
Credit: GaudiLab on Shutterstock
While more sunlight is good for everyone, natural light may help diabetic office workers improve blood sugar control.
In A Nutshell
- Natural light improves blood sugar control: People with type 2 diabetes spent 7.6% more time in their target glucose range when exposed to natural daylight through windows compared to artificial office lighting.
- Small but controlled study: Researchers tested 13 participants for just 4.5 days each under both lighting conditions, with each person serving as their own control to ensure accurate comparisons.
- Multiple metabolic benefits observed: Beyond glucose control, natural daylight exposure increased fat burning in the afternoon and boosted evening melatonin production, suggesting stronger circadian rhythms.
- Workplace implications unclear: While the findings suggest office lighting might affect metabolic health, longer studies with more diverse participants are needed to determine real-world applications.
Office workers with type 2 diabetes must frequently check blood sugar levels throughout the day and carefully time their meals and medications, all under the harsh hum of fluorescent lights. Could something as simple as letting in more natural light to workspaces help such employees with glucose control? Research from the Netherlands investigated this possibility.
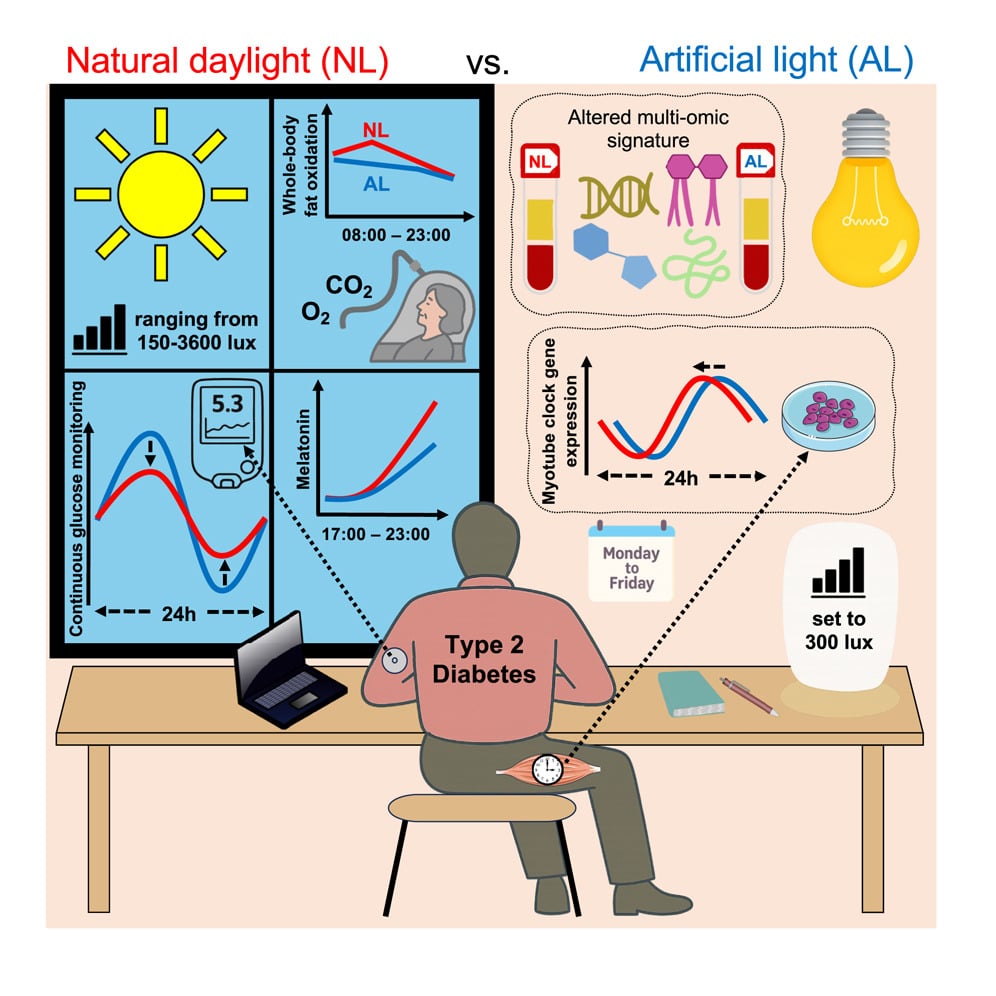
When scientists at Maastricht University Medical Center compared natural daylight exposure to artificial office lighting in people with type 2 diabetes, they observed differences in glucose control. Participants spent 7.6 percentage points more time in their target glucose range when exposed to natural daylight through windows compared to standard artificial lighting. This corresponds to roughly an extra hour and a half per day with blood sugar levels in the target range.
The finding emerges from a crossover study design, in which each participant experienced both lighting conditions. The same 13 people with diabetes experienced both lighting conditions for 4.5 days each, with their glucose levels continuously monitored throughout. This design eliminates the possibility that results simply reflected differences between groups of people, since each participant served as their own control.
The Window Effect on Blood Sugar
The numbers show a difference between lighting conditions. Under natural daylight conditions, participants spent an average of 50.9% of their time in the normal glucose range of 4.4 to 7.2 millimoles per liter. When confined to artificial lighting that blocked natural daylight, that figure dropped to 43.3%. The 7.6 percentage point difference was statistically significant.
Average glucose levels did not change dramatically between the two conditions. Natural daylight was associated with more time in the target glucose range. The researchers measured this using continuous glucose monitors that took readings every 15 minutes, providing an unusually detailed picture of how glucose control fluctuated under different lighting environments.
