
This discovery may produce new pain management options for arthritis patients. (© narstudio - stock.adobe.com)
Discovery opens door to potentially game-changing drug for patients with chronic inflammatory diseases
In A Nutshell
- Researchers discovered that chemical brake signals in the blood control when certain immune cells stop multiplying during inflammation, and blocking the enzyme that breaks down these signals reduced a type of white blood cell linked to chronic inflammatory diseases
- In a study of 49 healthy volunteers with controlled inflammation, the drug GSK2256294 significantly lowered intermediate monocytes without blocking the body’s initial inflammatory response to infection
- Intermediate monocytes are elevated in rheumatoid arthritis, lupus, cardiovascular disease, and other chronic inflammatory conditions, making them a potential therapeutic target
For millions of people living with rheumatoid arthritis, lupus, or chronic inflammatory conditions, the immune system never seems to accept there is no threat present. Inflammation that should resolve in days or weeks instead persists for months or years, gradually destroying healthy tissue. Now scientists may have found a crucial piece of the puzzle: a molecular “brake pedal” that tells inflammation when to wind down.
Researchers at University College London discovered that chemical messengers in the blood act like traffic signals for immune cells during inflammation, telling them when to multiply and when to stand down. When they gave healthy volunteers a drug that keeps these brake signals active longer, a specific type of immune cell linked to chronic disease dropped significantly. Crucially, it also didn’t appear to interfere with the body’s initial inflammatory response.
The breakthrough centers on intermediate monocytes, white blood cells that normally appear briefly during inflammation but get stuck at elevated levels in people with chronic inflammatory diseases.
How the Body Normally Winds Down Inflammation
When the body detects infection or injury, classical monocytes flood into the affected area as first responders. Some of these cells transition into intermediate monocytes, which help coordinate the immune response. Under normal circumstances, chemical brake signals tell these cells to stop multiplying once the threat passes. But in chronic inflammatory conditions, something goes wrong with this signaling system.
The study, published in Nature Communications, studied 49 healthy volunteers who received small injections of killed bacteria in their forearms to trigger localized inflammation. Some received a drug called GSK2256294 either before or after the injection that blocks an enzyme responsible for breaking down the body’s natural brake signals. Blood samples and tissue analysis over three days revealed that people who got the drug had dramatically fewer intermediate monocytes, both in their bloodstream and at the inflammation site.
Moreover, the drug didn’t prevent the main visible signs of acute inflammation like swelling, redness, or local temperature increases. But it did speed up pain resolution, and more importantly, it demonstrated precise control over a cell type that researchers increasingly recognize as problematic in chronic disease.
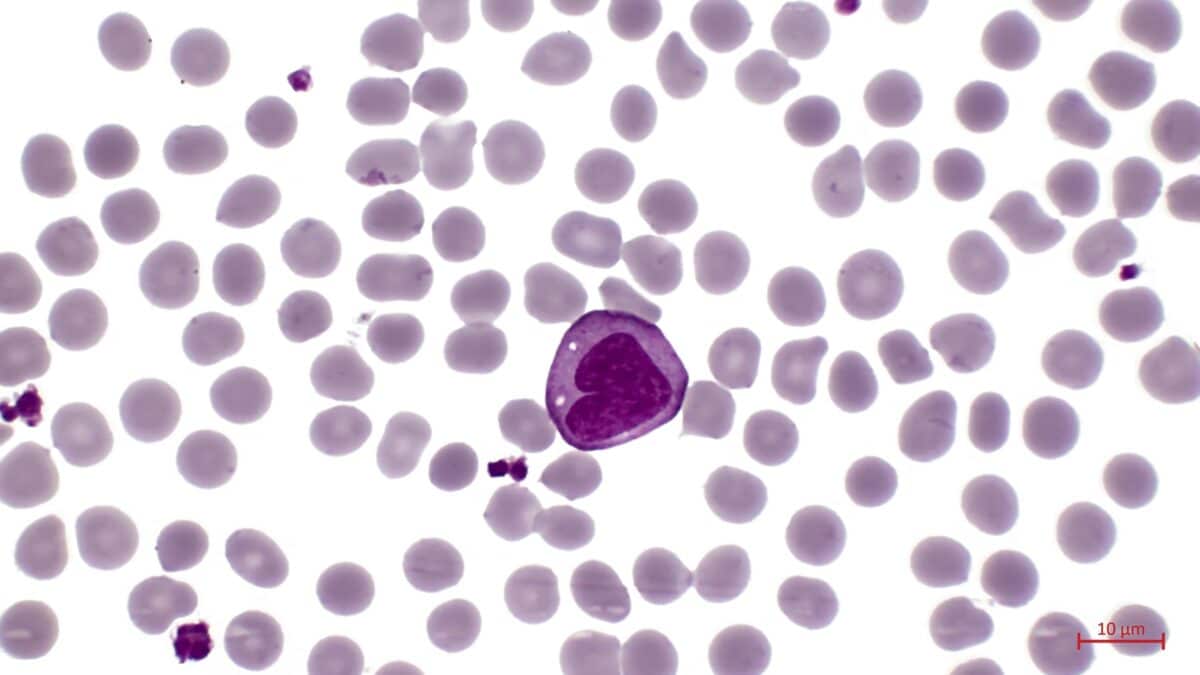
The Immune Cell That Won’t Leave
Laboratory experiments revealed the mechanism behind this effect. The natural chemical signals that the drug preserves work by blocking a protein that normally drives monocyte development. When researchers tested this in isolated immune cells, they could prevent classical monocytes from transitioning into intermediate monocytes, essentially stopping them from getting stuck in that problematic middle stage.
