients.
Published in Cell Stem Cell, the breakthrough involves adding immune cells called macrophages to mini-hearts grown from stem cells. When researchers exposed these lab-grown hearts to chronic inflammation, they developed the chaotic, rapid electrical activity seen in atrial fibrillation.
Atrial fibrillation affects millions of people worldwide and can lead to stroke and heart failure. Doctors know chronic inflammation triggers the condition, but studying exactly how has been difficult. Animal models don’t perfectly match human biology, and studying diseased human hearts raises ethical concerns.
Adding Immune Cells to Lab-Grown Hearts
The Michigan State University team started with mini-hearts they’d grown from stem cells. These already contained muscle cells and blood vessel cells, but they were missing macrophages—immune cells that move into developing hearts during embryonic life.
Researchers created macrophage precursors from the same stem cells and added them on days 8, 12, and 16 of development, timing it to mimic what happens in actual human embryos. Adding 20,000 to 30,000 cells at each stage produced mini-hearts where about 1 to 3 percent were macrophages, matching real embryonic hearts.
The immune cells didn’t just sit on the surface. They migrated deep into the tissue and stuck around for at least 60 days, just like macrophages do in real hearts. Genetic testing confirmed these lab-grown immune cells closely matched their natural counterparts in human embryos.
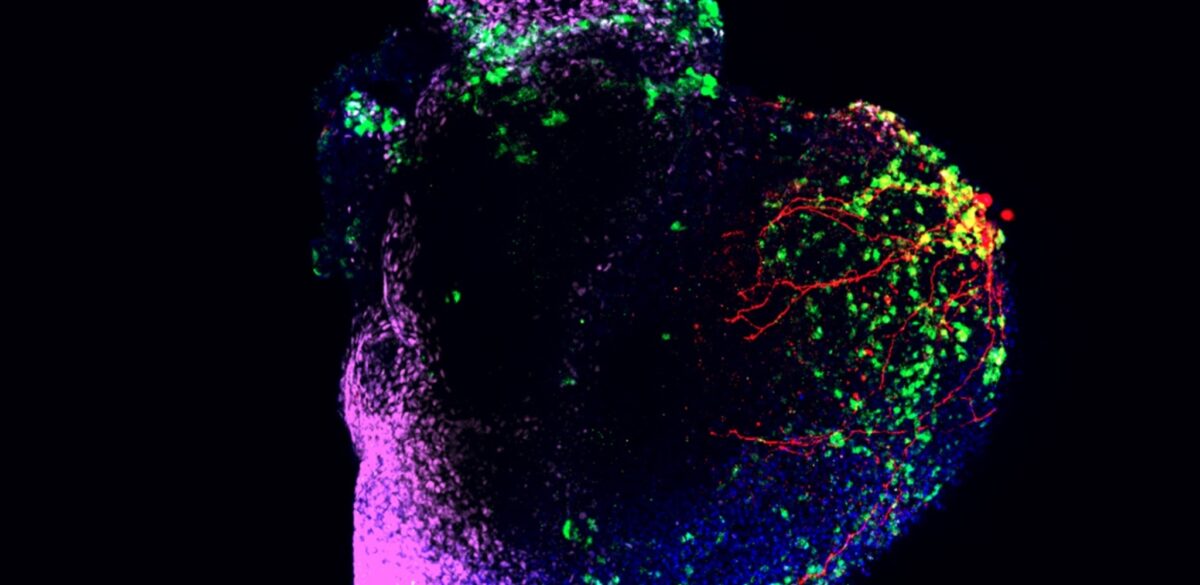
The red areas represent blood vessels or neural networks within the organoid. Image courtesy
of the Aguirre lab at Michigan State University.
Immune Cells Wire Into the Heart’s Electrical System
One surprising discovery: about 85 percent of the macrophages formed direct electrical connections with neighboring heart cells. When researchers labeled the immune cells with a fluorescent marker and watched them work, they saw the macrophages pulsing in sync with heart muscle cells.
This matters because macrophages showed longer electrical signals than typical heart cells, meaning they could influence how electrical impulses move through the heart. In developing hearts, this might help coordinate the growing organ. In diseased hearts, it could cause problems.
