
Photo by Brett_Hondow from Pixabay
ADELAIDE, Australia — Your bathroom sink might be cleaner than a hospital’s – but that’s not necessarily good news. A surprising new study reports that residential handwashing basins often harbor more potentially harmful bacteria than their hospital counterparts, raising concerns about home hygiene practices.
The study, led by Claire Hayward and colleagues from Flinders University in Australia, examined biofilms – thin, slimy layers of microorganisms that adhere to surfaces – found on faucets and drains in both hospital and residential settings. Their findings paint a concerning picture of the microbial world lurking in our sinks.
The team collected biofilm samples from 20 handwashing basins, half from hospitals and half from residential properties. Using advanced DNA sequencing techniques, they identified a diverse array of bacteria present in these biofilms, including some known to cause infections and others capable of corroding plumbing materials.
One of the most surprising discoveries was the significant difference between hospital and residential sink biofilms. While you might expect hospital sinks to be cleaner due to strict hygiene protocols, the reality is more complex. The researchers found that residential sinks, particularly drains, harbored higher levels of certain concerning bacteria, including Legionella – the bacterium responsible for Legionnaires’ disease.
This finding highlights a potential blind spot in our approach to infection control. While hospitals have rigorous cleaning and maintenance procedures, residential properties often lack such oversight. As healthcare increasingly moves into home settings, with services like at-home chemotherapy and post-surgical care becoming more common, this gap in hygiene practices could pose unforeseen risks to vulnerable patients.
The study, published in Science of The Total Environment, also revealed that biofilms in hospital sinks showed less variation between faucets and drains compared to those in residential sinks. This consistency in hospital environments might be due to regular, standardized cleaning practices. However, it also suggests that these cleaning methods, while thorough, may not be effectively eliminating all potentially harmful bacteria.
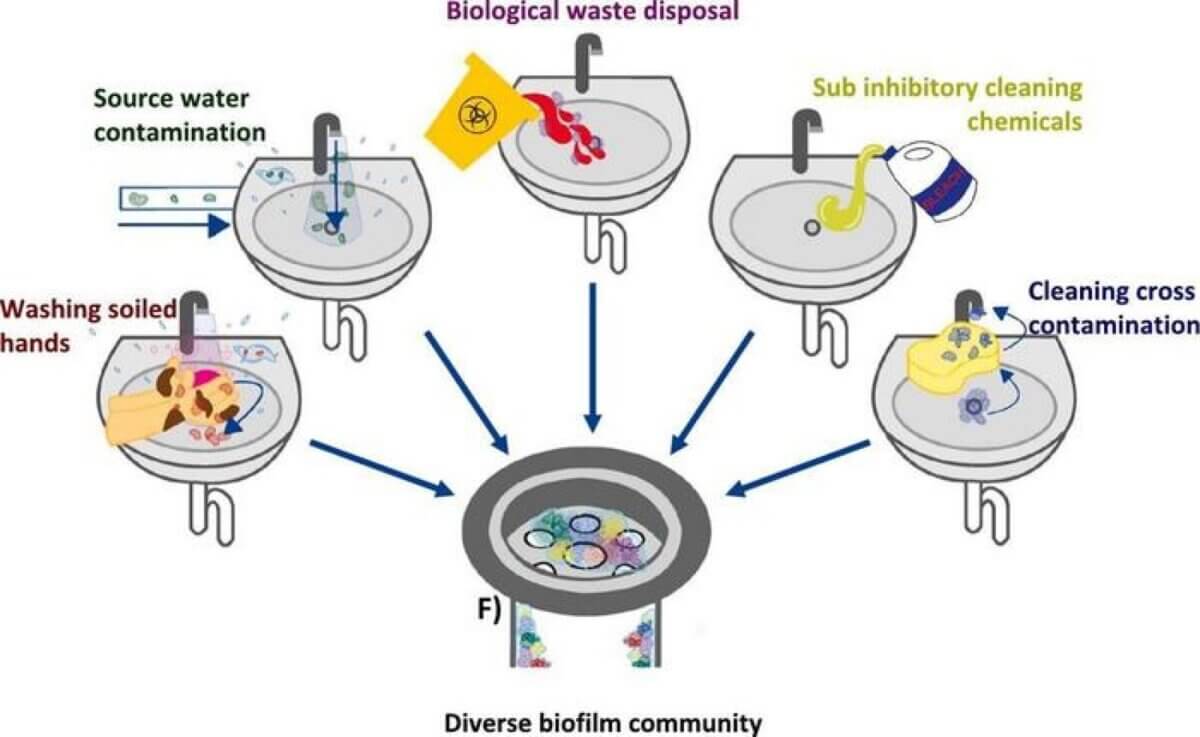
Among the concerning microbes identified were “opportunistic premise plumbing pathogens” (OPPPs). These bacteria are particularly adept at surviving and thriving in building water systems. The study found seven genera of OPPPs, including Pseudomonas and Legionella, with some showing higher prevalence in residential settings.
