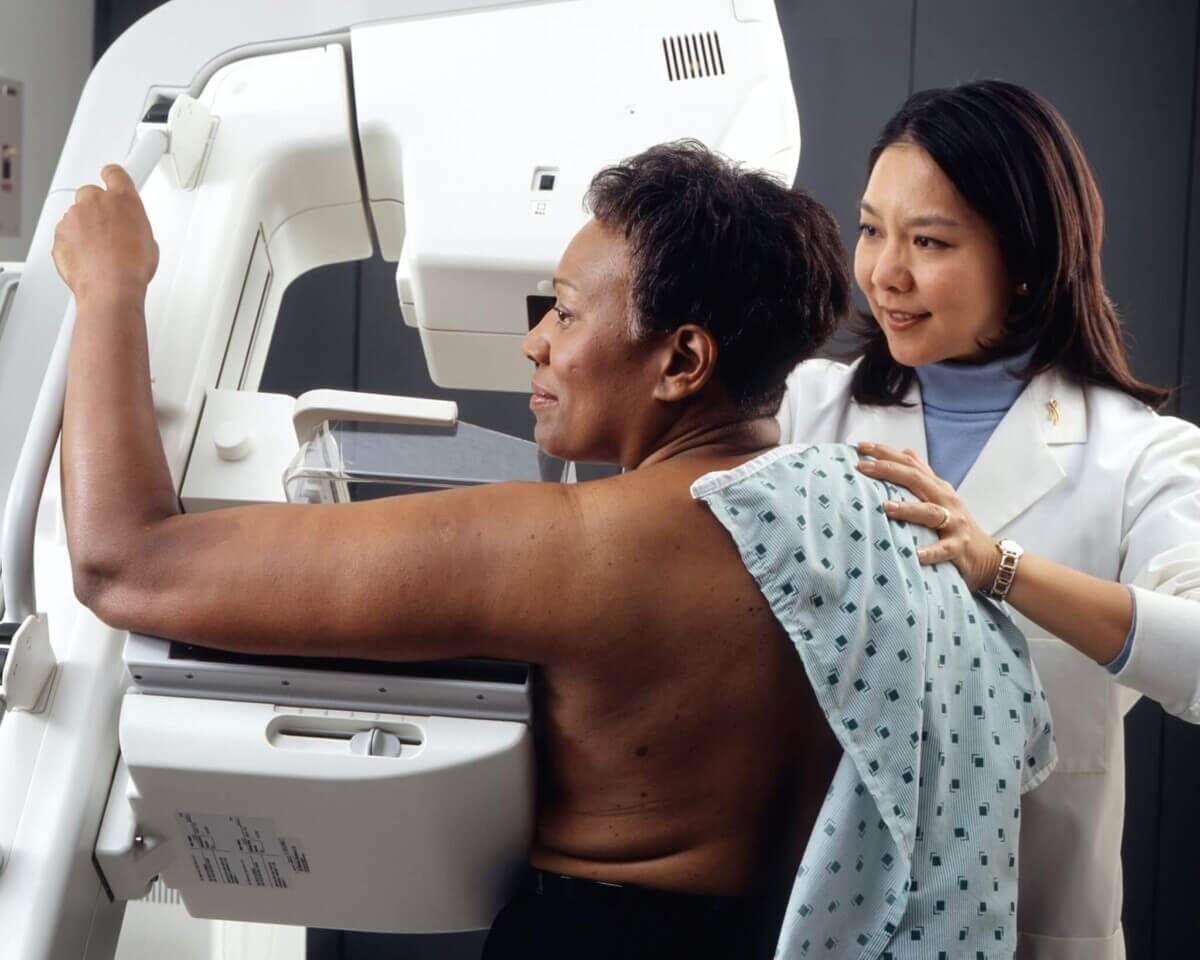
(Photo by National Cancer Institute on Unsplash)
PITTSBURGH — The age-old question of when women should start getting mammograms has just been given a compelling new answer. Researchers from the University of Pittsburgh Medical Center suggest that annual breast cancer screenings should begin at 40, challenging current guidelines and potentially reshaping how we approach early detection.
Published in the Journal of Clinical Oncology, this research provides strong evidence that starting annual mammograms at 40 could lead to earlier cancer detection and improved survival rates. This finding flies in the face of some current recommendations, such as those from the U.S. Preventive Services Task Force (USPSTF), which suggests biennial screenings starting at 50 for most women.
Dr. Margarita L. Zuley and her team analyzed data from over 8,000 women diagnosed with breast cancer between 2004 and 2019. What makes this study particularly noteworthy is its focus on real-world outcomes, examining how different screening intervals affected both the stage at which cancer was detected and long-term survival rates.
“Only about 65% of women over age 40 are screened for breast cancer, and only about half of those women are getting annual screening — in part because of conflicting guidelines about recommended screening intervals,” says Zuley, a professor and chief of the Division of Breast Imaging in the Department of Radiology at Pitt and UPMC, in a statement. “Our study shows that there is a significant benefit for annual screening over biennial screening, including in premenopausal women.”
The researchers divided the women into four groups based on their screening habits: those who got annual mammograms (within 15 months of each other), those who got biennial screenings (15-27 months apart), those with intermittent screenings (more than 27 months apart), and those who only had one screening before their diagnosis.
The results were striking and consistent across all age groups, including women in their 40s. Women who had annual mammograms were significantly less likely to be diagnosed with late-stage breast cancer compared to those who had less frequent screenings. Only 9% of women in the annual screening group were diagnosed with late-stage cancer, compared to 14% in the biennial group and 19% in the intermittent group.
