
The U-RHYTHM device and spool. (Credit: University of Bristol/Designworks Windsor/David Hills (Glude.tv))
BRISTOL, England –– Researchers have developed a pioneering wearable device capable of stress-monitoring by measuring hormones throughout day and night periods painlessly. U-RHYTHM is the first machine ever capable of monitoring stress across a full 24-hour period, including during sleep.
The development of this groundbreaking device may potentially replace the traditional, painful, and time-consuming process of drawing blood to measure stress hormones. This could simplify the identification of stress-related disease symptoms. The team also developed a new reference system aimed at improving the diagnosis and treatment of diseases related to the stress hormone system.
The collaborative research emphasizes the importance of monitoring adrenal steroid levels over extended periods. This approach yields more detailed information regarding hormonal changes over daily (circadian) and faster (ultradian) time periods. Disruption in the rhythms of stress hormones like cortisol is linked with depression, heart disease, obesity, diabetes, and even critical illnesses.
Until now, defining normal, healthy hormonal rhythmicity in daily life has posed a challenge to scientists. Diagnosing based on a single hormonal test taken at one point during the day fails to consider hormonal rhythms, leading to potential diagnostic delays and missed opportunities for early treatment interventions.
In the past, an accurate hormone profile could only be obtained by taking multiple blood samples during a hospital or research unit admission – a process that is inconvenient, stressful, and time-consuming.
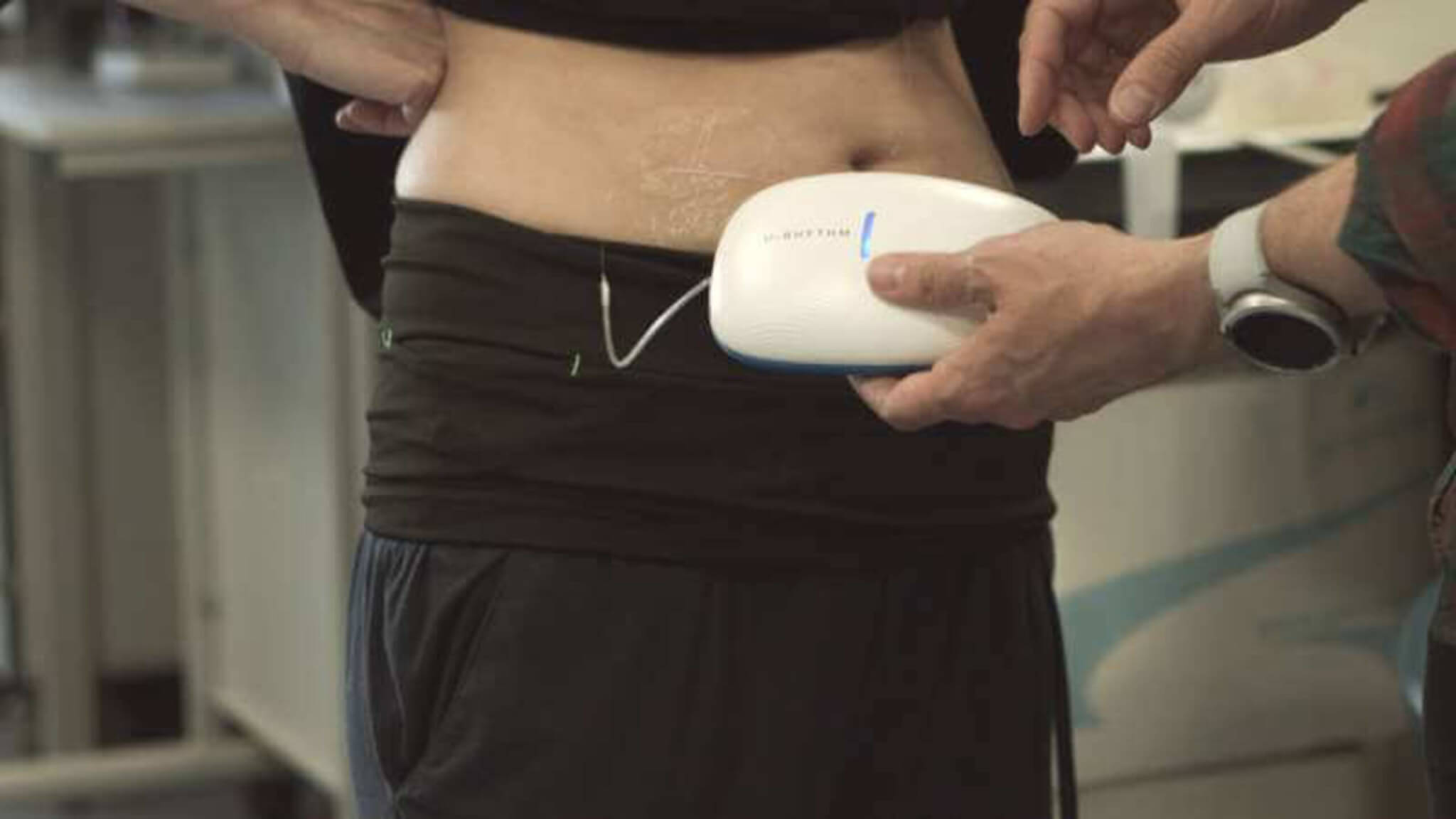
The U-RHYTHM device, a joint effort from the universities of Bristol, Birmingham, and Bergen in Norway, and designed by Designworks Windsor, is worn around the waist. It samples hormones painlessly and automatically from beneath the skin every 20 minutes without the need for blood samples. Remarkably, this method permits sampling during sleep, work, and other daily activities for up to 72 hours in a single session.
The accompanying study demonstrated the device’s effectiveness by analyzing samples from 214 healthy volunteers over a 24-hour period. Using data from multiple time points, the team was able to establish adrenal hormone profiles of healthy individuals in their daily lives.
“The information we have gathered forms an entirely new reference range which has the potential to revolutionize how diseases of the stress hormone system are diagnosed and treated,” says Dr. Thomas Upton, a Clinical Research Fellow in Automated Sampling at the University of Bristol and lead endocrinologist in the study, in a media release. “Our results represent a paradigm shift in the understanding of how the stress hormone system works in healthy people.”
Mathematicians from the University of Birmingham utilized this data to develop a new type of “dynamic markers.” These markers aim to better define what a healthy hormonal profile should look like, taking into account individual characteristics such as sex, age, and BMI. The findings could establish a baseline for improved methods of diagnosing hormonal conditions at earlier stages.
“The ability to measure the dynamics of hormone secretion across the day and night in patients in their own home will not only improve our ability to accurately diagnose any abnormality in hormone secretion without the need for complex inpatient investigations, but the whole diagnostic procedure can be performed from primary care and linked to newly available diagnostic algorithms,” says co-author of the study, Professor Stafford Lightman of Bristol Medical School. “This will not only provide good, personalized medicine, but will also allow the patient to follow their own hormone profiles during diagnosis and therapy and empower better patient: doctor discussions.”
This study is published in the journal Science Translational Medicine.
South West News Service writer James Gamble contributed to this report.







