
(© fahrwasser - stock.adobe.com)
NEW YORK — Intermittent fasting is all the rave these days, with more and more people claiming that it helps improve various aspects of health. A new study by researchers at the Icahn School of Medicine at Mount Sinai contradicts these claims, however, suggesting that skipping breakfast could hinder the body from fighting off infections. The team adds that missing the “most important meal of the day” could even lead to an increased risk of heart disease.
“There is a growing awareness that fasting is healthy, and there is indeed abundant evidence for the benefits of fasting. Our study provides a word of caution as it suggests that there may also be a cost to fasting that carries a health risk,” says lead author Filip Swirski, PhD, Director of the Cardiovascular Research Institute at Icahn Mount Sinai, in a media release. “This is a mechanistic study delving into some of the fundamental biology relevant to fasting. The study shows that there is a conversation between the nervous and immune systems.”
In order to better understand how short-term (only a few hours) and long-term (24 hours) fasting impacts the immune system, the research team analyzed two groups of mice. One group ate breakfast (their largest meal of the day) right after waking up. The other group skipped breakfast entirely. They then collected blood samples from both groups at baseline upon waking up, after four hours, and again after eight hours.
The team observed a distinct difference in the fasting group. They noticed a change in the number of monocytes, which are white blood cells made in the bone marrow that make their way into the blood and tissues to help fight infection, heart disease, and even cancer. At baseline, everyone had the same number of them. After four hours, however, a staggering 90 percent of the cells were no longer in the bloodstream in the fasting group. This got even worse after eight hours. Monocyte counts stayed the same in the non-fasting group.
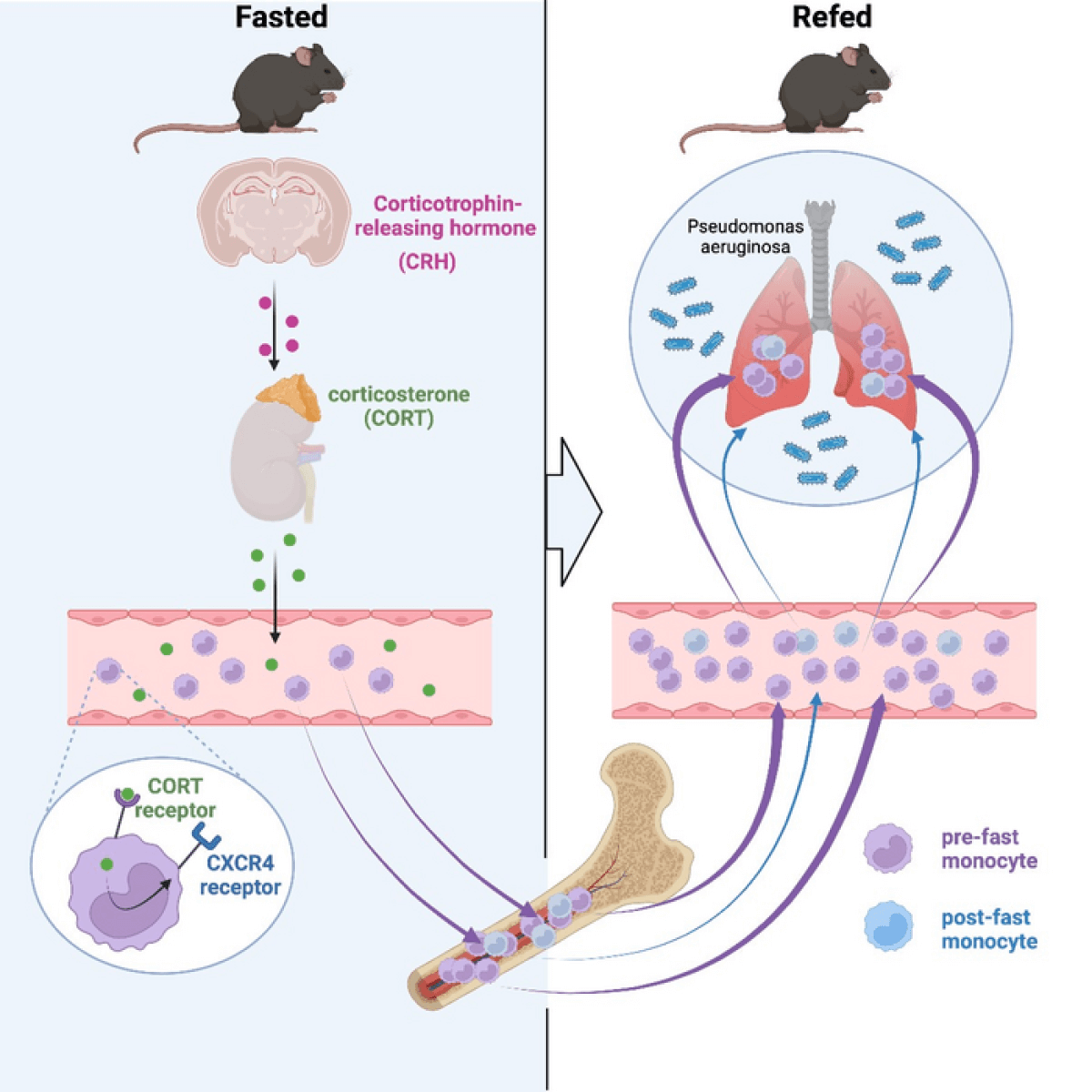
The researchers found that in the fasting group, the monocytes went back into the bone marrow and new cell production within the bone marrow did not occur. Usually in the bone marrow, these cells have a short lifespan. However, in fasting animals, monocytes lived longer in the bone marrow and aged differently than those remaining in the bloodstream.
Additionally, they found that the brain controls monocyte response. Fasting caused a stress response in the brain which induces a feeling of being “hangry ” — the combination of hunger and anger. This ultimately triggers the monocytes to shift back into the bone marrow.
“The study shows that, on the one hand, fasting reduces the number of circulating monocytes, which one might think is a good thing, as these cells are important components of inflammation. On the other hand, reintroduction of food creates a surge of monocytes flooding back to the blood, which can be problematic. Fasting, therefore regulates this pool in ways that are not always beneficial to the body’s capacity to respond to a challenge such as an infection,” explains Dr. Swirski. “Because these cells are so important to other diseases like heart disease or cancer, understanding how their function is controlled is critical.”
The study is published in the journal Immunity.