To confirm the finding, volunteers in a separate experiment took a different drug that blocks the same protein through a different pathway. After four days, their intermediate monocyte levels also dropped, supporting the conclusion that controlling this specific protein can dial down these cells.
What makes intermediate monocytes so interesting is that they’re elevated in nearly every major chronic inflammatory condition. People with cardiovascular disease, obesity-related inflammation, and autoimmune disorders like rheumatoid arthritis all show abnormally high levels. These cells appear helpful during short-term inflammation (they maintain other immune cells and help coordinate healing) but when they persist, they enhance tissue destruction.
The findings also revealed when these natural brake signals peak during inflammation. The chemical messengers reached their highest levels 14 hours after the bacterial injection: right at the transition point between active inflammation and the beginning of resolution. This timing suggests the body has built-in mechanisms to wind down the immune response, and chronic inflammatory diseases may represent a failure of these natural brakes.
A Different Approach to Anti-Inflammatory Treatment
Current anti-inflammatory drugs work like sledgehammers, broadly suppressing the immune system and often leaving patients vulnerable to infection. The ability to selectively reduce one type of immune cell, particularly one that’s consistently elevated in chronic disease, could represent a fundamentally different treatment strategy.
The drug used in the study, GSK2256294, has already been tested in humans and shown to be safe and well-tolerated. A single 15mg dose blocks more than 99% of the target enzyme within two hours, with effects lasting up to 30 hours. That safety profile makes it an attractive candidate for testing in people with chronic inflammatory diseases, where elevated intermediate monocytes are already a known problem.
Of course, whether blocking this enzyme will prove effective in actual disease remains to be seen. The study focused on healthy volunteers with short-term, controlled inflammation, not patients with established chronic conditions. Real-world chronic inflammation involves months or years of dysregulation, not the 48-72 hours studied here. Still, the fact that the same cell type consistently appears at elevated levels across so many different chronic inflammatory diseases suggests this pathway might matter beyond just acute inflammation.
By identifying a molecular brake that controls the appearance of cells consistently linked to chronic inflammation, the research opens the door to a more targeted approach than simply suppressing inflammation across the board. If this pathway proves relevant in chronic disease, it could offer a way to help those living with inflammatory conditions.
Disclaimer: This research was conducted in healthy volunteers using a controlled inflammation model and tracked responses for only 48-72 hours. The findings have not been tested in patients with chronic inflammatory diseases. Whether this approach will prove effective for treating conditions like rheumatoid arthritis, lupus, or cardiovascular disease remains unknown and will require additional clinical trials. Anyone with a chronic inflammatory condition should consult their healthcare provider before making any changes to their treatment plan.
Paper Notes
Limitations
The study focused exclusively on healthy male volunteers between ages 18-50, limiting generalizability to women, older adults, and individuals with existing inflammatory conditions. The inflammation model used UV-killed bacteria in skin, which may not fully represent inflammation in other tissues or from different causes. Sample sizes varied between 5-12 participants in different experimental arms due to participant refusal or technical issues with sample collection. The study tracked inflammation for only 48-72 hours, providing limited insight into longer-term resolution processes. Lipidomic analysis could not detect all potential epoxy-oxylipins and their metabolites. The study did not examine whether reduced intermediate monocytes translated to improved clinical outcomes in actual disease states.
Funding and Disclosures
This work was supported by an Arthritis UK studentship award to Bracken/Gilroy, a Biotechnology and Biological Sciences Research Council (BBSRC) research grant (BB/X016854/1 to D.W.G), the Division of Intramural Research at the National Institute of Environmental Health Sciences (NIEHS), NIH (Z01 ES025034 to D.C.Z), a Medical Research Council (MRC) Grand Challenge in Experimental Medicine (MICA) Grant (MR/M003833/1 to A.N.A), and a BBSRC research grant (BB/Y003365/1 to A.N.A). O.V.B. and D.W.G. have filed a patent application with the US Patent Office for the use of GSK2256294 in treating chronic inflammatory disease. All other authors declared no competing interests.
Publication Details
Authors: Olivia V. Bracken, Parinaaz Jalali, James R. W. Glanville, Larrissa Benvenutti, Emma S. Chambers, Hugh Trahair, Madhur Motwani, Karen T. Feehan, Jamie G. Evans, Jhonatan de Souza Carvalho, Roel P. H. De Maeyer, Arne N. Akbar, Fred B. Lih, Darryl C. Zeldin, David Bishop-Bailey, Matthew L. Edin, Derek W. Gilroy | Affiliations: Department of Ageing, Rheumatology and Regenerative Medicine, Division of Medicine, University College London (primary); Centre for Immunobiology, Blizard Institute, Queen Mary University of London; School of Cancer and Pharmaceutical Sciences, King’s College London; Nuffield Department of Orthopaedics, Rheumatology and Musculoskeletal Sciences, University of Oxford; Division of Intramural Research, National Institute of Environmental Health Sciences, NIH | Journal: Nature Communications | Publication Date: January 16, 2026 | Volume/Issue: 17:431| DOI: 10.1038/s41467-025-67961-5 | Received: January 25, 2025| Accepted: December 12, 2025 | License: Open Access under Creative Commons Attribution 4.0 International License








Good luck on improving on hundreds of millions of years of evolution. There may be some particular instances when this new knowledge can help. And this research may be pivotal, but only time will tell.
Just go carnivore for 6 months…. all inflammation gone! Beef and eggs only. at 39-40 I couldn’t run for the life of me! I’m a Marine… we ran all day until the runnin’ was done! Carnivore now for almost 3.5 years now, I run like the wind almost everyday! zero pain. You don’t need to dr ugs!!