The mini-hearts with immune cells also consumed more oxygen, contracted harder, and organized their structural proteins differently than those without macrophages. The immune cells were doing cleanup work too, removing dying cells—a job they perform in living hearts.
Triggering Irregular Heartbeats With Inflammation
Next, researchers tested whether they could trigger atrial fibrillation in these mini-hearts. They focused on a protein complex called NLRP3, which kicks off inflammatory responses and has been linked to atrial fibrillation in patients.
Starting on day 30, the team exposed some mini-hearts to a cocktail of three inflammatory molecules: LPS, interleukin-1 beta, and interferon-gamma. These substances are found at high levels in infections and autoimmune diseases. The researchers tested three different dose levels—low, medium, and high—and kept the exposure going through day 64.
The inflamed mini-hearts developed multiple signs of atrial fibrillation. Their electrical activity turned chaotic. Heart cells beat faster and contracted more weakly. Testing showed abnormal electrical firings—the kind that throw off the heart’s rhythm.
To confirm that inflammation was actually causing the irregular beats, researchers treated some mini-hearts with MCC950, a drug that blocks NLRP3. The drug significantly reduced the irregular rhythms and abnormal electrical patterns.
Heart cells still beat faster than normal despite the drug, but the improvement was substantial enough to show that inflammation was driving the electrical chaos.
Macrophages Turn From Helpers to Troublemakers
The immune cells themselves became part of the problem under chronic inflammation. When researchers isolated macrophages from inflamed mini-hearts, they found the cells had ramped up production of inflammatory molecules and switched from their normal supportive role to an inflammatory one.
Interestingly, the macrophages also increased production of an anti-inflammatory molecule, possibly trying to limit the damage—something these cells typically do in living tissue.
When researchers compared mini-hearts with and without macrophages, the immune cells made the irregular heartbeats worse. Both types beat faster under inflammation, but those with macrophages beat significantly faster. The immune cells amplified the electrical problems, likely through a combination of releasing inflammatory signals and being wired into the heart’s electrical system.
A New Tool for Drug Testing
Previous lab models of atrial fibrillation used flat sheets of heart cells or simple 3D structures without immune cells. This new approach gives researchers a more complete picture of how the disease develops.
The mini-hearts could be particularly useful for testing drugs. Because they’re grown from human cells, they might better predict how treatments would work in patients compared to animal studies. The researchers successfully tested them with three different human stem cell lines and kept them alive for 60 days—long enough to study both short-term and long-term disease processes.
The platform could potentially be adapted to study other heart conditions where immune cells play a role, including heart attacks and heart failure.
Paper Summary
Limitations
Like any lab model, these mini-hearts can’t capture everything a real adult heart does. They lack functional blood vessel networks, normal mechanical forces, and several important cell types including neural crest cells and certain immune cells like T cells, B cells, and mast cells. The models also miss systemic influences such as hormonal signals that affect real hearts. For the arrhythmia experiments, the imaging setup used magnification too high to fully map large “re-entry” loops that can occur across the whole mini-heart.
Funding and Disclosures
This work was supported by Michigan State University and grants from the National Institutes of Health and American Heart Association, along with support from the Corewell-MSU Foundation, Corewell Health, ARDF, and the Saving Tiny Hearts Foundation. The senior author, Aitor Aguirre, holds equity in Cytohub and Jaan Biotherapeutics. Aguirre and first author Colin O’Hern are listed as inventors on a related patent.
Publication Details
The study was conducted by Colin O’Hern, Sammantha Caywood, Shakhlo Aminova, Maritza N. Hermosillo, Yifan Wang, Yawen Tang, Adriana Salazar Coariti, Kareen L.K. Coulombe, Chao Zhou, Christopher Contag, and Aitor Aguirre. Institutional affiliations include Michigan State University (Department of Biomedical Engineering, Institute for Quantitative Health Science and Engineering), Brown University (Center for Biomedical Engineering), Stanford University (Department of Pediatrics, Department of Radiology, Department of Microbiology and Immunology), and University of Washington (Department of Bioengineering). The corresponding author is Aitor Aguirre (aaguirre@msu.edu). The paper was published in Cell Stem Cell, Volume 32, pages 1671-1690, on November 6, 2025. The DOI is 10.1016/j.stem.2025.09.011. The article is open access and was published by Elsevier Inc.







