
pexels.com
ATLANTA — Researchers at Georgia State University have turned to an unexpected friend in their quest to combat HIV: llamas. Yes, you read that right – those woolly, long-necked creatures typically associated with the Andes mountains might hold the key to neutralizing one of the most persistent viruses of our time.
Led by Assistant Professor of Biology Jianliang Xu, the research team has engineered tiny but powerful molecules derived from llama antibodies that can target and neutralize a wide range of HIV-1 strains. HIV-1 is the most common form of the human immunodeficiency virus, which causes AIDS.
“This virus has evolved a way to escape our immune system. Conventional antibodies are bulky, so it’s difficult for them to find and attack the virus’ surface,” Xu explains in a media release. “These new antibodies can do this in an easier way.”
So, why llamas?
For about 15 years, scientists have been interested in animals from the camelid family — which includes llamas, alpacas, and camels — because of their unique antibody structure. These animals produce special antibodies that are smaller and more nimble than human antibodies, making them better at identifying and neutralizing foreign invaders like viruses.
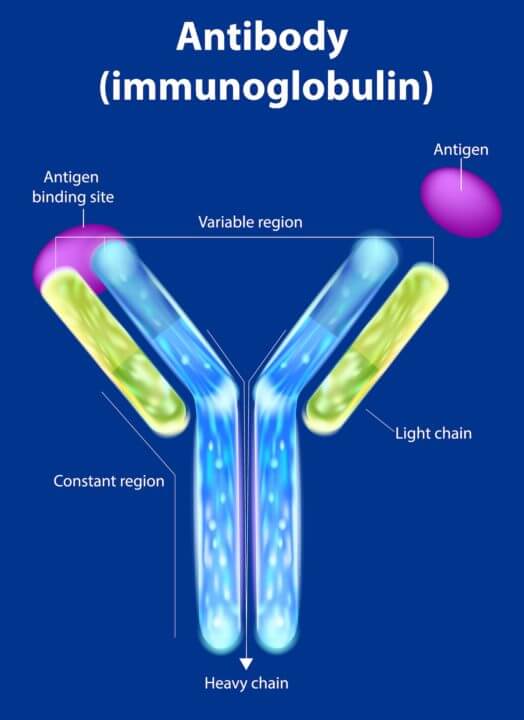
The star players in this research, published in the journal Advanced Science, are called “nanobodies.” These are engineered antibody fragments about one-tenth the size of a conventional antibody. They’re derived from Y-shaped heavy chain-only antibodies found in camelids, which lack the light chains present in human antibodies. This unique structure gives them an edge in fighting certain viruses.
To create these nanobodies, the research team first immunized llamas with a specially designed protein. This triggered the llamas’ immune systems to produce neutralizing nanobodies. The scientists then identified the most promising nanobodies – those that could target vulnerable spots on the HIV virus.
However, the real magic happened when the team engineered these nanobodies into a “triple tandem format.” In simpler terms, they repeated short lengths of the nanobody DNA three times. The result was astonishing: these supercharged nanobodies could neutralize 96 percent of a diverse panel of HIV-1 strains.
Further analysis revealed that these nanobodies work by mimicking the CD4 receptor, a key player in HIV infection. To make them even more potent, the researchers fused the nanobodies with another type of antibody called a broadly neutralizing antibody (bNAb). This fusion created a new antibody with unprecedented neutralizing abilities.
“Instead of developing a cocktail of antibodies, now we can make a single molecule that can neutralize HIV,” Xu says. “We are working with a broadly neutralizing nanobody that can neutralize over 90 percent of the circulating HIV strains, and when we combine that with another bNAb which also neutralizes some 90 percent, together, they can neutralize close to 100 percent.”
The implications of this research are enormous. HIV has long been a formidable foe due to its ability to mutate rapidly and hide from the immune system. A treatment that could neutralize nearly all strains of the virus would be a game-changer in the global fight against HIV/AIDS.
“These nanobodies are the best and most potently neutralizing antibodies to date, which I think is very promising for the future of HIV therapeutics and antibody research,” says Payton Chan, a Ph.D. candidate working with Xu at Georgia State. “I hope one day there will be approval of these nanobodies for the treatment of HIV.”
Looking ahead, Xu and his team plan to explore combining llama nanobodies with other existing bNAbs. Their goal is to neutralize all HIV strains 100%, potentially offering new and more effective treatment options.
Paper Summary
Methodology
The journey began with the immunization of a llama using a specially engineered version of the HIV-1 envelope protein, designed to mimic its structure when the virus is poised to infect a cell. Over multiple immunizations, the llama’s immune system produced a range of potent nanobodies — small, highly stable antibody fragments that llamas and other camelids naturally develop. These nanobodies are exceptional in their ability to bind tightly to specific protein nooks that human antibodies often miss.
Researchers isolated these nanobodies and further engineered them by combining the most effective ones with parts of human antibodies to create bispecific antibodies. These new entities have dual targeting capabilities, potentially increasing their effectiveness at preventing the virus from entering human cells.
Key Results
The hybrid antibodies demonstrated remarkable potency against a wide array of HIV strains. Two standout molecules, named G36 and R27, showed an ability to neutralize 96% of HIV strains tested, achieving this with incredibly low amounts of antibody. This high effectiveness is due to the antibodies’ dual mechanism of action, targeting both a primary site and a secondary site on the virus, which mimics the natural entry point of the virus into human cells.
Study Limitations
The primary challenge is ensuring that these antibodies can be safely and effectively used in humans. The immune systems of llamas and humans differ significantly, so there’s a risk of adverse reactions. Additionally, the production of these antibodies at a scale large enough for widespread clinical use presents logistical hurdles.
Discussion & Takeaways
If these bispecific antibodies prove safe and effective in human trials, they could be used both to treat HIV-positive individuals by halting the progression of the virus and as a preventive measure for those at high risk of HIV infection.
This innovative approach highlights the potential of leveraging the unique aspects of the immune systems of other species, such as llamas, to enhance human health. Moreover, the strategy of creating bispecific antibodies could be applied to other viral diseases, potentially opening new avenues in the prevention and treatment of infectious diseases.
As the global fight against HIV continues, these findings offer a hopeful glimpse into a future where this virus can be effectively controlled or even eradicated. However, further studies and clinical trials are needed to fully understand the potential and safety of these innovative treatments in human populations.







