
While pain may not be present, many people in their 30s already have joint damage. (© Dragana Gordic - stock.adobe.com)
CHICAGO — Two new studies have found that steroid injections for knee pain related to osteoarthritis can actually make things worse for patients.
Researchers from the University of California-San Francisco and Chicago Medical School of Rosalind Franklin University say that both MRI scans and X-ray imaging showed that steroid injections significantly exacerbated the progression of knee osteoarthritis. In the United States, this condition is the most common form of arthritis, affecting over 32 million adults. Additionally, over 10 percent of patients with knee osteoarthritis seek steroid or hyaluronic acid injections to relieve their pain.
Both studies used cohorts from the Osteoarthritis Initiative, which is a multicenter, longitudinal, observational study that is currently in its 14th follow-up year and includes almost 5,000 participants with knee osteoarthritis.
Steroids can damage several areas of the knee
The study conducted by the UCSF included 210 participants, with 70 receiving intraarticular injections (44 injected with steroids and 26 with hyaluronic acid). The remaining participants didn’t receive any over a two-year span.
All patients underwent MRI scans two years prior to injection, at the time of injection, and after injection. The team assessed their scans using whole-organ magnetic resonance imaging score (WORMS) to detect the severity of their osteoarthritis — examining the meniscus, bone marrow lesions, cartilage, joint effusion, and ligaments.
“This is the first direct comparison of corticosteroid and hyaluronic acid injections using the semi-quantitative, whole organ assessment of the knee with MRI,” says Upasana Upadhyay Bharadwaj, M.D., a research fellow in the Department of Radiology at University of California, San Francisco, in a media release.
They were then able to compare differences in scores between the initial and follow-up scans. Results show that steroid injections significantly influenced arthritis progression, particularly in the lateral meniscus, lateral cartilage, and medial cartilage.
Conversely, hyaluronic acid injections showed no significant relationship to disease progression. In fact, the team found that those who received hyaluronic acid showed the opposite effect. Participants within this treatment group saw a decrease in arthritis progression within bone marrow lesions.
“While both corticosteroid and hyaluronic acid injections are reported to help with symptomatic pain relief for knee osteoarthritis, our results conclusively show that corticosteroids are associated with significant progression of knee osteoarthritis up to two years post-injection and must be administered with caution,” Dr. Upadhyay Bharadwaj reports. “Hyaluronic acid, on the other hand, may slow down progression of knee osteoarthritis and alleviate long term effects while offering symptomatic relief.”
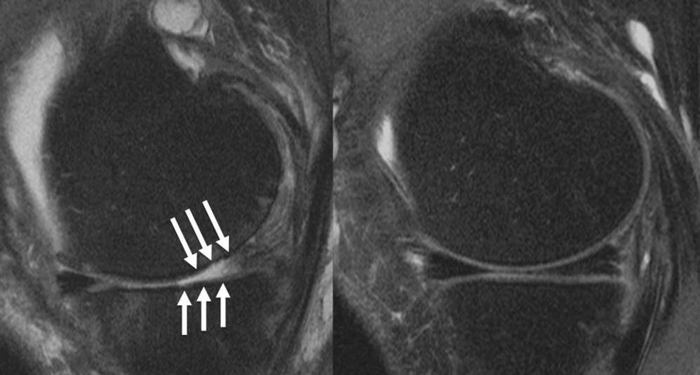
(CREDIT: RSNA and Upasana Upadhyay Bharadwaj, M.D.)
Steroids exacerbated the ‘hallmarks of osteoarthritis’
In the second study, a team from the Chicago Medical School led a case-control study with 150 participants and compared the radiographic progression of osteoarthritis in patients injected with the two treatments. Of those, 50 received steroid injections, 50 received hyaluronic acid, and the remaining 50 did not receive an injection over the 36-month span.
They used X-ray imaging at baseline and a two-year follow-up. Similar to the first study, those who received steroids saw an exacerbation in disease state, specifically in the medial joint space narrowing, which is a telltale sign of the condition.
“Even though imaging findings for all patients were similar at baseline, the imaging hallmarks of osteoarthritis were worse two years later in patients who received corticosteroid injections compared to patients who received hyaluronic acid injections or no treatment at all,” Darbandi said. “The results suggest that hyaluronic acid injections should be further explored for the management of knee osteoarthritis symptoms, and that steroid injections should be utilized with more caution.”
Bharadwaj also adds that this knowledge may help healthcare professionals improve pain management practices for people dealing with painful arthritis in the knee.
The researchers presented their findings at the annual meeting of the Radiological Society of North America (RSNA).







