ANN ARBOR, Mich. — Should older adults who have fewer years to live continue to get cancer screenings? A new study out of the University of Michigan National Poll on Healthy Aging is exploring that question. Researchers discovered that a significant number of older adults disagree with the inclusion of life expectancy in determining who should get cancer screenings such as mammograms and colonoscopies.
Of those surveyed, 62 percent of individuals between the ages of 50 to 80 opposed using life expectancy as a factor in these decisions.
This goes against a growing trend in actual medical guidelines. These guidelines are crafted by national organizations based on solid medical evidence and are primarily designed to assist healthcare providers in determining when to suggest specific tests to patients. Moreover, these guidelines also influence insurance coverage decisions.
The introduction of life expectancy into these guidelines stems from the increased risks associated with certain screening tests as people age. Additionally, research indicates that individuals need approximately 10 years to fully benefit from early cancer detection.
The poll highlighted that even among individuals categorized as “medical minimizers” — those who typically avoid medical interventions unless absolutely necessary — 57 percent did not support including life expectancy in cancer screening recommendations.
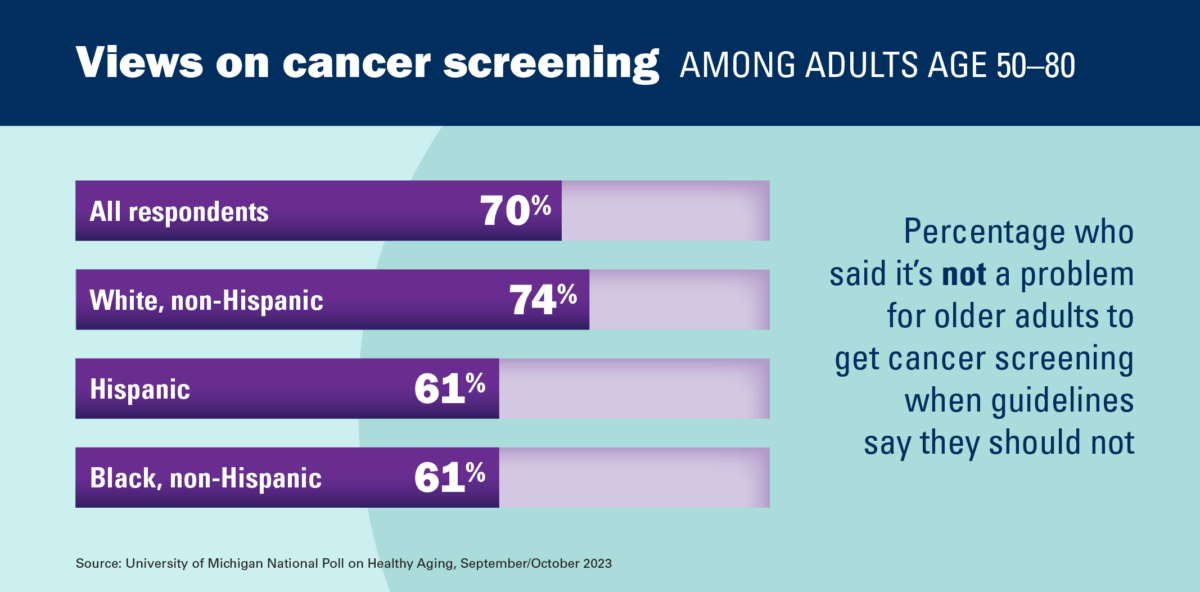
Furthermore, 70 percent of older adults surveyed expressed no issue if their peers underwent cancer screenings, even if guidelines did not advise it. The poll also touched on the 10-year life expectancy guideline, revealing that while 55 percent found it reasonable, 27 percent believed it was too brief.
“Personalizing cancer screening decisions to each patient’s health situation, rather than using one-size-fits-all age cutoffs, could benefit both very healthy and less healthy patients in different ways,” says Dr. Brian Zikmund-Fisher, a healthcare decision-making researcher and professor from the University of Michigan School of Public Health who worked on the poll, in a university release.
Dr. Zikmund-Fisher pointed out that this means talking about an individual’s projected lifespan and sometimes concluding that forgoing a screening could be the healthiest option.
These findings arrive at a crucial time, with an ongoing federal court case that might terminate the mandatory insurance coverage for cancer screenings based on national guidelines.
“Right now, insurance plans must cover the cost of cancer screenings for people in the groups covered by guidelines set by the U.S. Preventive Services Task Force,” explains poll director Dr. Jeffrey Kullgren, an associate professor of internal medicine at Michigan Medicine and physician and researcher at the VA Ann Arbor Healthcare System. “Depending on how the courts eventually rule, insurance coverage of some cancer screenings could end for some older adults, because insurers would be allowed to set their own standards for coverage and not have to abide by guidelines.”
Guidelines may evolve when new data emerges. An upcoming U.S. Preventative Services Task Force draft guideline might reduce the mammogram screening starting age to 40 but still not provide clear evidence for screening women over 75.
Additional insights from the poll include:
- 26% strongly disagreed with the idea of using life expectancy in screening guidelines.
- Strong disagreement was more pronounced among women (30%) than men (21%).
- Strong disagreement about ending screening based on life expectancy was also more common among Black respondents (37%) compared to White (24%) or Hispanic respondents (28%).
- 74% of White respondents were unconcerned if older adults had cancer screenings against their guidelines, whereas this figure was 61 percent for both Black and Hispanic respondents.
The poll included 2,563 adults between the ages of 50 and 80 in January 2023 and reflects the U.S. population.


Cancer treatments and screenings should be used for all people regardless of age
My father lived to be very old and he always took care of his self Every one