The U.S. Food and Drug Administration announced on May 11, 2023, that it has officially dropped restrictions that prohibit gay and bisexual men from donating blood under many circumstances on May 11, 2023. The ban was initially put in place in the early days of the AIDS epidemic, but for years medical professionals and gay rights advocates have argued that the ban was no longer medically justifiable and that it unnecessarily discriminated against men who have sex with men.
Ayako Miyashita is a health policy researcher at the University of California, Los Angeles, who studies HIV treatment and prevention. She explains the history of the ban and the reasoning behind its long-awaited reversal.
1. When and why did the ban begin?
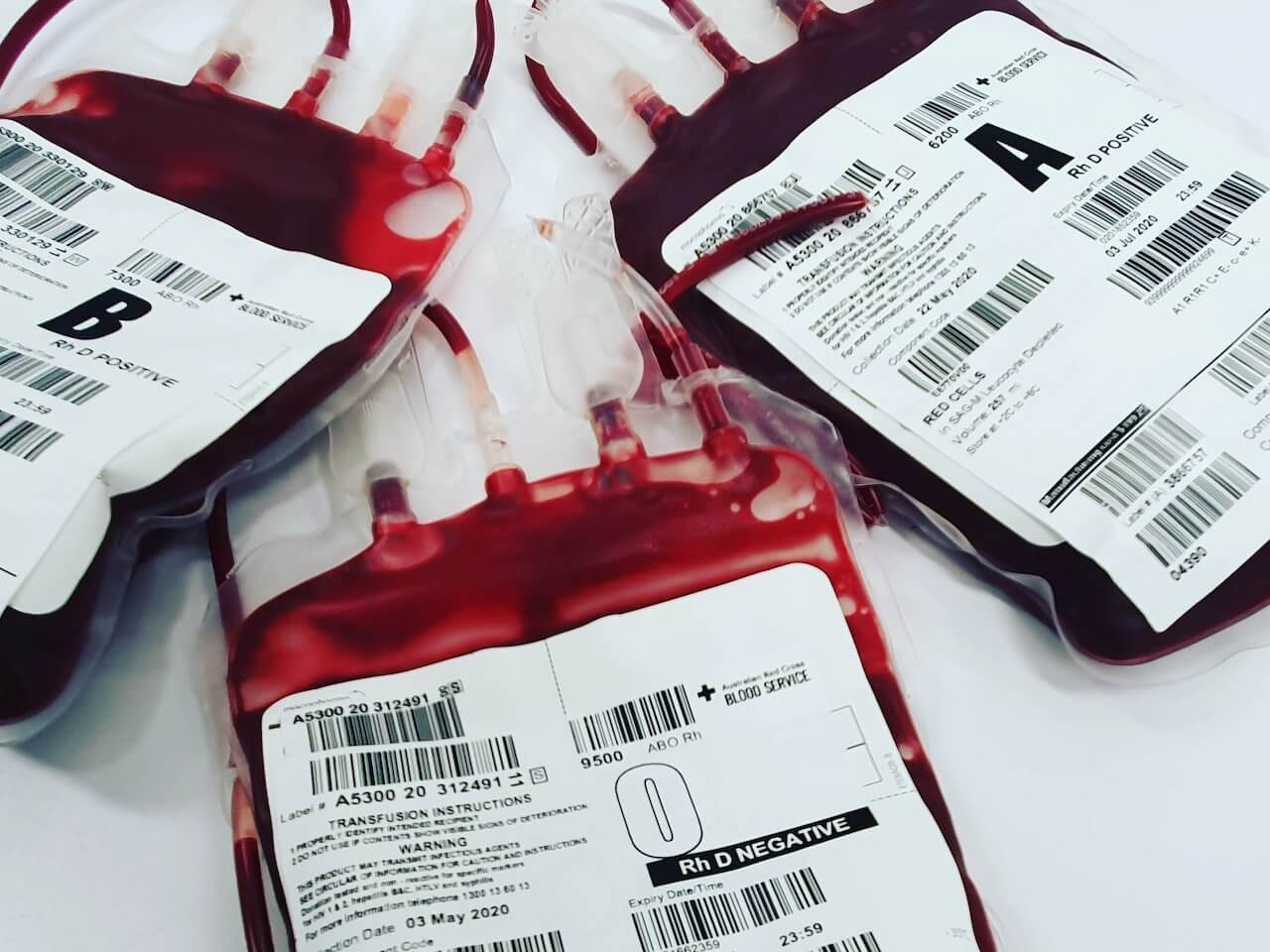
When the FDA first implemented the blood donation ban in 1983 for men who have sex with men, there were good reasons for broad regulations to ensure the safety of the blood supply. At the start of the AIDS epidemic, public health officials were dealing with an unknown virus that was spread through unknown means. Researchers formally identified HIV as the cause of AIDS a year later, in 1984, and it took another year to approve the first test to screen blood donations for HIV in 1985.
