
(© Casimiro - stock.adobe.com)
VANCOUVER, British Columbia — Historically quite difficult to recognize in its beginning stages, new research indicates there may be a new way to help identify early-stage multiple sclerosis (MS). Scientists at the University of British Columbia report MS patients are nearly twice as likely to experience mental illness in the years leading up to the onset of their disease.
More specifically, study authors found that psychiatric conditions including anxiety and depression may be associated with a prodromal phase of MS, considered the “precursor” set of preliminary symptoms and clues that appear just before classic MS symptoms materialize.
Multiple sclerosis is an especially awful chronic autoimmune disease of the central nervous system that essentially causes the body to attack itself. Even worse, symptoms vary greatly from person to person. Some may only experience mild symptoms like numbness or dizziness while others completely lose their capacity to see, walk, or speak. So, recognizing and diagnosing MS is usually a challenge for doctors because related symptoms vary so widely and are often mistaken for other conditions. For the patients themselves, this can mean enduring months and even years of symptoms before even being diagnosed.
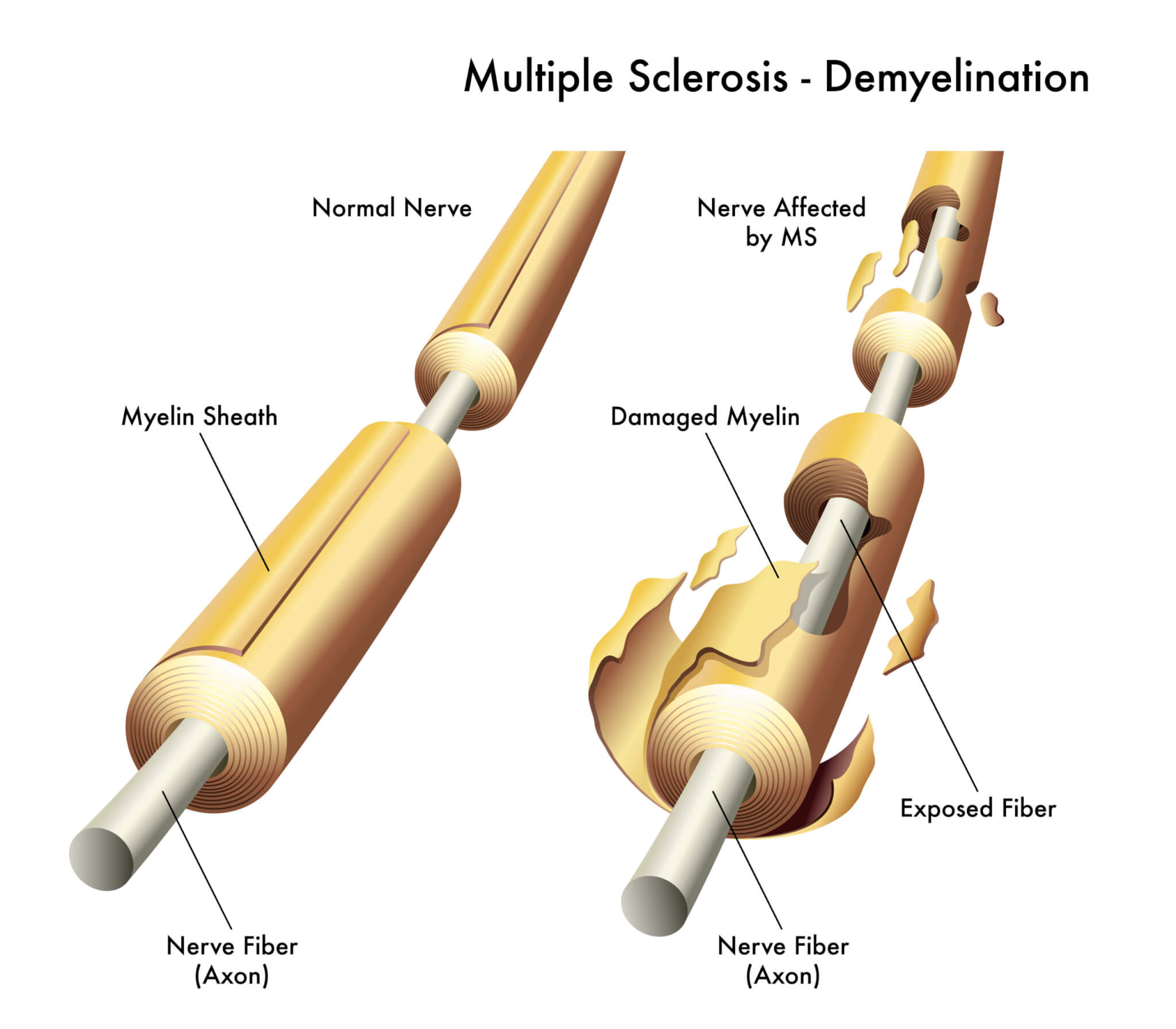
Much of MS is centered on myelin, or the fatty tissues that encase and protect our nerve fibers. In MS patients, myelin is often destroyed in various places. Eventually, that missing myelin leads to scar tissue known as sclerosis. The damage to nerves caused by all of this impedes essential electrical impulses from traveling to and from the brain.
“For a long time, it was thought that MS only really began clinically when a person experienced their first demyelinating event, such as in the form of vision problems,” says senior author Dr. Helen Tremlett, professor of neurology at UBC and member of the Djavad Mowafaghian Centre for Brain Health, in a media release. “But we’ve come to understand there is a whole period preceding those events where the disease presents itself in more indirect ways.”
Dr. Tremlett and her team have been working to better characterize the early stages of MS for some time, with their endgame hopefully being the facilitation of earlier detection and possible intervention. Prodromal periods are well established for other diseases, such as Parkinson’s, in which patients deal with symptoms such as constipation for years before classical motor deficiencies appear.