The study design included several controls. Participants ate identical standardized meals, followed the same sleep schedule, and maintained consistent physical activity during both lighting conditions. Their diabetes medications remained unchanged. Even when they left the controlled environment, they wore special orange-tinted glasses to block blue light, ensuring that the only variable was their daytime lighting exposure.

How Natural Light Affects Metabolism
The glucose improvements weren’t the only changes researchers observed. Natural daylight exposure also shifted how participants’ bodies burned fuel, increasing fat oxidation during afternoon hours compared to artificial lighting. This metabolic change indicates that natural light exposure was associated with changes in substrate metabolism.
The authors propose that the mechanism may involve the circadian clock. Natural daylight, with its dynamic spectrum and intensity that changes throughout the day, provides stronger signals to this internal clock than the static artificial lighting typical of most offices.
Evening measurements revealed another piece of the puzzle: participants produced more melatonin after natural daylight exposure. This hormone, best known for regulating sleep, also plays a role in glucose metabolism. Higher evening melatonin levels suggest that natural daylight helped strengthen participants’ circadian rhythms, which in turn supported better metabolic function.
The researchers even found evidence of these changes at the cellular level. Muscle biopsies showed increased expression of clock genes, and muscle cells cultured from participants displayed altered rhythmic patterns after natural light exposure. These molecular changes may provide biological plausibility for the observed metabolic differences.
What the Study Actually Tested
Before office workers start rearranging their desks, it’s important to understand what this research did and didn’t demonstrate. The study involved just 13 participants, all of whom were older adults with an average age of 70 years. Eight were women, most of whom were post-menopausal. This small, specific population limits how broadly the findings might apply to younger office workers or men with diabetes.
The intervention lasted only 4.5 days per lighting condition — long enough to detect metabolic changes, but far too short to assess whether benefits would persist over weeks or months. The researchers acknowledge this limitation, noting that longer studies are needed to determine whether natural daylight exposure could produce lasting improvements in diabetes management.
The lighting contrast was also deliberately extreme. Participants were either exposed to dynamic natural daylight through windows, with illumination ranging from about 530 to 2,200 lux depending on weather and time of day, or confined to constant artificial lighting at roughly 300 lux with no access to natural daylight. Most real-world office environments fall somewhere between these extremes.
The study took place in the Netherlands between April and October, when daylight hours are relatively long and intense. Whether similar benefits would occur during winter months or in different geographic locations remains an open question.
Implications for Office Workers
Despite these limitations, the findings indicate possible implications for workplace wellness strategies. The researchers suggest that natural daylight exposure “has a positive metabolic impact on individuals with type 2 diabetes and could support the treatment of metabolic diseases.” The key word is “support” — this isn’t about replacing established diabetes care, but potentially complementing it.
For employers, the research suggests that lighting environment may be a factor to consider in workplace wellness programs.
The practical applications remain speculative, however. The researchers note that “future studies could usefully explore if longer-term exposure to natural light could elicit more pronounced effects or if alternative strategies, such as natural light exposure during working commutes, would be sufficient to offset the negative effects of artificial lighting.”
For individuals with diabetes, the findings indicate that the effects of natural daylight exposure during work hours may warrant further discussion with healthcare providers.
The research does not establish that natural daylight exposure improves long-term diabetes outcomes such as HbA1c levels or reduces complications. Those questions require much larger studies conducted over months or years. The study simply shows that lighting environment was associated with differences in glucose control in this sample.
As remote work continues to reshape how and where people work, these findings take on additional relevance. Home offices often have more flexibility in lighting design than traditional corporate environments. The research implies that when setting up a workspace, proximity to windows might matter for more than just the view.
The study provides initial evidence that lighting environment may influence metabolic health in people with diabetes. For the 13 participants in this controlled study, natural daylight through office windows was associated with more time in the target glucose range compared to artificial lighting. Further research is needed to explore practical applications.
Paper Notes
Limitations
The study acknowledges several limitations, primarily regarding the small sample size of 13 participants, which limits statistical power and precision. Additionally, the study population consisted of older individuals (mean age 70 years) and predominantly post-menopausal women, restricting the generalizability of findings to younger or more diverse cohorts with type 2 diabetes. Furthermore, the intervention lasted only 4.5 days per condition and was conducted during a single season (April to October), preventing the assessment of longer-term effects or seasonal variation.
Funding and Disclosures
This work was supported by the VELUX Stiftung, Swiss National Science Foundation, Vontobel Foundation, Olga Mayenfisch Foundation, Ligue Pulmonaire Genevoise, Swiss Cancer League, ISREC Foundation, Gertrude von Meissner Foundation, Swiss Life Jubiläumsstiftung, Swiss Society of Endocrinology and Diabetes, Nutrition 2000plus Foundation, Medical Board of the Geneva University Hospitals, and the Hjelt Foundation. The authors declare no competing interests.
Publication Information
Harmsen, Jan-Frieder, et al. “Natural daylight during office hours improves glucose control and whole-body substrate metabolism.” Cell Metabolism, January 6, 2026. DOI: 10.1016/j.cmet.2025.11.006. The study utilized clinical data from 13 participants (8 females, 5 males) with type 2 diabetes, collected at the Maastricht University Medical Center in the Netherlands between April and October 2022. Jan-Frieder Harmsen and colleagues are affiliated with Maastricht University Medical Center and other collaborating institutions.