Despite the ban on blood donations from men who have sex with men, there was some small risk that failures in donor screening and blood screening protocols could lead to transmission of HIV or other diseases from blood transfusion. But over the years, scientific advancements and strict protocols have helped to nearly eliminate HIV transmission through blood. In fact, the last documented transmission of HIV through the a U.S. donor’s blood product occurred nearly 15 years ago.
Starting in 2013, the U.S. government began implementing a nationwide system to monitor the safety of the U.S. blood supply for a variety of different pathogens, including HIV.
2. Why lift the ban now?
While the blood donation ban – as well as many other laws passed in the 1980s regarding HIV exposure and spread – were reasonable at the time, the science has changed. Researchers and public health officials have gained a better understanding of how HIV is transmitted and the risks associated with different activities. Given today’s knowledge, many medical experts believe that the benefits of the ban no longer outweigh the hit to the blood supply or the harm caused by what is a discriminatory rule.
The FDA has been slowly working toward this change. In December 2015, the organization took a big step by allowing men who have sex with men to donate blood if they hadn’t had sexual contact in one year. That period was further reduced to three months in April 2020, during the height of the COVID-19 pandemic, to help fight a critical blood shortage.
While a step in the right direction, these updates didn’t change the blunt assessment by the FDA that men who have sex with men are performing high-risk sexual behaviors and are themselves high-risk donors. Researchers and gay rights advocates have long argued that time-based deferrals lack nuance and fail to realistically consider the differences in risk associated with the type of sex, type of relationship, number of partners and frequency of sexual encounters.
The FDA’s latest draft recommendations go a long way toward improving clarity about what makes a person a high-risk donor and removes the blanket categorization of prospective donors based on their gender and sexual orientation alone.
Under the new guidelines, there is a way to differentiate between individuals who are monogamous and those who are not, as well as between those who have not engaged in anal sex in the prior three months and those who have. The recommendation now suggests that blood donor history questionnaires be used to evaluate an individual’s risk rather than a reliance on broad categorizations. If the assessment finds an individual to be high-risk, then the guidelines recommend that person be prevented from donating blood for three months.
3. What effect could this have on the blood supply?
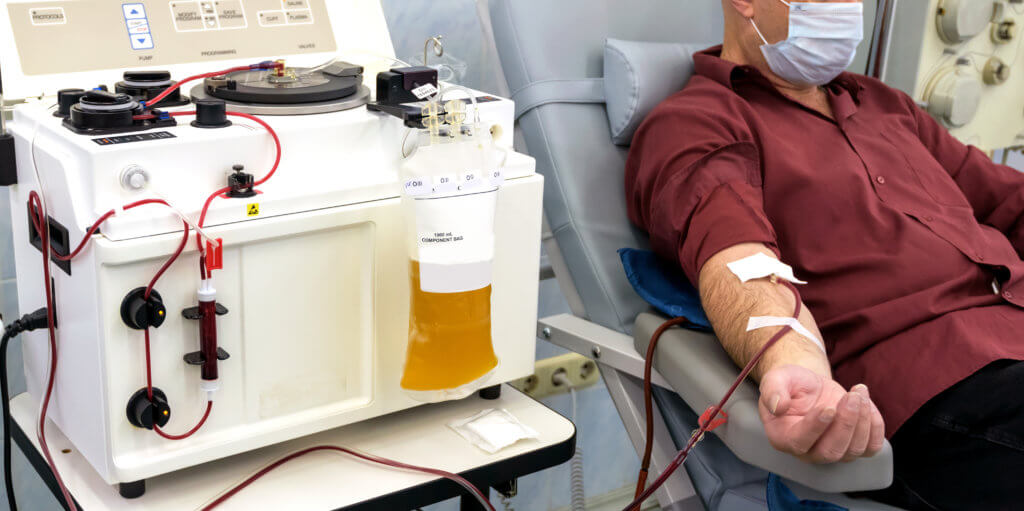
The FDA’s latest move represents a seismic shift for men who have sex with men as well as for the critically low U.S. blood supply.
According to recent research, a conservative estimate suggests that the lifting of the ban will lead to a 2% to 4% increase in the blood supply. With the ongoing blood shortage, that increase could help save more than a million lives. In addition, removing gender and sexual orientation from the risk assessment for blood donation will take the U.S. one step further in addressing stigma and discrimination against men who have sex with men.![]()
Ayako Miyashita, Adjunct Professor of Public Policy and Social Welfare, University of California, Los Angeles
This article is republished from The Conversation under a Creative Commons license. Read the original article.
You might also be interested in:
- Plastic particles found in the human bloodstream for the first time ever
- Universal blood type organs created in groundbreaking procedure, making transplants available for all patients
- Artificial blood for life-saving transfusions one step closer to reality


Absolutely insane policy change, as the policy change literally admits the prime risk of HIV transmission – anal sex. And the group which mostly practices this high-risk sexual activity promiscuously is now given extraordinary deference in becoming donors? No other group is accorded this benefit of a doubt, proving that this was a purely political decision, not a medical one.