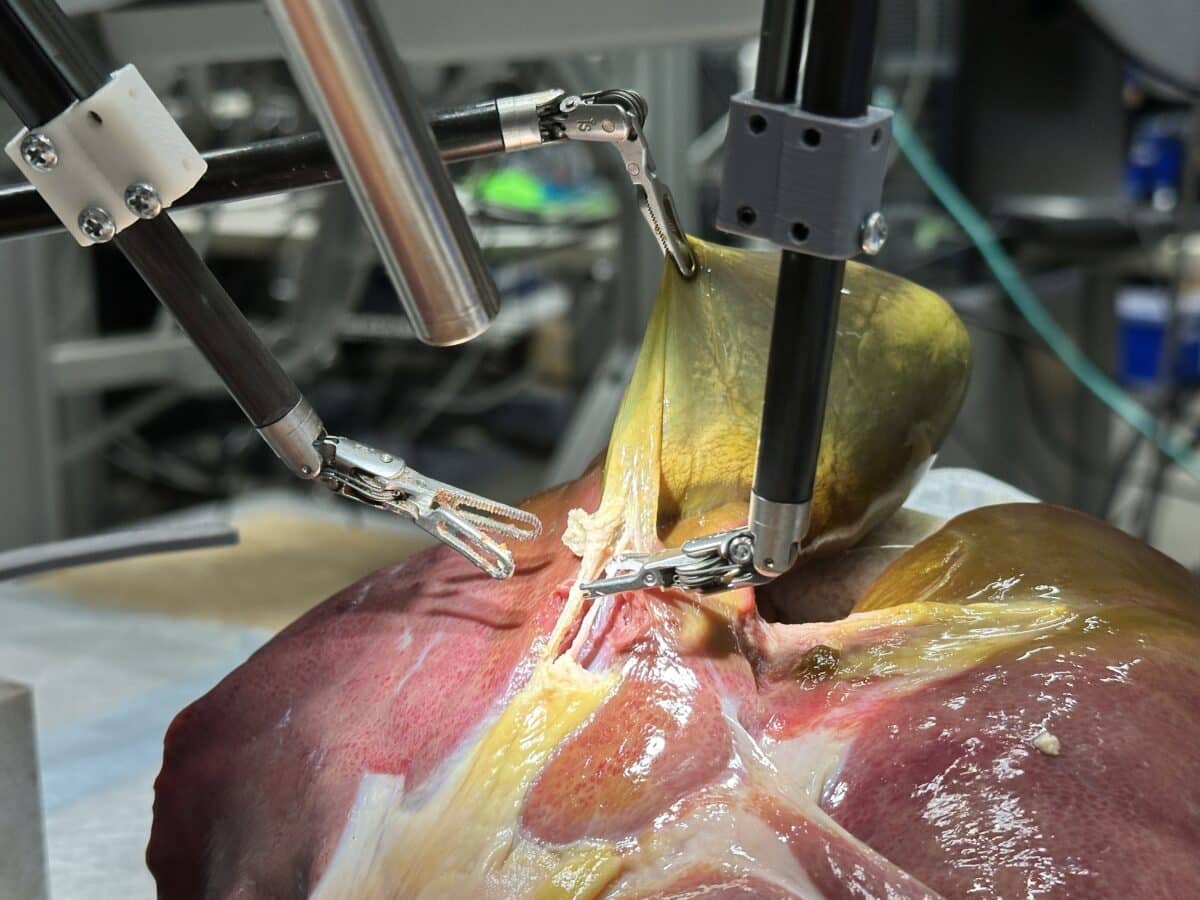
The Surgical Robot Transformer-Hierarchy performing a gallbladder surgery (Credit: Juo-Tung Chen/Johns Hopkins University)
Table of contents
In A Nutshell
- A new robot trained with real surgical footage successfully removed pig gallbladders in a lab, performing all critical steps on its own.
- It achieved a perfect success rate: eight surgeries, zero failures.
- The system used simple language instructions, learned to fix its own mistakes, and was tested on organs similar to human anatomy.
- It’s still early days — the technology hasn’t been used on live patients yet but could one day help with routine surgeries and ease surgeon shortages.
BALTIMORE — A surgical robot has successfully removed pig gallbladders in a lab setting without any hands-on help during the actual surgery steps, completing each operation with a 100% success rate. The new system, developed by researchers at Johns Hopkins University, handled all the critical parts of the procedure by itself, even correcting its own mistakes along the way.
