(© unlimit3d - stock.adobe.com)
PARIS, France — New research suggests that the origins of Alzheimer’s disease may go all the way back to when a patient is still in the womb, where abnormalities in brain development may lay the groundwork for this memory-depriving illness. These findings could potentially lead to a screening program that identifies at-risk individuals at birth.
Although there is currently no cure for Alzheimer’s, increasing attention is being paid to protective lifestyle changes, which include maintaining physical fitness and consuming a diet rich in fish, fruit, and vegetables. Neurodegenerative diseases are generally diagnosed between the ages of 40 and 60. However, it is believed that clinical symptoms emerge several decades after the onset of decline in specific brain cell connections.
A French team of scientists explain that this decline might stem from molecular-scale anomalies present from childhood, or potentially even earlier.
“We were interested in the amyloid precursor protein, or APP, which is highly expressed throughout the development of the nervous system,” says lead author Bassem Hassan of the Paris Brain Institute.
“It is an exciting research target as its fragmentation produces the famous amyloid peptides, whose toxic aggregation is associated with neuronal death observed in Alzheimer’s disease. We, therefore, suspect that APP may play a central role in the early stages of the disease,” Hassan continues in a media release.

In many species, APP is involved in various biological processes, such as repairing cerebral lesions, orchestrating cellular response after oxygen deprivation or controlling brain plasticity.
APP is highly expressed during the differentiation and migration of cortical neurons, which are responsible for functions such as speech and swallowing – functions often compromised by dementia. The complex process of formation from stem cells begins in the fetus from five weeks gestation and is almost complete by 28 weeks.
“In humans, neurogenesis lasts particularly long compared with other species,” explains Khadijeh Shabani, a post-doctoral researcher at Paris Brain Institute. “Neural stem cells remain in a progenitor state for an extended period. Only later do they differentiate into glial cells, astrocytes, or oligodendrocytes that will form the architecture of the brain and spinal cord.”
Until now, it remained unclear how this balance between stem cell proliferation and differentiation into various cell types was regulated. Moreover, it was unknown whether the extended duration of human neurogenesis could potentially contribute to neurodegenerative diseases.
Historically, Alzheimer’s drugs have proved unsuccessful due to their prescription at a stage when the disease has already taken hold. However, this study, published in the journal Science Advances, paves the way for the development of medications that target APP in middle age – or even earlier.
The researchers utilized cell sequencing data from fetuses at 10 weeks and 18 weeks gestation to track APP expression during human brain development. They found that the protein was initially expressed in six cell types and later in 16 types.
By using gene editing to produce neural stem cells lacking APP expression and comparing these modified cells with those from fetuses, the researchers gathered important data.