To put this in perspective, imagine a group of 100 women in their 40s getting mammograms. If they all opted for annual screenings, about 9 of them might be diagnosed with late-stage cancer. But if they chose biennial screenings, that number jumps to 14, and with even less frequent screenings, it rises to 19. These differences might seem small, but they translate to thousands of women when applied to the broader population.
The study didn’t stop at analyzing cancer stages; it also looked at overall survival rates. Here, the findings were equally compelling. Women who had annual screenings had significantly better survival rates compared to those who had biennial or intermittent screenings. This survival advantage held true even after accounting for factors like age, race, and menopausal status.
One of the most intriguing aspects of this study is that it challenges the notion that different screening recommendations should apply to different age groups or menopausal statuses. The researchers found that the benefits of annual screening were consistent for both pre and post-menopausal women, starting from age 40.
This is particularly noteworthy because current USPSTF guidelines suggest that women in their 40s should make individual decisions about screening in consultation with their doctors, weighing potential benefits and risks. The Pittsburgh study, however, suggests that these guidelines might be missing an opportunity to catch cancers earlier and save more lives.
Of course, the decision to get a mammogram is not always straightforward. Some women worry about the potential for false positives, which can lead to unnecessary anxiety and additional tests. Others are concerned about overdiagnosis – the detection of cancers that might never have caused symptoms or required treatment.
However, this study emphasizes that these concerns need to be balanced against the very real benefit of catching aggressive cancers early when they are most treatable. The researchers point out that the survival advantage seen with annual screening persisted even after they adjusted their analysis to account for potential lead-time bias – the possibility that earlier detection might appear to improve survival rates simply by finding cancers sooner, without actually changing the course of the disease.
“We recognize that there are potential harms associated with calling women back for additional screening, but I don’t think that these harms outweigh the risk of missing cancers and women dying as a result,” says Zuley. “We’re also working on testing screening tools that have lower false positives than mammography and pushing on every front to identify the most cost-effective and accurate way of taking care of our patients.”
This research comes at a time when breast cancer remains one of the most common cancers affecting women worldwide. In the United States alone, about one in eight women will develop breast cancer in their lifetime. While treatment options have improved dramatically in recent years, early detection remains crucial for the best outcomes.
The study’s findings have implications not just for individual women making decisions about their health care but also for policymakers and insurance companies. If annual screenings starting at age 40 truly offer a significant advantage in terms of earlier detection and improved survival, it could lead to changes in screening guidelines and coverage policies.
As with any medical decision, women should consult with their healthcare providers to determine the best screening schedule for their individual circumstances. Factors like family history, genetic risk, and personal preferences all play a role in these decisions. However, this study provides valuable new information that could help inform those conversations and decisions, especially for women in their 40s who may have been unsure about when to start regular screenings.
“Annual mammograms are crucial for early detection of breast cancer, which increases the likelihood of survival, decreases harms to patients because treatment may not need to be as intense, makes recovery easier and can lower the cost of care,” concludes Zuley.
Paper Summary
Methodology
The researchers analyzed data from 8,145 women diagnosed with breast cancer between 2004 and 2019 who had at least one screening mammogram before their diagnosis. They categorized these women into four groups based on their screening frequency: annual (≤15 months between screenings), biennial (>15 and ≤27 months), intermittent (>27 months), and baseline (only one screening).
They then examined the relationship between screening frequency and two main outcomes: the stage of cancer at diagnosis and overall survival. The study used statistical methods to adjust for factors like age, race, and menopausal status, ensuring that the observed effects were truly related to screening frequency.
Key Results
The study found that women who had annual mammograms were less likely to be diagnosed with late-stage cancer (defined as stage IIB or higher). Only 9% of women in the annual screening group had late-stage cancer at diagnosis, compared to 14% in the biennial group and 19% in the intermittent group.
This trend held true across all age groups, including women in their 40s, and for both pre- and post-menopausal women. In terms of survival, women who had annual screenings had significantly better overall survival rates compared to those with less frequent screenings. Even after adjusting for potential lead-time bias, the survival advantage remained significant.
Study Limitations
First, it’s an observational study, which means it can show associations but can’t prove causation. Second, the data comes from a single healthcare system, which might not be representative of all populations. There’s also a possibility of selection bias, as women who choose annual screenings might have other health-conscious behaviors that could influence outcomes.
Additionally, the study didn’t account for all potential confounding factors, such as overall health status or socioeconomic factors, which could affect both screening frequency and cancer outcomes.
Discussion & Takeaways
This study provides strong evidence supporting annual mammographic screening for women aged 40 and older. It challenges current guidelines that recommend biennial screening for many women and suggests that more frequent screenings from an earlier age could lead to earlier cancer detection and improved survival rates. The consistency of these findings across different age groups and menopausal statuses is particularly noteworthy.
However, the researchers acknowledge that their results need to be balanced against potential harms of screening, such as false positives and overdiagnosis. They call for further research to confirm their findings and to explore the impact of annual screening on these potential downsides.
Funding & Disclosures
The study was supported in part by an award from the National Cancer Institute. The authors disclosed various potential conflicts of interest, including consulting roles, research funding, and stock ownership related to companies in the medical imaging and cancer treatment fields.
However, these disclosures are standard in medical research and don’t necessarily impact the validity of the findings. The transparency in reporting these potential conflicts allows readers to consider the results in context.







