JACKSON, Miss. — Alzheimer’s disease robs sufferers of their memory and families of loved ones well before they die. There is no cure, but prevention techniques can certainly help delay the onset and severity of symptoms. Now there may soon be a way for people genetically at risk to tackle the condition farther in advance than ever before. Scientists have developed a simple new blood test could diagnose Alzheimer’s disease decades before symptoms develop.
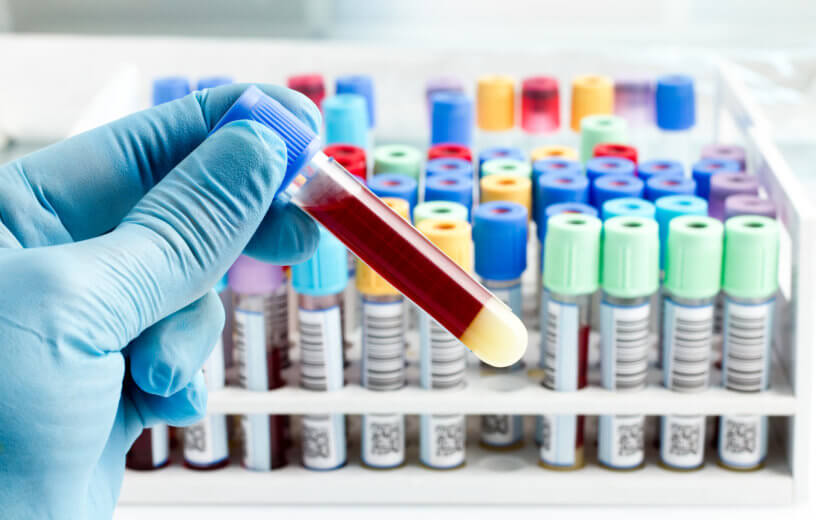
Currently, the only way to detect amyloid beta, the toxic protein viewed as the hallmark signature of Alzheimer’s, is through costly PET scans or invasive spinal tap procedures. The Alzheimer’s blood test could lead to a screening program, enabling medications and lifestyle changes to be prescribed to vulnerable individuals. One of the reasons drug trials have failed is they are given to patients once the condition has already taken hold.
“Right now we look at levels in the central nervous system as a biomarker of Alzheimer’s,” explains lead author Dr. Kevin Sullivan, of the University of Mississippi Medical Center, per South West News Service. “But the only way to do that is through brain scans or looking at the cerebrospinal fluid via a lumbar puncture. These new results suggest there is utility in using simple blood draws that would be less expensive and much less invasive for people.”
Sullivan and his team looked at two types of amyloid beta — known as Aβ42 and Aβ40 — and the ratio between the two. Every 67 picogram per milliliter (pg/mL) rise in the latter increased the risks of dementia or mild cognitive impairment (MCI) by 15 percent. On the other hand, every 10 pg/mL increase reduced them by 13 percent.
A lower ratio of Aβ42 to Aβ40 also increased the risk of dementia and MCI.
“A doubling of this ratio under this threshold at midlife was associated with a 37% lower risk of MCI or dementia, which is comparable to about five years of younger age, and a doubling of this ratio under this threshold at late life was comparable to about three years younger age,” notes Sullivan. “Amyloid in the blood may be useful as a biomarker for risk of future cognitive impairment.”
Midlife Alzheimer’s blood test could help prove future predictions wrong
In the study, 2,284 men and women with an average age of 59 were tracked for 25 years. Blood samples were analyzed at the start (the midlife test) and then again in late life, when they were about 77. The participants did not have problems with memory or thinking skills at the outset.
Mental tests showed 502 and 832 went on to develop dementia and MCI, respectively.
The study, published in the journal Neurology, took into account age, education and cardiovascular risk factors.
As the brain engages in daily tasks, it continually produces and clears away amyloid beta, which can stop brain cells functioning properly. Some is washed into the blood, and some floats in the cerebrospinal fluid, which is why spinal taps are used. If the protein starts building up, it can collect into plaques that stick to neurons, triggering permanent damage.
They are composed mainly of amyloid beta 42, meaning it is probably being deposited in the brain before moving into the blood.
In the U.S., about 6 million people are currently living with Alzheimer’s. It’s believed that number will balloon to 13 million by 2050, according to the Alzheimer’s Association. One recent study predicts that dementia cases worldwide will triple by that year.
South West News Service writer Mark Waghorn contributed to this report.