BETHESDA, Md. — Your risk for high blood pressure may have a lot more to do with your genes than scientists previously thought. A new study by the National Institutes of Health has discovered over 100 new regions of the human genome that appear to affect a person’s blood pressure. Specifically, researchers found that these genetic markers explain up to 12 percent of the differences between two people and their individual blood pressure readings.
The findings, published in the journal Nature Genetics, found genetic regions which seem to play a role in iron metabolism as well as a type of cellular receptor known as adrenergic receptors. Since high blood pressure tends to run in families, scientists say this new discovery points to the significance of an individual’s genetic makeup — explaining why they have hypertension and their friend with a similar diet and health history does not.
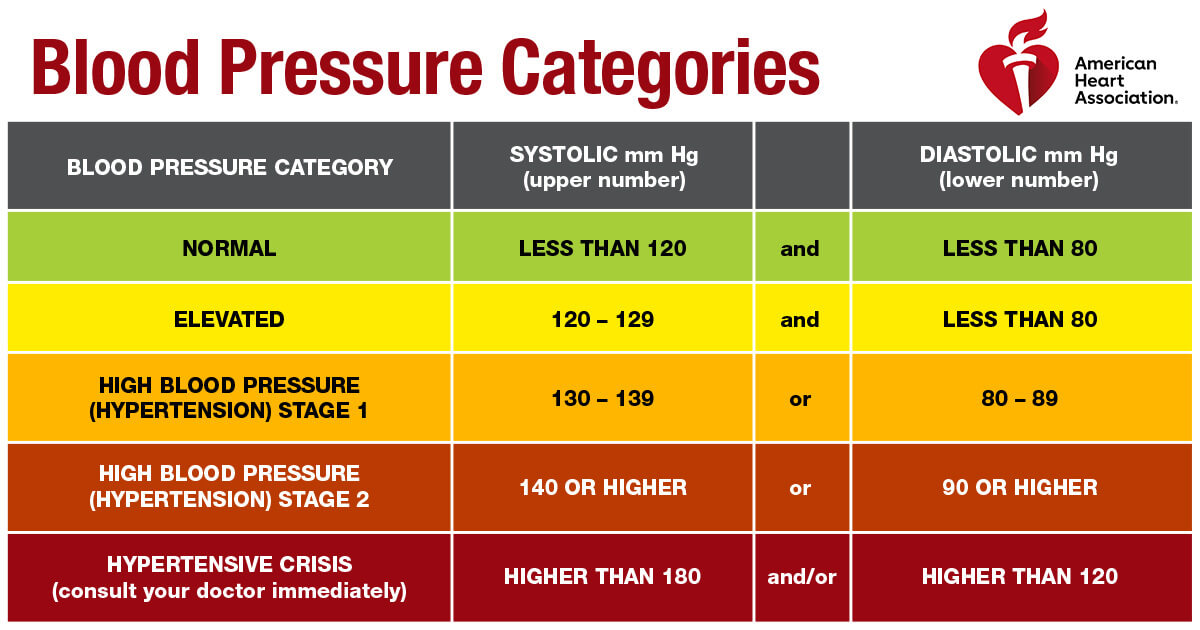
The CDC notes that healthy half of all U.S. adults have high blood pressure. Along with genetic factors, high-salt diets, physical inactivity, smoking, and stress are all contributors to changes in a person’s blood pressure. When these readings are dangerously high, it can lead to severe disease in the kidneys and heart.
The new study is one of the largest to date connecting the human genome to blood pressure, including over a million people. Researchers believe the findings reveal new genetic targets for high blood pressure drugs, possibly helping millions of Americans with hypertension.
“Our study helps explain a much larger proportion of the differences between two people’s blood pressure than was previously known,” says Jacob Keaton, Ph.D., a staff scientist in the Precision Health Informatics Section within the National Human Genome Research Institute’s (NHGRI) Intramural Research Program, in a statement. “Our study found additional genomic locations that together explain a much larger part of the genetic differences in people’s blood pressure. Knowing a person’s risk for developing hypertension could lead to tailored treatments, which are more likely to be effective.”
During the study, researchers at NIH combined four huge collections of data from human genome studies related to blood pressure. Their analysis uncovered over 2,000 genetic regions with a connection to blood pressure. This included 113 regions (genomic loci) that were completely new to scientists.
Those new genomic regions included several which sit inside genes that influence iron metabolism. Previous studies have found that high levels of iron accumulating within the body may lead to cardiovascular disease — one of the main consequences of having hypertension. Finding genetic markers linked to iron metabolism appears to confirm this connection to high blood pressure and the diseases the condition causes.
The study also found a potential link between mutations in the ADRA1A gene and blood pressure. The NIH team explains that ADRA1A encodes adrenergic receptors — a current target of high blood pressure medications. Researchers believe the discovery of other genetic variants in this new study may also be susceptible to drug interventions, a good sign for hypertension patients.
“This study shows that these big genome-wide association studies have clinical relevance for finding new drug targets and are needed to discover more drug targets as we go forward,” Dr. Keaton adds.
New genetic tests for high blood pressure?
The study also used its findings to run genetic exams, which created a polygenic risk score for patients. The scores combined the impact of all these genomic variants to predict someone’s blood pressure and their future risk for hypertension.
Although polygenic risk scores are a promising step towards preventing hypertension, the study authors believe more diverse genetic data is needed before they can become a common tool in your local doctor’s office. However, the study did find that their polygenic risk scores for high blood pressure were still applicable to people of African ancestry despite most of the data in this study coming from people of European ancestry.