QUEBEC CITY, Quebec — For scientists studying degenerative diseases like Alzheimer’s and Parkinson’s, getting the right medication to the brain is the hardest job. Researchers in Canada say they have developed nanoparticles that can successfully bypass all the obstacles which make the brain so difficult to repair. Their study reveals that these particles can deliver drugs to the neurons, which regular treatments can’t reach.
A team from the Institut national de la recherche scientifique (INRS) explains that the blood-brain barrier is the biggest obstacle when treating neurodegenerative diseases. Illnesses like Alzheimer’s expose the brain cells to harmful plaques which interfere with memory and motor function.
While standard drugs which enter through the bloodstream can’t sneak through into the brain, researchers say nanoparticles with specific chemical properties would be ignored by the body’s immune system. “The blood-brain barrier filters out harmful substances to prevent them from freely reaching the brain. But this same barrier also blocks the passage of drugs,” explains pharmacologist Charles Ramassamy in a university release.
Treating the brain usually leads to unintended side-effects
Study authors say normal treatments require high dosages just so a small amount of a particular drug reaches the brain. Unfortunately, this leaves much of the medication in a patient’s blood stream, causing potentially harmful side-effects.
If the symptoms are too intense, some patients may even need to stop their treatments. Switching to nanoparticles, the team finds, would enclose the drug in a protective coating and result in fewer side-effects.
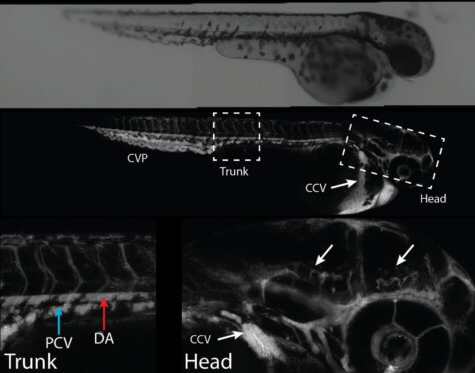
Researchers tested their design using cultured cells and then zebrafish. Previous studies have proven how useful this species can be to human medical research. The small freshwater fish is very similar to humans on a molecular, genetic, and cellular level. It makes them very helpful for comparisons before scientists move on to human trials.
“This species offers several advantages. Its blood-brain barrier is similar to that of humans and its transparent skin makes it possible to see nanoparticles’ distribution almost in real time,” Prof. Ramassamy explains.
Are these nanoparticles safe to inject?
Scientists also made sure to use substances which the human body can break down safely once it delivers a drug to the brain.
“We made the particles with polylactic acid (PLA), a biocompatible material that is easily eliminated by the body. A layer of polyethylene glycol (PEG) covers these nanoparticles and makes them invisible to the immune system, so they can longer circulate in the bloodstream,” the chairholder of the Louise and André Charron Research Chair on Alzheimer’s disease details.
The experiments reveal these PLA/PEG particles can cross the blood-brain barrier within zebrafish, reaching the neurons. The team is now continuing to test their delivery system, using active ingredients housed in the particles. Ramassamy’s group will be testing how successful drug-loaded nanoparticles are on other animals before moving on to clinical trials.
The study appears in the Journal of Controlled Release.
