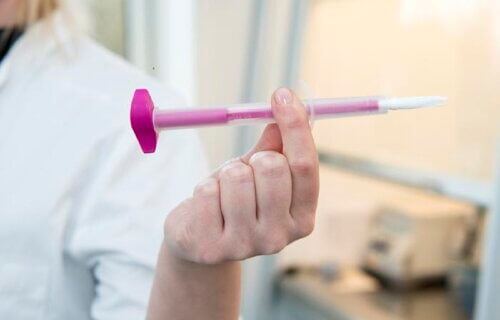
RANDERS, Denmark — A recent study suggests that conducting HPV tests for women over the age of 65 could aid in preventing cervical cancer. Human Papillomavirus (HPV) screenings check for infection and potential cancerous cells.
During the screening, a small sample of cells from the cervix is collected for testing. Although HPV is a common group of viruses that often causes no problems, certain types can lead to cancer, making the test critical for cervical cancer prevention. However, a large number of women over 65 have never undergone a test.
The recent study focused on women between 65 and 69 in Denmark who had no record of cervical cancer screening in the previous five-and-a-half years and no record of an HPV test between ages 60 and 64. Denmark provides a free cervical cancer screening program for women up to the age of 64.
Over 11,000 eligible women residing in one region of Denmark were invited to participate in HPV-based cervical cancer screenings. They had the option of booking an appointment with a doctor or ordering a vaginal self-sampling kit. Additionally, over 33,000 women in the remaining regions of Denmark were invited to form a control group. Although these women did not receive a screening invitation, they could still opt for an opportunistic cervical cytology sample collection.
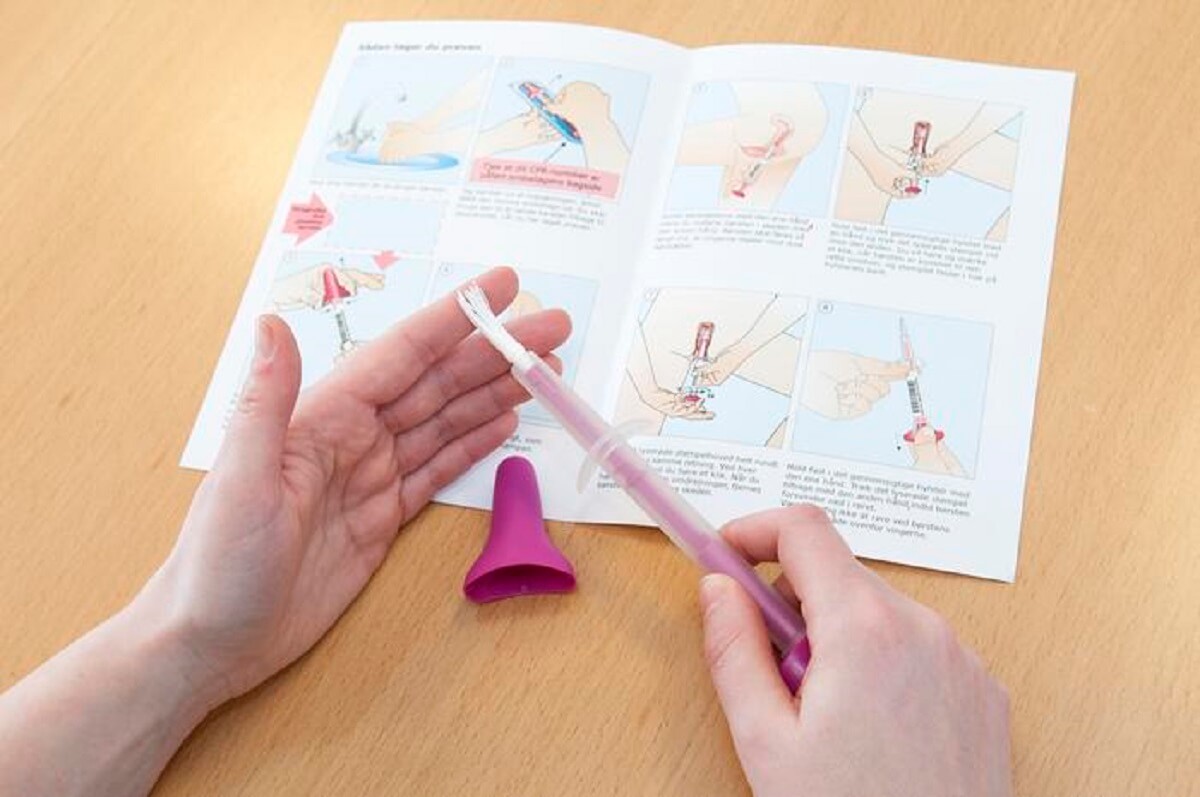
(credit: Helle Brandstrup Larsen (CC-BY 4.0, https://creativecommons.org/licenses/by/4.0/))
Cervical intraepithelial neoplasia (CIN) rates were tracked for all participants for at least 13 months. CIN, often caused by specific types of HPV, is a precancerous condition that can potentially evolve into cancer and spread to nearby tissues.
The study finds that 62.2 percent of the women in the intervention group, nearly 7,000, underwent screening within 12 months, while only 2.2 percent in the control group had a cervical cytology sample collected. The detection rate for CIN grade two or worse (CIN2+) was notably higher in the intervention group than in the control group.
The researchers discovered that women who had not been screened adequately at ages 50 to 64 had a higher likelihood of carrying HPV and more CIN2+ lesions compared to women who had been sufficiently screened. These insufficiently screened women were also more likely to opt for vaginal self-sampling, suggesting this method could be more appropriate for older women.
“A catch-up HPV screening test could potentially improve cervical cancer prevention in women aged 65 years and older who have never had an HPV test,” says Dr. Mette Tranberg, from the University Research Clinic for Cancer Screening at Randers Regional Hospital in Denmark, in a media release. “Older insufficiently screened women were more likely to self-collect a vaginal sample for HPV testing in their own home as compared to sufficiently screened women; hence this screening modality could be ideal to identify older women at risk of cervical cancer.”
The study is published in the journal PLoS Medicine.
South West News Service writer Alice Clifford contributed to this report.