Although a human operator still had to reload surgical clips and switch tools when needed (like a nurse would during a real surgery), the robot made all decisions for the surgical steps on its own, from spotting the right parts of the anatomy to placing surgical clips and making precise cuts. The team says this is the first time a robot has handled an entire surgical procedure, step by step, without direct control. A paper on the achievement was published in Science Robotics.
Teaching Robots to Think Like Surgeons
The secret behind the robot’s success is its two-part artificial intelligence system, which works like an experienced surgeon guiding a medical trainee in the operating room.
The first AI component acts like a lead surgeon: every three seconds, it looks at video from surgical cameras and decides what should happen next, issuing simple commands like “clip the left tube” or “move the right arm higher.” The second AI acts like the surgeon’s hands, turning those instructions into smooth, precise movements 30 times a second.
To train the system, the researchers recorded 17 hours of real gallbladder removal practice on pig organs taken from butcher shops and used for medical training. They captured more than 16,000 examples of the steps involved, including common mistakes and how to fix them, so that the robot could learn how to adjust on its own when something goes wrong.

How the Robot Surgeon Did
When tested, the robot completed all 17 steps needed to remove a gallbladder, including grabbing tissue, placing clips to seal off ducts and arteries, and cutting them. Each procedure took about five minutes on average, not counting time for the human assistant to reload clips and swap tools.
The robot proved it could adapt when things didn’t go exactly as planned. In some tests, the researchers deliberately put it in tricky positions, such as having to grab tissue at an odd angle. The system figured out how to fix the problem by itself. On average, it made about six self-corrections per surgery.
When compared to a simpler version of the AI that didn’t have this layered approach or built-in corrections, the new system was far more reliable. The basic model only succeeded about a third of the time, while the full version got it right every time.
“The motion of the robot felt very human and it felt like some living being was controlling it,” lead author Ji Woong “Brian” Kim, a former postdoctoral researcher at Johns Hopkins who’s now with Stanford University, tells StudyFinds. “This made sense — the robot was trained to imitate human motions, but still, its ability to self-correct mistakes and perform intelligent behavior was quite exhilarating to watch.”
Looking Ahead: How Robotics Might Help Patients
While these tests used pig organs in a lab, not live animals or humans, the breakthrough brings us closer to real surgical robots that can take on bigger roles in operating rooms. In the United States alone, surgeons remove over 700,000 gallbladders every year. Smart robots like this could help hospitals handle routine surgeries, especially in places where there aren’t enough trained surgeons.
“Just as surgical residents often master different parts of an operation at different rates, this work illustrates the promise of developing autonomous robotic systems in a similarly modular and progressive manner,” said co-author Jeff Jopling, a Johns Hopkins surgeon.
Importantly, these systems aren’t designed to replace surgeons entirely. Instead, they could take care of straightforward, repetitive steps, freeing up human surgeons to focus on complex parts of an operation or unexpected problems. Because the robot understands simple spoken instructions, surgeons could step in to guide it if needed, just like training a resident.
“This advancement moves us from robots that can execute specific surgical tasks to robots that truly understand surgical procedures,” said medical roboticist Axel Krieger. “This is a critical distinction that brings us significantly closer to clinically viable autonomous surgical systems that can work in the messy, unpredictable reality of actual patient care.”
Of course, plenty of hurdles remain before this kind of system is used on real patients. The robot still needs to be tested inside the body, where it would have to work around bleeding, moving organs, and tight spaces. The cameras it uses today are also too big for standard surgical tools, so they’ll need to be made smaller.
Patient safety will always come first. The team behind this research says future versions could check their own confidence and ask a human surgeon for help when they’re unsure. They might even be able to run a virtual test of each step before doing it for real. For now, this study shows that robots can do more than single tasks, they’re learning to handle entire surgeries from start to finish.
StudyFinds’ Q&A With Lead Author Dr. Brian Kim
Why did you choose gallbladder removal as your test procedure?
Cholecystectomy was the first procedure that was performed laparascopically, and it is a very common procedure performed at ~700k times a year in the U.S. alone. We thought it would be meaningful and impactful to automate such a common procedure that many people know.
What was the biggest technical hurdle in getting the robot to self-correct its own mistakes?
The most challenging part was figuring out how we could design the robot model to correct itself. To accomplish this, we decided that the robot should have two choices: either generate task instructions or corrective instructions. Dividing the instruction into these two types made it more clear to the robot when self-correction was needed.