“This comparison provided us with valuable data,” Shabani explains. “We observed that in the absence of APP, neural stem cells produced many more neurons, more rapidly, and were less inclined to proliferate in the progenitor cell state.”
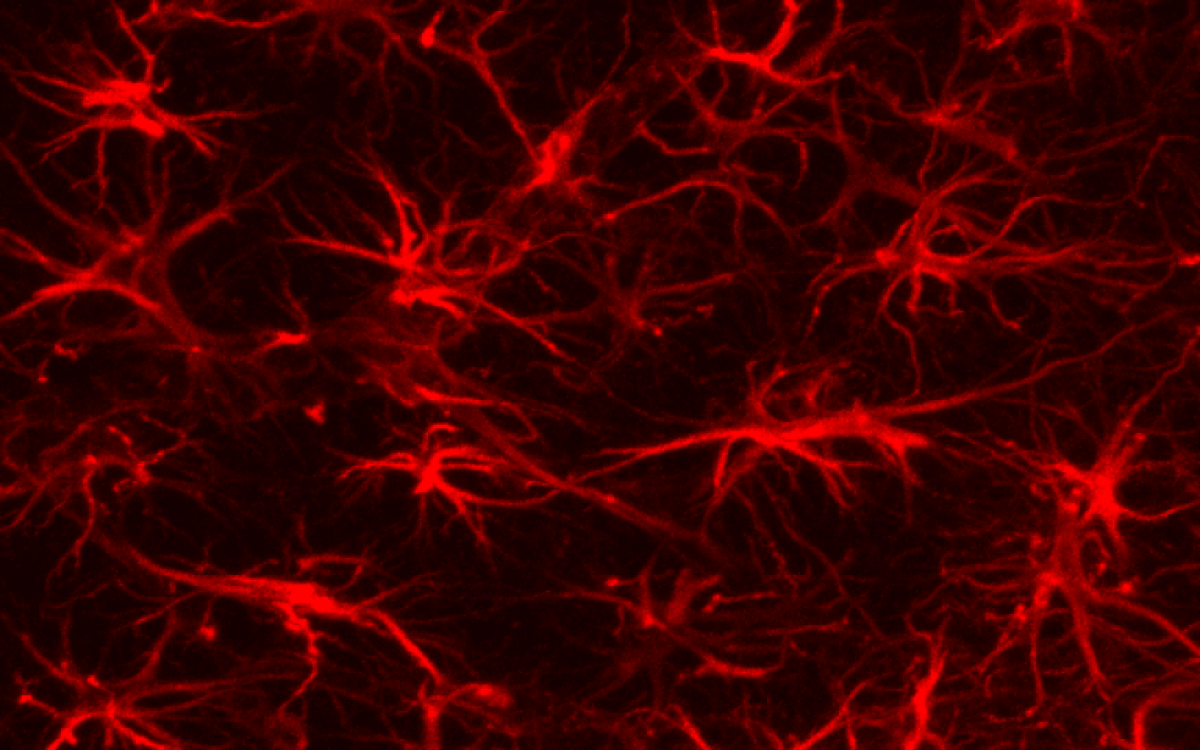
Specifically, APP regulates neurogenesis timing by influencing two finely-tuned genetic mechanisms – one chemical pathway controlling stem cell proliferation and another triggering the production of new neurons.
“In mouse models, neurogenesis is already very fast – too fast for APP deprivation to accelerate it further. We can imagine that the regulatory role of this protein is negligible in mice, while it is essential in the neurodevelopment of our species: to acquire its final form, our brain needs to generate huge quantities of neurons over a very long period, and according to a definite plan. APP-related abnormalities could cause premature neurogenesis and significant cellular stress, the consequences of which would be observable later,” suggests Hassan.
“Moreover, the brain regions in which early signs of Alzheimer’s disease appear also take the longest to mature during childhood and adolescence.”
There could be a direct link between the timing of human neurogenesis and the mechanisms of neurodegeneration. Given that the number of dementia cases worldwide is expected to triple to over 150 million by 2050 due to ageing populations, finding a therapy that targets the root cause is paramount in medical research.
APP appears to play a critical role in this respect, although further studies are necessary to confirm its centrality. Such research could significantly advance our understanding of Alzheimer’s disease and the brain’s development, potentially leading to early identification methods and new treatments.
The Paris Brain Institute team’s findings have added a crucial piece to the Alzheimer’s puzzle. This work suggests a paradigm shift in our understanding, positioning the disease’s origins much earlier in life than previously assumed. If their hypothesis holds true, we may be able to detect those at risk at a much earlier stage, offering the potential for targeted preventative measures and therapies.
In a world where Alzheimer’s cases are set to skyrocket, the implications of this research are vast and could significantly alter our approach to tackling this debilitating disease. The promise of a therapy that intervenes at the cause, rather than just managing symptoms, represents a “holy grail” in medical research. With Alzheimer’s’ seeds potentially sown in the womb, this research offers a new understanding that could bring us closer to achieving this goal.
“These disturbances lead to the formation of a brain that functions normally at birth but is particularly vulnerable to certain biological events – such as inflammation, excitotoxicity or somatic mutations – and certain environmental factors such as a poor diet, lack of sleep, infections, etc.,” the study authors conclude.
“Over time, these different stresses could lead to neurodegeneration – a phenomenon specific to the human species and made particularly visible by the increase in life expectancy.”
You might also be interested in:
- What the world looks like to someone living with dementia: Photos show distorted reality, even in own home
- Children are constantly ingesting microplastics — even in the womb, study reveals
- New FDA-approved drug may revolutionize Alzheimer’s treatment
South West News Service writer Mark Waghorn contributed to this report.