The researchers also identified bacteria capable of corroding plumbing materials, which could lead to infrastructure damage and create more hiding spots for harmful microbes. This finding underscores the potential for a vicious cycle where bacterial growth leads to material degradation, which in turn provides more surfaces for bacteria to colonize.
Perhaps most alarmingly, the study found evidence of bacteria resistant to common antibiotics and disinfectants. This includes methicillin-resistant Staphylococcus aureus (MRSA) and other “superbugs” that pose significant challenges in healthcare settings. The presence of these resistant bacteria in sink biofilms suggests that our cleaning practices may be inadvertently creating selective pressures that favor the survival of these dangerous microbes.
“The difference in the diversity of the microbial communities could be due to more regular cleaning, usage and the design of basins in hospitals through the implementation of healthcare infection control practices,” Hayward says in a media release.
“This poses a risk to patients receiving healthcare in the home which has been emerging as an alternative to extensive inpatient hospital stays to reduce the burden on the healthcare system.”
The study calls into question our current approaches to infection control, especially in residential settings where healthcare is increasingly being delivered. The researchers suggest that we need to rethink how we design, use, and maintain our handwashing basins to minimize the risk of bacterial growth and spread.
For the average person, this study serves as a wake-up call to pay more attention to sink hygiene. Regular cleaning of both faucets and drains, using appropriate disinfectants, could help control bacterial growth. However, the researchers caution that improper use of disinfectants could potentially make the problem worse by selecting resistant bacteria.
As we continue to face global health challenges, including the rise of antibiotic-resistant bacteria, studies like this highlight the importance of understanding the microbial ecosystems in our immediate environments. The sink, a fixture we use daily for hygiene, may paradoxically be a source of hidden danger if not properly managed.
In the end, this study reminds us that in the world of public health, even the most mundane fixtures in our homes can play a significant role. The next time you wash your hands, remember that the battle against harmful bacteria extends beyond just scrubbing your palms – it includes maintaining the very systems we rely on to keep us clean.
Paper Summary
Methodology
The researchers collected biofilm samples from 20 handwashing basins (11 residential and 9 hospital) using sterile swabs. They swabbed both the faucet and drain of each basin. The collected samples were processed to extract DNA, which was then amplified and sequenced to identify the types of bacteria present. This technique, known as 16S rRNA gene amplicon sequencing, allows researchers to identify bacteria based on their genetic material, even if they can’t be grown in a lab. The team then used various statistical methods to analyze the differences in bacterial communities between hospital and residential sinks, and between faucets and drains.
Key Results
The study found significant differences in bacterial communities between hospital and residential sinks. Residential sinks, especially drains, had higher levels of certain bacteria, including Legionella. Hospital sink biofilms showed less variation between faucets and drains.
The researchers identified 19 potentially pathogenic bacterial genera, 38 potentially corrosive genera, and 20 strong biofilm-forming genera. Some bacteria, like Pseudomonas, were more common in drains, while others, like Methylobacterium-Methylorubrum, were more prevalent in faucets. The study also found evidence of antibiotic-resistant bacteria in the biofilms.
Study Limitations
The study had a relatively small sample size of 20 handwashing basins, which may not be fully representative of all situations. The researchers couldn’t collect detailed information about the buildings or cleaning practices due to privacy concerns, which could have provided more context for the findings.
The study also focused on identifying genera of bacteria rather than specific species, which limits the ability to pinpoint exact pathogens. Additionally, the presence of bacteria doesn’t necessarily mean they will cause infections; the study didn’t assess the viability or infectivity of the detected microbes.
Discussion & Takeaways
This study highlights the potential for handwashing basins to harbor diverse and potentially harmful bacterial communities. It suggests that current cleaning practices, especially in residential settings, may not be adequate to control these microbes. The findings underscore the need for more attention to sink hygiene in home healthcare settings.
The study also points to the potential for sink design to influence bacterial growth, suggesting that changes in sink construction could help mitigate risks. Overall, the research calls for a reevaluation of our approach to maintaining clean water systems in both healthcare and residential environments.
Funding & Disclosures
The study was supported by the Flinders Foundation: Health Seed Grant 2021. One of the authors, Jason Hinds, is employed by Enware Australia Pty Ltd., a company involved in plumbing fixtures. The other authors declared no competing interests.