How did you decide to use simple natural language instructions instead of more complex interfaces?
We thought about how experienced surgeons would instruct surgical residents by talking to them during the surgery. We thought this already felt quite natural to what surgeons were doing, and it also seemed like the easiest way to control the robot — just tell it what to do.
In your opinion, what would a hospital need to change to safely adopt this kind of system in the real world?
If autonomous systems got reliable enough to be deployed in hospitals, the users of the systems should understand how to set up the robot and understand its limitations clearly.
What surprised you the most when watching the robot perform the procedure for the first time on its own?
The motion of the robot felt very human and it felt like some living being was controlling it. This made sense — the robot was trained to imitate human motions, but still, its ability to self-correct mistakes and perform intelligent behavior was quite exhilarating to watch.
What safety features are you most focused on improving before moving to human trials?
We are first moving to in-vivo trials using animals first. But if doing human trials, we really need to stress-test the system at its limits to ensure that it will work very well in very difficult scenarios, at least as reliable as a human. A good safety feature would be some way to interpret the confidence of the model’s predictions, so that we can judge how confident the robot is in certain scenarios.
How far away do you think we are from seeing robots like this assisting surgeons during live operations?
It’s very hard to predict the future. If I had to guess, we might have some robots with very simple functionalities in the next 5 – 10 years. But I may be way off.
Do you see this technology eventually helping rural hospitals or regions with too few trained surgeons?
Definitely. One of the big motivations for autonomous surgery is to provide greater access to care.
Paper Summary
Methodology
The researchers developed a two-level AI system called SRT-H (Surgical Robot Transformer – Hierarchy) that performs gallbladder removal surgery autonomously. The high-level policy processes visual information from surgical cameras every 3 seconds to decide what task should be performed next (like “grab gallbladder” or “clip artery”). It can also identify when corrections are needed and issue commands like “move left arm higher.” The low-level policy receives these language instructions and translates them into precise robot movements at 30 Hz. The team collected 17 hours of surgical demonstrations from experienced operators using 34 pig gallbladders, totaling over 16,000 recorded movements. They used imitation learning to train the AI system, including examples of both optimal performance and recovery from mistakes.
Results
The autonomous surgical system achieved a 100% success rate across all 8 test gallbladders, completing all 17 subtasks without human intervention. Each procedure took an average of 317 seconds (about 5 minutes), with the robot making an average of 6.4 self-corrections per operation. When compared to simplified versions, the full system dramatically outperformed alternatives: an end-to-end approach achieved only 33% success, while versions without corrective capabilities or specialized cameras showed significantly degraded performance. In preliminary comparisons with an expert surgeon, the robot took longer to complete tasks but demonstrated smoother, more efficient movements with shorter trajectory lengths and lower motion jerk.
Limitations
The study was conducted on ex-vivo (removed) pig organs in a controlled laboratory environment, without the challenges of breathing motion, bleeding, or the confined spaces of minimally invasive surgery. The current wrist camera configuration is too bulky for standard laparoscopic ports, though the researchers note that modern sub-millimeter cameras could address this. The system requires manual tool changes and clip reloading between steps. Additionally, approximately 10% of gallbladders were excluded due to anatomical variations like crossing arteries or branching structures that the current system cannot handle.
Funding or Disclosures
This research was supported by NSF/FRR grant 2144348, NIH grant R56EB033807, NSF DGE fellowship 2139757, and ARPA-H grant AY1AX000023. The authors declared no competing interests.
Publication Info
The paper “SRT-H: A Hierarchical Framework for Autonomous Surgery via Language Conditioned Imitation Learning” was published in Science Robotics on July 9, 2025. It was authored by Ji Woong (Brian) Kim, Juo-Tung Chen, Pascal Hansen, Lucy X. Shi, Antony Goldenberg, Samuel Schmidgall, Paul Maria Scheikl, Anton Deguet, Brandon M. White, De Ru Tsai, Richard Cha, Jeffrey Jopling, Chelsea Finn, and Axel Krieger from Johns Hopkins University, Stanford University, and Optosurgical. Corresponding author: Axel Krieger (axel@jhu.edu).








Who wrote this article? A nurse loads the clips “like a nurse would during a real surgery”? Clearly you haven’t been in the OR. However, this is something all surgeons need to pay attention to…