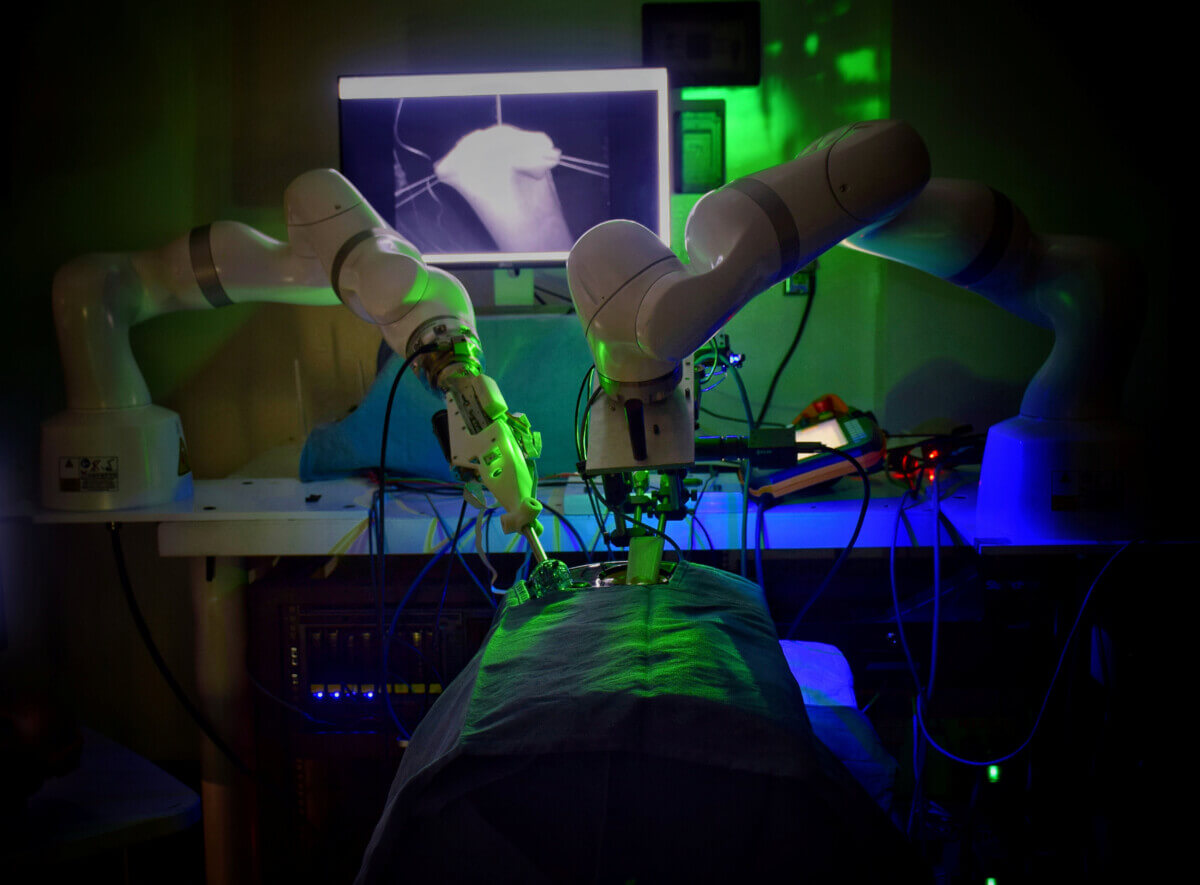
The Smart Tissue Autonomous Robot can perform laparoscopic surgery on the soft tissue of a pig without human help.
BALTIMORE, Md. — Robots helping doctors perform surgery has become a common sight in modern medicine. However, a team from Johns Hopkins University says a robot has successfully performed the first laparoscopic surgery — without a doctor to guide it through the procedure.
Laparoscopic (or “keyhole”) surgery is a common, minimally invasive procedure which inserts a camera inside a tube into the abdomen or a woman’s reproductive system to check for problems.
The procedure, performed on a pig, is a major step towards fully autonomous operations on patients. During the surgery, the robot called STAR (Smart Tissue Autonomous Robot) successfully reconnected two ends of the intestine.
Researchers says STAR actually performed better than real surgeons, who deviated more from the ideal cut line — causing more tissue damage.
“Our findings show that we can automate one of the most intricate and delicate tasks in surgery: the reconnection of two ends of an intestine. The STAR performed the procedure in four animals and it produced significantly better results than humans performing the same procedure,” says senior author Dr. Axel Krieger, a mechanical engineer at Johns Hopkins, in a university release.
Laparoscopic surgery takes nerves of steel
The procedure is arguably the most challenging task in gastrointestinal surgery, requiring a high level of accuracy and consistency. Even the slightest hand tremor or misplaced stitch can result in a leak — with potentially catastrophic complications for the patient.
Scientists specifically designed the vision-guided system to suture soft tissue. STAR is an improvement over a 2016 model created by the same team that successfully repaired a pig’s intestines but required a large incision and more help from humans.
STAR has an infrared camera and new features for enhanced independence and improved precision. They include specialized suturing tools and state-of-the art scanners that provide more accurate visualizations of the surgical field.
Soft-tissue surgery is especially hard for robots because of its unpredictability. Dr. Krieger adds it forces the technology to adapt quickly to handle unexpected obstacles.
‘More accuracy and precision’ from patient to patient
STAR has a novel control system that can adjust the surgical plan in real time, just as a human surgeon would.
“What makes the STAR special is that it is the first robotic system to plan, adapt, and execute a surgical plan in soft tissue with minimal human intervention,” Dr. Krieger explains.
A structural-light based 3D tube, or endoscope, and machine learning-based tracking algorithm guides STAR.
“We believe an advanced three-dimensional machine vision system is essential in making intelligent surgical robots smarter and safer,” says co-author Professor Jin Kang.
As the medical field moves towards more keyhole approaches for surgeries, it will be important to have an automated robotic system designed for such procedures to assist.
“Robotic anastomosis is one way to ensure that surgical tasks that require high precision and repeatability can be performed with more accuracy and precision in every patient independent of surgeon skill,” Krieger says. “We hypothesize that this will result in a democratized surgical approach to patient care with more predictable and consistent patient outcomes.”
Keyhole surgery has a number of benefits such as the reduced risk of infection and pain in comparison to standard surgery. Patients are able to go home quicker, freeing up space in hospitals. Dr. Krieger believes robots will one day be on the battlefield, performing trauma surgery on wounded soldiers.
Although mechanical systems consisting of robotic arms with laparoscopic instruments have been helping patients over the last few years, there has always been a doctor in control — until now.
STAR is described in the journal Science Robotics.
South West News Service write Mark Waghorn contributed to this report.







