
(© vegefox.com - stock.adobe.com)
CHARLESTON, S.C. — Neuroscientists from the Medical University of South Carolina have successfully identified subtle differences in the way the brain functions in older adults during the early stages of Alzheimer’s disease (AD), using novel brain imaging. In a sense, researchers say each person has unique “fingerprints” in their brain which they can now use to spot signs of cognitive decline.
People with Alzheimer’s in its preclinical state (or early stages) show a buildup of amyloid-beta proteins in their brains, which is usually the telltale sign of the disease. Things often get hazy for patients before an official diagnosis and treatment because this buildup could be present without a sign of actual cognitive decline. However, it’s difficult to study the very preliminary changes that the brain undergoes in the beginning of AD onset, which is why so much remains unknown about the condition. This is why new, innovative ways to study the brain (like what the researchers in this study are doing) is imperative for understanding how Alzheimer’s develops.
Scientists mapped out the brain’s ‘inner city’
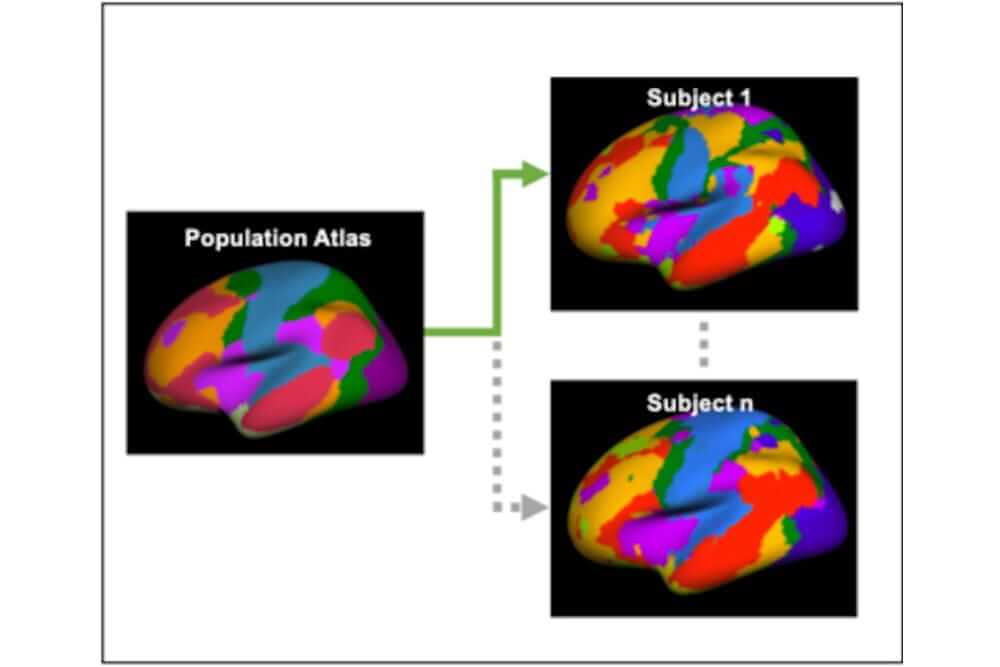
In this pilot project, researchers used individualized maps of brain function that measure how different brain regions communicate with each other. Called a functional connectome, the technology allows researchers to view the brain like a big city, and watch different activities happen throughout that city.
“Prior studies have not found an association between brain function and behavior in preclinical AD,” says study leader Andreana Benitez, Ph.D., in a media release. “Using these individualized maps of brain function, we found a potential brain-based reason for very subtle cognitive changes in this early phase of the disease.”
“We all have the same functional parts of our brain, but they’re positioned slightly differently, sort of like a fingerprint,” adds study co-leader Stephanie Fountain-Zaragoza. “This method creates an individualized brain fingerprint that more accurately reflects where the different functional regions are in each individual’s brain.”
Do Alzheimer’s patients have overactive brains?
The team studied the brains of 149 adults between 45 and 85 who did not have signs of cognitive decline. All participants underwent PET scans of their brains, with the team dividing them according to their results (evidence of early amyloid-beta protein buildup or not). They also underwent MRI scans in order to generate their unique brain fingerprint.
The researchers found that in those with preclinical Alzheimer’s, information processing worsened, which the team attributed to overactivity in their brains. Processing was better in those with calmer brain connectivity, or more contained brain activity within important places or “networks.”
“A healthy brain typically has a balance of connectivity within and between its networks,” explains Fountain-Zaragoza. “We found that in preclinical AD—when amyloid build-up is present in the brain—this balance can be disrupted, potentially leading to information no longer being processed as efficiently.”
Luckily, Benitez and Fountain-Zaratoga don’t have to stop their work here. The team has more grant funding, thanks to the National Institute on Aging, to continue their studies of preclinical Alzheimer’s. They plan to narrow their focus to just how these brain changes affect how the disease runs its course. They also want to look into new treatment options like brain stimulation.
The findings appear in the journal Brain Connectivity.