“If we can recognize MS earlier, treatment could begin sooner. That has tremendous potential to slow disease progression and improve quality of life for people,” Dr. Tremlett adds.
To research this topic, the study authors assessed the health records of 6,863 MS patients in British Columbia. Researchers focused specifically on the rate of mental health conditions (depression, anxiety, bipolar disorder, schizophrenia) during the five years before patients developed classical, medically recognized signs of MS. These MS patients were compared to a control group of 31,865 people without MS.
The results revealed MS patients (28%) were experiencing mental illness at close to twice the rate of the general population (14.9%). Healthcare usage for psychiatric symptoms, such as visiting a physician or psychiatrist, prescriptions, and hospitalizations, was also consistently higher among MS patients. It’s important to note, as well, that this observed gap widened in each of the five years leading up to disease onset.
“We see higher and higher rates of psychiatric conditions that peak in the final year before MS onset,” explains first study author Dr. Anibal Chertcoff, who conducted the study as a postdoctoral fellow in Dr. Tremlett’s lab and is now an assistant professor at the University of Manitoba. “While we’re not suggesting that these conditions alone can be a predictor of MS, they may be one piece of the MS prodrome puzzle and a potential signal when combined with other factors.”
This work actually builds on an earlier project conducted in Dr. Tremlett’s lab that found other symptoms such as fatigue, sleep disorders, irritable bowel syndrome, anemia, and pain may also be included in the MS prodrome.
Sharon Roman, who has lived with MS for 25 years, says that better defining this prodromal period could have huge benefits for countless patients.
“We take many things in life for granted — walking, balance, vision, speech, even the simple act of swallowing — until one day it’s taken from us by MS,” Roman explains. “The better we can identify the early signs and symptoms of MS, the earlier we can recognize, diagnose and treat it. We can help prevent people from being diagnosed the way I was, with a massive attack and hospitalization, and prevent the losses I’ve experienced. Earlier treatment may help slow progression.”
The study is published in the journal Neurology.







